Call PhD Dental Today for Exceptional Dental Care
BOOK AN APPOINTMENTLos Angeles Periodontists
Gum health plays a critical role in protecting your teeth, jawbone, and overall oral stability, yet periodontal issues often develop slowly before symptoms become obvious. Patients searching for Los Angeles periodontists are often dealing with gum inflammation, bone loss, or concerns that extend beyond routine dental care. Periodontal treatment focuses on diagnosing and managing conditions that affect the supporting structures of the teeth, with the goal of preserving oral health over the long term.
At PhD Dental, care from our Los Angeles periodontists is centered on precision, education, and thoughtful treatment planning. Our team addresses both early and advanced periodontal concerns using modern techniques designed to control infection, support healing, and protect natural teeth whenever possible. Every visit emphasizes clear explanations and coordinated care so patients understand their condition and the options available to them. If you have been referred for periodontal care or are concerned about your gum health, call (323)269-5437 to speak with PhD Dental or visit our contact page to schedule a consultation and take the next step toward protecting your oral health.
Top-Rated Dentists
in Los Angeles
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
- When Gum Health Issues Require Los Angeles Periodontists
- Conditions Treated by Los Angeles Periodontists
- How Periodontal Health Is Evaluated Beyond Routine Dental Exams
- How Los Angeles Periodontists Structure Treatment Plans for Long-Term Stability
- How Los Angeles Periodontists Carry Out Treatment in Complex Cases
- How Periodontal Care Supports Bone and Gum Regeneration
- The Role of Periodontal Maintenance After Regenerative Treatment
- Why Patients Choose PhD Dental's Los Angeles Periodontists
- Schedule an Appointment With PhD Dental's Los Angeles Periodontists Today
When Gum Health Issues Require Los Angeles Periodontists
Gum conditions often develop gradually, making it difficult for patients to recognize when routine dental care is no longer sufficient. Symptoms that seem mild or intermittent frequently reflect deeper changes affecting the gums and supporting bone beneath the surface. Evaluation by our Los Angeles periodontists allows these issues to be identified before they lead to irreversible damage, tooth instability, or long-term oral health complications.
Periodontal concerns differ from general dental problems because they involve the structures responsible for anchoring teeth in place. As inflammation progresses, damage can extend below the gumline in ways that cannot be resolved through standard cleanings alone. Understanding when specialized periodontal care is appropriate helps patients take timely steps toward protecting their oral foundation and preserving natural teeth.
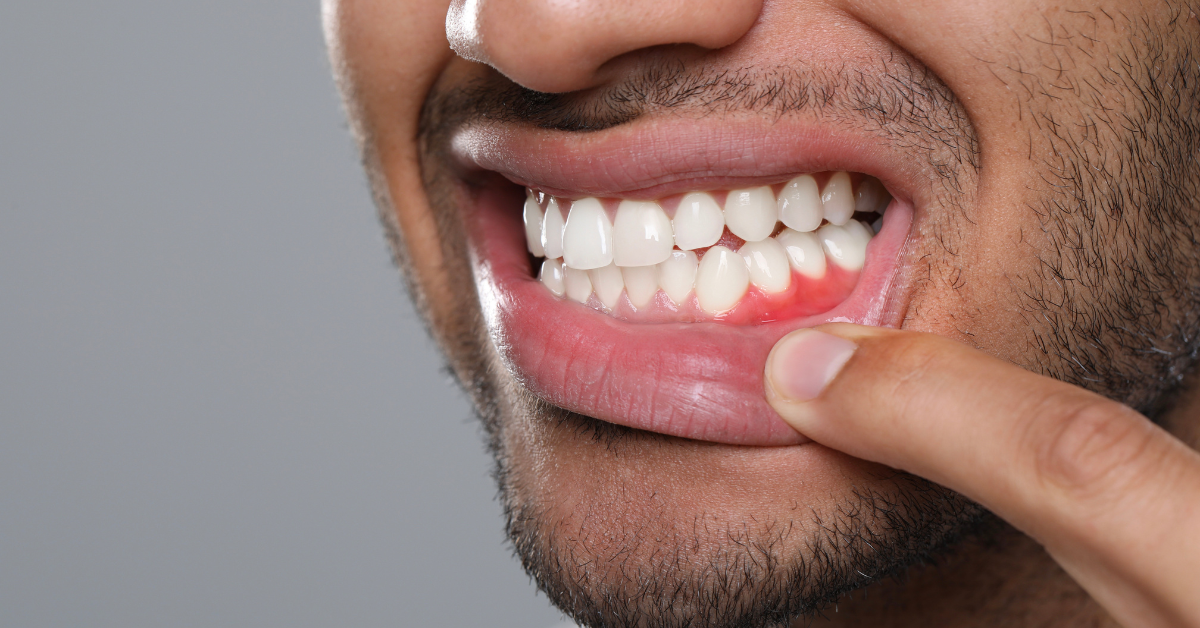
Persistent gum bleeding and inflammation often signal active infection beneath the gumline rather than temporary irritation caused by brushing or flossing habits. These symptoms indicate that bacteria have accumulated in areas that daily oral hygiene cannot adequately reach, allowing inflammation to continue unchecked. Over time, this inflammatory response can weaken the attachment between the gums and teeth, increasing the risk of tissue breakdown and bone loss. Ignoring ongoing bleeding may allow periodontal disease to progress silently, even when pain is minimal or absent.
