
Endosteal Implants in Inglewood
Replacing missing teeth with implant based solutions requires careful consideration of bone support and long-term functional expectations. Endosteal implants in Inglewood are placed directly into the jawbone and are commonly used when patients have sufficient bone volume to support a stable foundation for individual crowns, bridges, or fixed restorations. This approach emphasizes structural integration with the jaw which makes planning and placement especially important for long-term performance.
Choosing endosteal implants in Inglewood also involves understanding how bone quality, healing capacity, and bite forces influence implant success over time. Dentists rely on detailed imaging and evaluation to determine if the jawbone can support direct implant placement without compromising surrounding structures. Treatment decisions prioritize durability and comfort rather than speed or convenience alone. This measured approach helps ensure implants function reliably as part of the patient’s natural bite. If you are considering endosteal implants in Inglewood, call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation focused on healing and long-term outcomes.
Table of Contents
- Who Is a Candidate for Endosteal Implants in Inglewood
- How Healing Phases Differ After Endosteal Implant Placement
- How Dentists Plan Implant Placement for Endosteal Implants in Inglewood
- How PhD Dental Coordinates Surgical and Restorative Decisions for Endosteal Implants
- Call PhD Dental About Endosteal Implants in Inglewood Today
Who Is a Candidate for Endosteal Implants in Inglewood
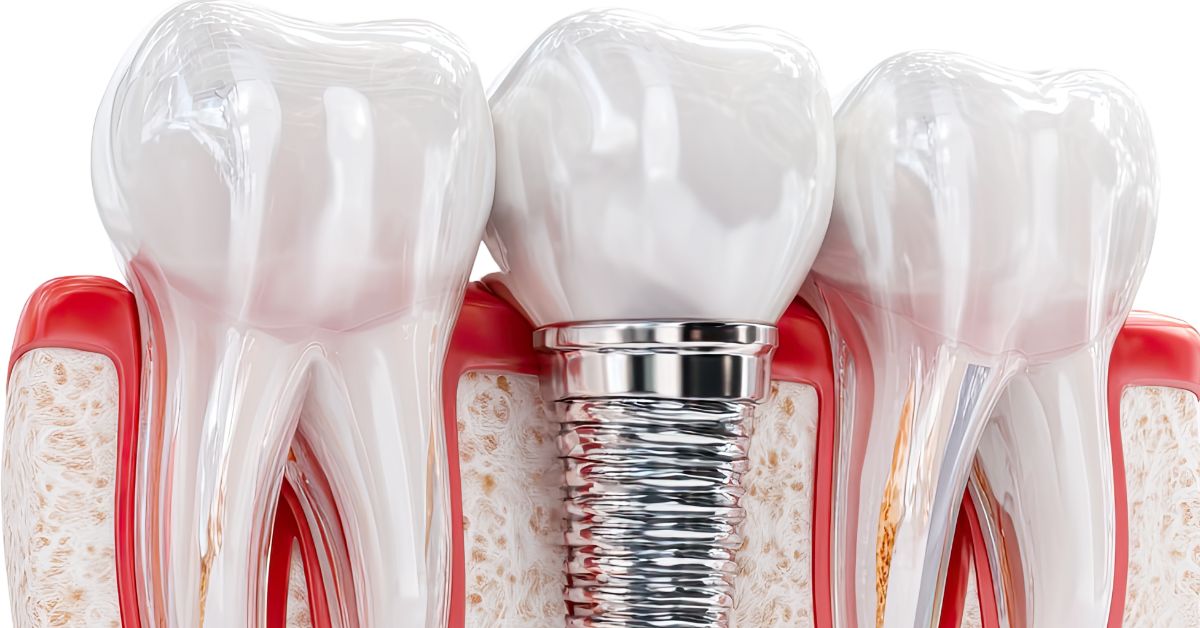
Determining candidacy for implant placement requires evaluating more than whether a tooth is missing or damaged. Dentists assess anatomical readiness, systemic health, and long-term functional demands before recommending endosteal implants in Inglewood as a viable solution. This process ensures that implants integrate predictably with the jawbone and remain stable under daily chewing forces. Patient selection focuses on biological compatibility rather than convenience or treatment speed. Careful screening protects patients from pursuing implant care that their anatomy may not reliably support.
Candidacy discussions also clarify when preparatory treatment may be necessary before implant placement can proceed. Some patients require bone management, infection control, or medical coordination to create appropriate conditions for surgery. Identifying these needs early prevents compromised outcomes later in treatment. This structured evaluation allows dentists to recommend endosteal implants in Inglewood only when long-term success remains realistic. At PHD Dental our patients know that responsible planning remains central to implant longevity.