Why Bleeding Gums Signal More Than Surface Irritation
When bleeding continues despite consistent oral hygiene, it reflects inflammatory changes occurring within the deeper gum tissues. This inflammation disrupts the natural seal between the gums and teeth, creating pockets that harbor additional bacteria. Periodontal evaluation focuses on measuring pocket depth and assessing tissue response to determine disease severity.
How Early Periodontal Assessment Helps Control Infection
Early assessment allows infection to be addressed before it spreads further into the supporting bone. Targeted periodontal treatment reduces bacterial load and helps stabilize inflamed tissues. This proactive approach supports healthier healing and lowers the risk of progressive structural damage.
Gum recession exposes the roots of the teeth, often leading to heightened sensitivity and increased vulnerability to decay. This process typically occurs slowly, making it easy for patients to overlook until discomfort becomes more pronounced. As gums recede, protective tissue is lost, and underlying structures become more susceptible to damage. Without evaluation, recession can continue to progress, affecting both appearance and long-term tooth support.
How Recession Affects Tooth and Bone Support
As gum tissue recedes, exposed tooth roots lose the protection once provided by healthy gums. This exposure increases the risk of root decay and can coincide with underlying bone loss. Periodontal assessment helps determine the extent of tissue and bone involvement and identify contributing factors.
Why Addressing Recession Early Supports Long-Term Stability
Early intervention can slow or stop further tissue loss and help preserve remaining gum structure. Periodontal care may reduce sensitivity and protect exposed root surfaces. Addressing recession early supports tooth stability and long-term comfort.
Changes in bite alignment or a sensation that teeth are shifting often indicate underlying support loss. As periodontal disease advances, bone deterioration can alter how teeth fit together and distribute biting forces. These changes may occur gradually, making them difficult to notice until functional issues arise. Evaluation becomes important when teeth feel loose, spacing changes appear, or chewing comfort declines.
How Bone Loss Can Affect Tooth Positioning
Supporting bone maintains tooth alignment and bite balance. When bone loss occurs, teeth may shift or lose stability, affecting overall function. Periodontal assessment focuses on identifying areas of bone deterioration and evaluating how these changes influence tooth positioning.
Why Prompt Evaluation Helps Prevent Further Movement
Identifying bone-related changes early allows steps to be taken to stabilize affected teeth. Periodontal treatment aims to control disease activity and preserve remaining support. Early care reduces the likelihood of continued tooth movement or bite disruption.
Conditions Treated by Los Angeles Periodontists
Periodontal care focuses on conditions that affect the gums, connective tissues, and underlying bone that support the teeth. These conditions often progress gradually and may not cause immediate discomfort, which can delay treatment until structural damage has already begun. Evaluation by Los Angeles periodontists centers on identifying how deeply the disease has affected the supporting structures and how that progression may influence long-term tooth stability. Periodontal conditions exist on a spectrum, meaning treatment recommendations vary based on severity, rate of progression, and individual risk factors. Understanding these conditions helps patients recognize why specialized periodontal care may be necessary rather than routine dental treatment alone.

Gingivitis represents the earliest stage of periodontal disease and is limited primarily to inflammation of the gum tissue. At this stage, symptoms may include redness, swelling, and bleeding during brushing or flossing, yet irreversible bone loss has not occurred. The absence of pain often leads patients to underestimate the seriousness of the condition. Without proper intervention, gingivitis can progress into more advanced periodontal disease that affects deeper tissues. Early identification plays a critical role in preventing that progression.
How Early Gum Inflammation Develops Beneath the Surface
Bacterial plaque accumulates along the gumline and triggers an inflammatory response within the soft tissue. When plaque hardens into tartar, it becomes difficult to remove through daily oral hygiene. This buildup allows inflammation to persist and creates an environment that supports disease progression.
Why Early Periodontal Evaluation Can Prevent Progression
Early evaluation helps determine whether gum inflammation remains reversible. Targeted periodontal care can reduce bacterial load and restore healthier tissue conditions. Addressing disease at this stage significantly lowers the risk of bone loss and long-term complications.
As periodontal disease advances, inflammation extends below the gumline and begins to affect the bone that supports the teeth. This stage often involves periodontal pocket formation, gum recession, and measurable bone loss. Teeth may begin to feel loose or appear to shift as structural support weakens over time. Changes may also occur gradually, making them difficult to notice without professional evaluation. Advanced periodontitis requires careful assessment to determine the extent of damage and appropriate treatment approach.
How Bone Loss Alters Tooth Stability and Function
Supporting bone anchors teeth during chewing and biting forces. When bone deteriorates, teeth lose stability and may migrate or loosen. Periodontal assessment focuses on identifying affected areas and evaluating how bone loss impacts overall function.
Why Advanced Disease Requires Specialized Periodontal Care
Once bone loss occurs, treatment becomes more complex and targeted. Periodontal care aims to control infection and limit further breakdown. Specialized intervention helps stabilize remaining support and slow disease progression.
Gum recession occurs when gum tissue pulls away from the teeth, exposing root surfaces that lack protective enamel. This exposure increases sensitivity and raises the risk of decay and structural damage. Recession often develops gradually, making early changes easy to overlook. Over time, exposed roots can compromise both comfort and appearance. Periodontal evaluation helps determine the cause and severity of tissue loss.
How Recession Affects Both Comfort and Oral Health
Exposed roots respond more strongly to temperature changes and bacterial activity. This vulnerability can lead to discomfort and increased decay risk. Periodontal assessment evaluates tissue thickness and attachment levels to guide care decisions.
Why Managing Recession Supports Long-Term Tooth Preservation
Early management helps protect exposed root surfaces from further damage. Periodontal treatment may reduce sensitivity and slow tissue loss. Preserving gum structure supports long-term comfort and tooth retention.
How Periodontal Health Is Evaluated Beyond Routine Dental Exams

Routine dental exams focus primarily on tooth surfaces and visible gum conditions, but periodontal evaluation requires a deeper level of assessment. Periodontal health involves the tissues and bone that support the teeth, which cannot be fully evaluated through visual inspection alone. Specialized evaluation methods help identify disease activity beneath the gumline where damage often begins. This deeper assessment allows subtle changes to be detected before they lead to advanced bone loss or tooth instability.