Sufficient jawbone volume and density are essential for anchoring implants placed directly within bone. Dentists evaluate whether the jaw can provide primary stability during placement and sustained support during healing. Bone quality influences implant diameter, length, and positioning decisions. Inadequate bone may limit placement options or require preparatory procedures. These assessments determine whether endosteal implants in Inglewood can be placed safely and predictably.
How Dentists Measure Bone Readiness
Dentists rely on three-dimensional imaging to evaluate bone height, width, and density across potential implant sites. This imaging allows precise identification of resorbed areas, cortical thickness, and anatomical boundaries that influence implant placement strategy. Measurements guide decisions about implant length, angulation, and the need for preparatory procedures. Accurate imaging reduces surgical uncertainty and supports controlled placement.
Why Bone Sufficiency Supports Long-Term Stability
Adequate bone volume allows implants to achieve secure primary fixation at placement. Stable fixation supports controlled force transfer during healing and long-term function. Insufficient bone increases the risk of mechanical overload and compromised integration over time.
Systemic health plays a critical role in how well implants integrate and surrounding tissues respond to surgery. Dentists review medical history, medications, and conditions that may affect healing. Factors such as uncontrolled diabetes or compromised immunity require careful management. Healing capacity influences both surgical timing and complication risk. This review protects patients considering endosteal implants in Inglewood from preventable setbacks.
How Medical Screening Guides Treatment Decisions
Medical screening allows dentists to identify conditions that may slow healing or increase surgical risk. Dentists may coordinate with physicians to stabilize health factors before proceeding. Treatment timing can be adjusted to support predictable recovery. These decisions prioritize biological readiness over scheduling convenience.
Why Health Disclosure Matters for Implant Success
Accurate medical disclosure allows dentists to anticipate healing challenges and plan appropriately. Undisclosed conditions can compromise integration and increase complication risk. Transparency supports responsible decision making and safer outcomes.
Implants must withstand daily chewing forces without excessive stress on surrounding bone. Dentists evaluate bite patterns, jaw movement, and habits such as grinding or clenching. Excessive forces can overload implants if not addressed during planning. Functional analysis informs implant positioning and restoration design. These considerations influence candidacy for endosteal implants in Inglewood.
How Bite Analysis Influences Implant Planning
Dentists assess occlusal contact patterns and jaw movement to understand how forces distribute during function. Implant placement and restorative design adjust to balance these forces across the jaw. Proper force distribution protects implant interfaces and surrounding bone. Functional analysis supports long-term mechanical stability.
Why Habit Evaluation Occurs Early
Unmanaged clenching or grinding can place excessive stress on implants. Early identification allows dentists to incorporate protective strategies into treatment planning. Addressing habits before placement reduces long-term mechanical risk.
How Healing Phases Differ After Endosteal Implant Placement

Healing following implant surgery occurs through a sequence of biological phases that directly influence whether the implant becomes a stable, long-term replacement or encounters integration challenges. Dentists emphasize that healing is an active biological process rather than a passive waiting period, with each stage requiring specific protections and clinical oversight. Endosteal implants in Inglewood depend on controlled bone response, soft tissue adaptation, and carefully managed functional forces during this time. Each phase introduces different risks and responsibilities that affect patient behavior, hygiene routines, and follow-up scheduling. Understanding how healing progresses allows patients to protect outcomes instead of unintentionally compromising them.
The timing of restorative steps is determined by how the body responds biologically rather than by an arbitrary calendar. Dentists monitor measurable indicators of bone and tissue adaptation before allowing treatment to advance. This approach prevents premature loading that can undermine integration before it is fully established. Healing capacity varies from patient to patient based on anatomy and health factors. Respecting these differences supports predictable long-term stability.
The earliest healing phase begins immediately after surgical placement and involves the body stabilizing the implant site at a cellular level. Blood clot formation and inflammatory response initiate the groundwork for new bone development around the implant surface. During this period, the implant remains particularly vulnerable to movement and excessive pressure. Even small disruptions can interfere with early attachment processes. Protecting the site during this phase directly influences long-term integration quality.
How Dentists Protect Stability During Initial Healing
Dentists provide detailed guidance on limiting chewing forces and avoiding mechanical stress near the implant site. Temporary adjustments may be made to the bite to reduce pressure during everyday function. Follow-up evaluations assess swelling, discomfort, and early tissue response. These steps collectively preserve the conditions needed for stable integration.
Why Early Movement Affects Integration Quality
Micromovement during the earliest healing phase can interrupt the formation of a stable bone interface. Disruption at this stage weakens the structural connection that develops later. Preventing unnecessary movement supports stronger and more uniform bone attachment.
Soft tissue healing occurs simultaneously with bone integration and plays a critical role in long-term implant health. Gum tissue adapts around the implant to create a protective seal against bacterial intrusion. Inadequate adaptation can expose underlying bone to inflammation. Dentists monitor tissue contour, color, and attachment carefully. Healthy tissue supports both comfort and hygiene effectiveness.