Comprehensive periodontal evaluation provides the foundation for accurate diagnosis and long-term treatment planning. By combining clinical measurements, imaging, and risk assessment, Los Angeles periodontists gain a clearer picture of disease behavior over time. This approach helps differentiate stable conditions from active disease that requires intervention. Evaluating periodontal health beyond routine exams ensures treatment decisions are based on structural realities rather than surface-level findings.
Periodontal evaluation includes precise measurement of gum pocket depths around each tooth. These measurements reveal whether the gums have detached from the teeth, creating spaces where bacteria can accumulate. Increased pocket depth often signals active disease that requires targeted care. Tracking attachment levels over time helps determine whether conditions are stable or progressing. This information guides decisions about monitoring versus intervention.
Why Pocket Measurements Reveal Hidden Disease Activity
Deeper pockets indicate areas where bacteria thrive beyond the reach of routine hygiene. These environments allow inflammation to persist and damage supporting tissues. Measuring pocket depth provides objective data about disease severity and progression.
How Attachment Levels Influence Treatment Decisions
Attachment loss reflects structural changes that cannot be reversed without intervention. Identifying these changes early helps determine appropriate treatment timing. Accurate measurements support individualized care planning.
Bone health plays a critical role in tooth stability and overall oral function. Diagnostic imaging allows evaluation of bone levels surrounding each tooth and across the jaw. Subtle bone loss may not produce symptoms but can indicate advancing periodontal disease. Imaging helps identify patterns of deterioration that influence treatment strategy. This assessment ensures care decisions reflect both current condition and future risk.
How Imaging Provides Insight Beyond Visual Exams
Radiographic images reveal bone changes hidden beneath gum tissue. These images help distinguish between localized and generalized bone loss. Imaging allows clinicians to assess structural integrity accurately.
Why Bone Assessment Supports Long-Term Oral Stability
Bone loss directly affects tooth retention and bite function. Early identification allows steps to be taken to preserve remaining support. Ongoing monitoring helps prevent further deterioration.
Periodontal evaluation considers individual risk factors that influence disease development and progression. Factors such as medical history, genetics, oral hygiene habits, and previous treatment outcomes all play a role. Understanding these variables helps predict how periodontal disease may behave over time. Evaluation focuses on patterns rather than isolated findings. This broader perspective supports proactive management rather than reactive treatment.
How Risk Factors Shape Periodontal Assessment
Certain conditions increase susceptibility to tissue breakdown and bone loss. Evaluating these factors helps explain why disease progresses differently among patients. Risk assessment informs both monitoring frequency and treatment approach.
Why Progression Patterns Matter for Treatment Planning
Disease progression is rarely uniform across the mouth. Identifying active versus stable areas helps prioritize care. Understanding patterns supports more precise and effective intervention.
Active periodontal infection must be addressed before long-term stability can be achieved. Bacterial activity beneath the gumline drives inflammation that weakens tissue attachment and bone support. Treatment planning prioritizes infection control to prevent continued breakdown of supporting structures. This phase often determines how much natural tissue can be preserved. Early control improves the effectiveness of later treatment stages.
Why Infection Control Comes Before Structural Repair
Inflammation interferes with healing and tissue response. Attempting repair while infection remains active reduces treatment success. Stabilizing bacterial levels creates conditions necessary for recovery.
How Early Disease Control Improves Long-Term Outcomes
Reducing infection lowers inflammatory pressure on the gums and bone. This allows tissues to respond more predictably to care. Long-term stability depends on this initial control phase.
Periodontal tissues respond differently depending on disease severity and individual risk factors. Treatment plans must be adjusted as healing progresses or stabilizes. Monitoring tissue response allows clinicians to refine care rather than repeating ineffective approaches. Bone and gum changes guide whether additional intervention is needed. This adaptive strategy supports sustained improvement rather than short-term results.
How Tissue Response Guides Ongoing Care Decisions
Healing patterns reveal whether disease activity has slowed or persists. A positive response may allow less aggressive care. Poor response signals the need for modification.
Why Ongoing Assessment Prevents Treatment Stagnation
Static plans can fail when conditions change. Reassessment ensures care evolves with tissue response. This flexibility supports durable outcomes.
Long-term periodontal stability depends on consistent maintenance after active treatment. Maintenance planning focuses on preventing reinfection and monitoring subtle changes over time. Without structured follow-up, previously treated disease can reemerge. Treatment plans therefore extend beyond procedures into ongoing care schedules. Maintenance reinforces the stability achieved through earlier intervention.
How Maintenance Protects Prior Treatment Results
Regular monitoring helps detect early signs of recurrence. Professional care disrupts bacterial buildup before damage resumes. Maintenance preserves treatment gains.
Why Long-Term Planning Reduces Disease Recurrence
Periodontal disease has a chronic component for many patients. Ongoing care reduces the likelihood of relapse. Structured maintenance supports lasting oral stability.

How Los Angeles Periodontists Carry Out Treatment in Complex Cases
Complex periodontal cases require a methodical treatment approach that addresses both active disease and structural changes that have already occurred. These cases often involve deeper periodontal pockets, bone loss, or recurring infection that cannot be resolved through basic interventions alone. Treatment is typically delivered in stages, allowing clinicians to control infection, evaluate tissue response, and adjust care as conditions evolve. Each phase builds on the previous one to avoid unnecessary intervention while protecting remaining support structures.
Carrying out periodontal treatment in complex situations also involves careful coordination between evaluation findings and clinical execution. Decisions are guided by how the gums and bone respond rather than rigid timelines. This adaptive approach reduces the risk of overtreatment while ensuring disease activity is properly managed. Precision and flexibility are central to achieving long-term stability in advanced periodontal cases.
Initial Disease Control and Stabilization Phase
The first stage of complex periodontal treatment focuses on reducing active infection and controlling inflammation throughout the affected areas. Bacterial activity beneath the gumline drives tissue breakdown and must be addressed before meaningful healing can occur. This phase aims to interrupt disease progression and establish a healthier environment within the gums. Tissue response during this stage provides valuable insight into disease severity and treatment resistance. Stabilization outcomes strongly influence how subsequent care is planned.
Monitoring Tissue Response and Adjusting Care
Following initial stabilization, periodontal tissues are monitored closely for signs of improvement or continued breakdown. Changes in inflammation, pocket depth, and tissue attachment guide treatment refinement. This phase allows clinicians to adapt care based on biological response rather than assumptions. Monitoring helps identify areas that respond well and those that remain resistant. Ongoing evaluation prevents ineffective repetition and unnecessary escalation.
Coordinating Advanced Procedures With Our Los Angeles Periodontists When Necessary
Some complex cases require advanced procedures to address remaining disease or structural damage. These interventions are considered only after infection control and tissue response have been evaluated thoroughly. Careful coordination ensures procedures are limited to clearly defined problem areas. This stepwise approach reduces unnecessary risk and supports healing predictability. Advanced care is integrated thoughtfully rather than applied broadly.
How Periodontal Care Supports Bone and Gum Regeneration
Bone and gum regeneration plays a critical role in restoring stability after periodontal disease has caused structural damage. Regenerative periodontal care focuses on encouraging the body’s natural healing processes while controlling infection and inflammation. These approaches are designed to rebuild lost support rather than simply slow further deterioration. Treatment decisions depend on the extent of bone loss, tissue condition, and overall healing potential. Care planning emphasizes predictability, preservation, and long-term oral stability.
Los Angeles periodontists use regenerative strategies to help restore both hard and soft tissues affected by periodontal disease. These methods are integrated carefully into broader treatment plans rather than applied in isolation. Regeneration is most effective when underlying disease activity has been controlled and tissues are biologically prepared to heal. The goal is to reestablish support structures that contribute to tooth retention, comfort, and function.