How Soft Tissue Health Affects Implant Longevity
Stable gum tissue helps protect the implant interface from chronic irritation. Well-adapted tissue supports easier cleaning and reduces plaque accumulation. Tissue health influences both function and appearance. Long-term success depends on this protective barrier.
Why Tissue Management Continues Beyond Initial Closure
Healing does not stop once sutures are removed or discomfort subsides. Tissue continues to remodel as function resumes. Ongoing evaluation identifies early signs of inflammation. Continued management preserves stability.
The final healing phase involves gradually introducing functional forces to the integrated implant. Dentists confirm that biological milestones have been met before allowing the implant to support a crown or other restoration. Load is introduced carefully to encourage bone adaptation rather than stress overload. This transition marks a shift from healing to functional use. Timing remains individualized for safety.
How Dentists Determine Readiness for Restoration
Clinical readiness is assessed through stability measurements, imaging findings, and soft tissue evaluation. Dentists confirm that integration can withstand functional forces. Comfort and absence of inflammation are considered together. These criteria guide restoration timing.
Why Gradual Loading Matters Biologically
Bone responds best to progressive force adaptation rather than sudden stress. Gradual loading encourages strengthening around the implant. Controlled progression protects integration and long-term performance.
How Dentists Plan Implant Placement for Endosteal Implants in Inglewood
Planning implant placement involves converting diagnostic findings into precise surgical decisions that account for anatomy, restoration design, and long-term mechanical behavior. Dentists approach endosteal implants in Inglewood by determining where implants can be placed to achieve stability while supporting proper bite alignment and hygiene access. Placement planning balances available bone with restorative requirements so implants function predictably once loaded. Each decision considers how forces will transfer through the implant into surrounding bone during daily use. Careful planning at this stage reduces the likelihood of complications that cannot be corrected after placement.
Dentists also recognize that no two jaws present identical anatomical conditions, even when tooth loss appears similar on the surface. Variations in bone contour, density, and anatomical landmarks require individualized placement strategies. Digital imaging and restorative modeling allow these differences to be addressed before surgery begins. Planning adapts to patient anatomy rather than forcing standardized spacing or angulation. This individualized approach supports predictable outcomes for endosteal implants in Inglewood.
Dentists begin placement planning by identifying regions of the jaw that can support direct implant anchorage without compromising surrounding structures. Bone height, width, and density are evaluated in relation to nerves, sinuses, and adjacent tooth roots. These anatomical constraints define where implants can be placed safely and how deep they can extend. Placement decisions respect these boundaries to avoid sensory complications or restorative limitations. Anatomical evaluation establishes the physical framework within which planning occurs.
How Imaging Defines Safe Placement Zones
Three-dimensional imaging provides detailed visualization of internal bone architecture and critical anatomical landmarks. Dentists use this information to map implant trajectories before surgery. Imaging clarifies spatial relationships that are not visible during clinical examination. This preparation reduces intraoperative uncertainty and supports controlled placement.
Why Respecting Anatomical Boundaries Protects Future Function
Implants placed too close to nerves or sinuses can cause chronic discomfort or restrict restorative design. Boundary violations may also limit implant longevity by compromising surrounding structures. Respecting anatomical limits preserves both safety and functional flexibility. Long-term success depends on these considerations.
Implant placement is planned with the final restoration in mind rather than bone availability alone. Dentists consider crown position, emergence profile, and contact relationships during placement planning. This alignment ensures that restorations sit naturally within the bite and are accessible for cleaning. Poor alignment can lead to uneven forces or hygiene challenges. Restorative driven planning reduces compromise later in treatment.
How Restorative Goals Shape Surgical Decisions
Digital restorative models allow dentists to visualize final crown or bridge placement before surgery. Implant positions are adjusted to support these designs accurately. This coordination prevents awkward angulation or excessive cantilevering. Surgical decisions reflect restorative intent rather than convenience.
Why Planning From the Restoration Backward Matters
Working backward from the final restoration avoids corrective procedures after placement. Proper alignment supports comfort, function, and appearance. This approach prioritizes durability over speed. Long-term outcomes improve when restoration needs guide placement.
Spacing between implants and adjacent teeth influences how chewing forces are transmitted through bone and restorative materials. Dentists evaluate spacing carefully to prevent stress concentration at implant interfaces. Improper spacing can accelerate bone remodeling or mechanical wear over time. Balanced distribution of force protects both implants and surrounding structures. Spacing decisions are integral to long-term performance.