Bone regeneration focuses on rebuilding support that has been lost due to chronic inflammation and prolonged bacterial infection. Periodontal disease disrupts the balance between bone breakdown and new bone formation, allowing loss to progress over time. Regenerative care aims to restore this balance by creating conditions that favor healing rather than continued destruction. Treatment decisions are guided by defect shape, depth, and surrounding tissue stability. Successful bone regeneration improves tooth stability and helps reduce the risk of future tooth loss.
How Controlled Healing Environments Promote Predictable Bone Formation
Bone regeneration depends on creating a stable environment where healing can occur without disruption. Reducing bacterial contamination and controlling inflammation allows bone-forming cells to function more effectively. Stabilization of the treatment site supports predictable tissue response and structural rebuilding.
Why Bone Regeneration Requires Detailed Planning and Sequencing
Bone regeneration cannot succeed without proper timing and preparation. Inadequate sequencing may interfere with healing and limit structural recovery. Careful planning maximizes the likelihood of durable, long-term bone support.
Healthy gum tissue is essential for protecting regenerated bone and preventing reinfection. Periodontal regeneration also focuses on improving soft tissue attachment and increasing tissue thickness. Stronger gum tissue creates a more effective barrier against bacterial penetration and irritation. Treatment selection considers tissue quality, anatomy, and functional demands. Improved attachment contributes to comfort, stability, and long-term periodontal health.
How Soft Tissue Healing Supports Structural and Biological Stability
Gum tissue serves as the first line of defense against bacterial invasion. Improved attachment reduces pocket depth and limits inflammation. Healthy tissue enhances the success and durability of regenerative care.
Why Tissue Thickness Influences Long-Term Periodontal Outcomes
Thin or compromised tissue is more susceptible to recession and breakdown. Increasing tissue thickness improves resistance to mechanical and bacterial stress. Stronger tissue supports lasting treatment results.
Regeneration is most effective when incorporated into a comprehensive periodontal care strategy. Long-term success depends on continued disease control, maintenance, and monitoring after regeneration. Regenerative improvements must be protected through consistent professional care and patient participation. Treatment planning emphasizes prevention of recurrence alongside structural restoration. Integration ensures that regenerative gains remain stable over time.
How Maintenance Care Protects Regenerated Bone and Tissue
Regular monitoring allows early identification of changes that threaten healing structures. Maintenance care disrupts bacterial accumulation before damage resumes. Ongoing care preserves regenerative results.
Why Continued Periodontal Oversight Is Essential After Regeneration
Regeneration does not eliminate the underlying susceptibility to periodontal disease. Continued oversight helps protect restored structures from relapse. Long-term professional involvement supports durability and stability.
The Role of Periodontal Maintenance After Regenerative Treatment
Successful regenerative periodontal treatment does not conclude once bone and gum tissue have healed, because long-term stability depends on continued monitoring, bacterial control, and reinforcement of healthy tissue attachment over time. After regeneration, the supporting structures of the teeth remain biologically susceptible to reinfection if inflammation and bacterial accumulation are not carefully managed through professional care. Periodontal maintenance focuses on preserving regenerative improvements by tracking tissue response, reinforcing home care practices, and identifying subtle changes that may signal early relapse. This phase of care is critical for transforming regenerative success into lasting oral stability rather than a temporary improvement. Los Angeles periodontists consistently emphasize that maintenance is an essential extension of regenerative treatment.
Ongoing periodontal maintenance is structured to reduce the likelihood of disease recurrence while supporting the long-term integrity of regenerated bone and gum tissue. Los Angeles periodontists design maintenance schedules based on individual healing patterns, medical risk factors, and the severity of prior periodontal breakdown to ensure care remains appropriately proactive. These visits allow clinicians to identify minor inflammatory changes before they escalate into active disease that threatens regenerated structures. Long-term periodontal success depends on consistent professional oversight combined with patient participation between visits. Maintenance care ensures that regenerative outcomes remain stable as oral conditions evolve over time.
Post-treatment monitoring focuses on evaluating whether regenerated bone and gum tissue maintain stability under daily functional forces such as chewing, brushing, and natural oral movement. Even small changes in pocket depth, tissue firmness, or inflammatory response can indicate early instability if not addressed promptly. Regular periodontal assessments allow clinicians to confirm that healing continues as expected following regenerative care. Monitoring also helps identify localized areas that may require additional attention or adjustments to maintenance routines. Los Angeles periodontists rely on consistent monitoring to protect the long-term success of regenerative treatment outcomes.
How Ongoing Evaluation Identifies Subtle Signs of Periodontal Relapse
Early relapse often begins with minor inflammatory changes that may not produce noticeable symptoms for patients. Professional evaluation detects these changes through detailed measurements, tissue assessment, and comparison to baseline healing data. Identifying instability at this stage allows corrective action before structural damage resumes.
Why Early Intervention Is Critical for Preserving Regenerated Structures
Addressing minor changes promptly helps prevent progression into active periodontal disease. Early intervention protects newly regenerated bone and soft tissue from renewed bacterial damage. Timely care plays a key role in maintaining long-term stability.
Even after successful regeneration, bacterial exposure remains a constant challenge due to the complex anatomy of previously diseased areas. Daily oral hygiene alone may not consistently disrupt bacterial accumulation around regenerated tissue margins. Periodontal maintenance visits provide targeted professional cleaning that supports effective bacterial control. This ongoing care reduces inflammatory pressure on healing tissues and supports long-term attachment stability. Los Angeles periodontists prioritize bacterial management as a foundational component of post-regenerative care.
How Professional Maintenance Reduces the Risk of Inflammatory Breakdown
Professional periodontal maintenance reaches areas that routine brushing and flossing cannot adequately address. Removal of bacterial deposits reduces inflammatory triggers that compromise tissue health. This support helps maintain a stable biological environment around regenerated structures.
Why Bacterial Control Directly Impacts Regenerative Longevity
Unchecked bacterial activity can gradually undermine regenerated bone and tissue. Consistent bacterial control limits destructive processes that threaten healing outcomes. Long-term regenerative success depends on maintaining this balance.
Not all patients share the same risk level following periodontal regeneration, which makes individualized maintenance planning essential. Factors such as systemic health conditions, genetic predisposition, and previous disease severity influence how tissues respond over time. Maintenance strategies are adjusted to reflect these variables rather than relying on standardized schedules. Care intensity may change as healing stabilizes or new risk factors emerge. Los Angeles periodontists tailor long-term maintenance strategies to protect each patient’s regenerative results.
How Risk Assessment Shapes Long-Term Maintenance Planning
Patients with elevated risk require closer monitoring and more frequent professional care. Lower-risk individuals may maintain stability with less intensive schedules. Risk-based planning improves both efficiency and outcomes.
Why Personalized Maintenance Supports Lasting Periodontal Health
Uniform maintenance approaches may fail to address individual vulnerabilities. Personalized strategies focus care where it is most needed. This customization strengthens long-term treatment durability.
Why Patients Choose PhD Dental's Los Angeles Periodontists
Choosing a provider for periodontal care often involves more than addressing immediate symptoms, especially when long-term gum and bone health are at stake. Patients seek a practice that combines clinical precision, clear communication, and a treatment philosophy focused on stability rather than short-term fixes. PhD Dental approaches periodontal care with an emphasis on education, coordination, and thoughtful planning that supports lasting outcomes. This approach helps patients feel informed and supported throughout every phase of care. Trust is built through consistency, transparency, and a commitment to long-term oral health.
Patients also value a care environment where periodontal treatment is integrated into a broader dental framework rather than handled in isolation. PhD Dental emphasizes collaboration between providers to ensure periodontal care aligns with overall oral health goals. This coordinated approach reduces fragmentation and improves continuity. Care decisions are guided by both clinical findings and patient priorities. Los Angeles periodontists working within PhD Dental contribute specialized expertise while remaining connected to the patient’s broader care plan.