How Dentists Anticipate Functional Forces During Planning
Dentists analyze bite records, jaw movement, and contact patterns to understand how force is applied during function. These findings inform where implants should be positioned to accommodate vertical and lateral forces. Placement strategies are adjusted to reduce excessive loading during everyday movements. Anticipating forces before surgery reduces the need for later correction. Functional analysis transforms placement into a dynamic decision.
Why Load Distribution Influences Implant Longevity
Even force distribution reduces the risk of localized overload at the bone implant interface. Concentrated stress can weaken integration or contribute to mechanical complications. Balanced loading supports sustained stability under repeated use. Longevity depends on managing these forces from the outset.
How PhD Dental Coordinates Surgical and Restorative Decisions for Endosteal Implants
Successful implant treatment depends on how well surgical execution and restorative planning are aligned long before any procedure begins. PhD Dental approaches endosteal implants in Inglewood by treating surgery and restoration as interdependent phases rather than isolated steps handled independently. Decisions about implant position, depth, and angulation are made in direct relation to how the final crown or bridge must function within the bite. This coordination reduces the risk of compromises that only become apparent after implants are already placed. Integrated planning supports outcomes that remain stable, functional, and serviceable over time.
Coordination also allows the dental team to anticipate future restorative needs rather than reacting to limitations created during surgery. PhD Dental evaluates how materials will wear, how hygiene access will be maintained, and how forces will be distributed across restorations before placement occurs. This foresight shapes both surgical technique and restorative design. Patients benefit from a treatment plan that accounts for years of function rather than only the day of surgery. Alignment between phases remains central to predictable implant performance.
Surgical planning at PhD Dental begins with a clear understanding of what the final restoration must accomplish functionally and structurally. Dentists evaluate where crowns or bridges need to emerge within the arch to support proper bite alignment and speech. Implant placement is adjusted to ensure restorations can be positioned naturally without excessive angulation or cantilevering. This approach prevents surgical decisions from limiting restorative options later. Surgery is shaped by restorative intent rather than convenience.
How Restorative Modeling Informs Surgical Placement
Digital restorative models allow dentists to visualize final crown contours before surgery. These models guide implant positioning to support proper emergence profiles and contact points. Surgical guides may be created to transfer this plan accurately to the clinical setting. Modeling ensures placement decisions align with restorative goals.
Why Restoration Driven Surgery Reduces Future Complications
When implants are placed without restorative guidance, adjustments often become necessary later. Poor alignment can lead to uneven forces or hygiene challenges. Restoration driven surgery minimizes these risks. Long-term function benefits from this coordination.
PhD Dental carefully coordinates when restorative steps occur relative to surgical healing milestones. Dentists avoid advancing treatment before bone and tissue conditions support functional loading. Healing timelines are individualized based on biological response rather than predetermined schedules. This coordination protects integration while maintaining progress. Timing decisions balance patience with efficiency.
How Dentists Determine Appropriate Restoration Timing
Stability testing, imaging, and tissue evaluation inform readiness for restoration. Dentists assess whether implants can withstand functional forces. Comfort and absence of inflammation are considered together. These factors guide safe progression.
Why Premature Restoration Can Compromise Outcomes
Loading implants too early can overload developing bone attachment. Premature force may weaken integration. Coordinated timing protects structural stability. Long-term success depends on respecting healing phases.
Clear communication between surgical and restorative planning remains continuous throughout treatment. PhD Dental documents placement details that influence restorative design. Adjustments are discussed collaboratively rather than independently. This communication prevents misalignment between phases. Continuity supports consistency.
How Documentation Supports Coordinated Care
Detailed records of implant position, depth, and orientation inform restorative fabrication. Dentists reference these records during restoration planning. Accurate documentation reduces guesswork. Coordination improves efficiency and accuracy.
Why Integrated Oversight Supports Long-Term Care
Ongoing collaboration allows future maintenance and adjustments to proceed smoothly. Understanding original planning decisions informs long-term monitoring. Integrated oversight protects implant and restoration performance. Continuity benefits patients over time.
Call PhD Dental About Endosteal Implants in Inglewood Today
Choosing an implant solution involves more than selecting a procedure, especially when long-term comfort, function, and maintenance are part of the decision. Patients exploring endosteal implants in Inglewood benefit from understanding how surgical placement and ongoing care must work together to support stable outcomes over time. PhD Dental approaches these conversations with transparency so patients understand not only what treatment involves, but also why specific planning decisions matter.
A consultation provides the opportunity to review bone readiness, bite considerations, healing expectations, and restoration planning in a coordinated discussion. Dentists explain how endosteal implants in Inglewood are planned to integrate with existing oral structures while supporting long-term function. Patients leave with a realistic understanding of timelines, responsibilities, and expected outcomes rather than generalized promises. Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation and discuss if endosteal implants in Inglewood align with your oral health needs, goals, and long-term expectations.
Get in Touch with PhD Dental
PhD Dental Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