PhD Dental treats a wide range of periodontal conditions, including cases involving advanced bone loss, tissue damage, and recurring disease. Experience with complex presentations allows providers to anticipate challenges that may not be apparent during early evaluation. This familiarity supports more accurate planning and realistic expectations for outcomes. Patients benefit from care that reflects both technical knowledge and clinical judgment developed over time. Los Angeles periodontists at PhD Dental bring specialized training to cases that require a higher level of precision and oversight.
How Experience Shapes Treatment Strategy and Decision-Making
Experience influences how disease patterns are interpreted and addressed. Subtle indicators of progression or instability are recognized earlier through repeated exposure to complex cases. This insight helps guide decisions that balance intervention with preservation.
Why Depth of Experience Matters in Advanced Periodontal Care
Advanced cases often require nuanced sequencing rather than standardized approaches. Experience supports better timing and selection of care strategies. This depth reduces uncertainty and improves predictability.
Periodontal care is most effective when it is coordinated with other aspects of oral health management. PhD Dental integrates periodontal treatment into a broader network of dental services to support continuity. This coordination helps ensure that periodontal decisions align with restorative planning and long-term maintenance goals. Patients experience fewer disruptions and clearer transitions between phases of care. A unified care model supports consistency across visits and providers.
How Integrated Care Improves Treatment Continuity
Shared records and communication allow providers to stay aligned on treatment goals. This alignment reduces repetition and conflicting recommendations. Continuity strengthens patient confidence and comfort.
Why Coordination Supports Long-Term Periodontal Stability
Fragmented care can undermine treatment outcomes over time. Coordinated planning reinforces stability across multiple stages of care. Long-term success benefits from this consistency.
PhD Dental places strong emphasis on helping patients understand their periodontal condition and treatment options. Education supports informed decision-making rather than passive compliance. Patients are encouraged to ask questions and participate actively in care planning. Clear explanations reduce anxiety and increase confidence in recommended treatment paths. Los Angeles periodontists within the practice prioritize communication as a core component of effective care.
How Patient Education Improves Treatment Participation
Understanding the reasoning behind care recommendations increases engagement. Educated patients are more likely to follow maintenance guidance. Participation strengthens outcomes.
Why Clear Communication Builds Long-Term Trust
Transparency fosters confidence in both providers and treatment plans. Trust grows when patients feel respected and informed. Long-term relationships depend on this clarity.
Schedule an Appointment With PhD Dental's Los Angeles Periodontists Today

Periodontal concerns often require timely attention and a clear plan that prioritizes long-term gum and bone stability rather than temporary relief. Working with experienced Los Angeles periodontists allows underlying issues to be addressed thoughtfully, with care strategies designed to protect natural teeth and support lasting oral health. At PhD Dental, periodontal care is delivered within a coordinated dental environment where communication, precision, and patient understanding remain central to every decision.
If you have been referred for periodontal treatment or are concerned about changes in your gum health, the team at PhD Dental is ready to help you move forward with clarity and confidence. Call (323) 269-5437 to speak with our Los Angeles periodontists or visit our contact page to schedule your consultation and learn how comprehensive periodontal care can support your long-term oral stability.
Learn About Our Periodontics Services
Call Us 24/7
Learn about our periodontics services at PhD Dental, including treatment for gum disease, gum recession, and dental implant support. Our team focuses on protecting your gum health and preserving the strong foundation your smile needs.
LEARN MOREGet in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 9:30AM - 6:30PM
- Tue 9:30AM - 6:30PM
- Wed 9:30AM - 6:30PM
- Thu 9:30AM - 6:30PM
- Fri 9:30AM - 6:30PM
- Sat 9:00AM - 4:00PM
- Sun Closed