
Mini Dental Implants in Inglewood
Replacing missing teeth does not always require the same implant size or surgical approach, particularly when bone volume or anatomical limitations influence treatment planning. Mini dental implants in Inglewood are designed for specific situations where traditional implant dimensions may not be appropriate, allowing dentists to stabilize restorations with a more conservative surgical footprint. Choosing mini dental implants in Inglewood involves understanding how implant diameter, bone engagement, and restorative purpose interact during both placement and long-term use.
Dentists evaluate if these mini implants can support the intended restoration without introducing excess stress to bone or surrounding structures. Treatment planning emphasizes realistic expectations, healing behavior, and maintenance considerations. This careful assessment helps ensure mini implants are used appropriately and responsibly. If you are considering mini dental implants in Inglewood and want to understand whether this option aligns with your bone structure, restoration goals, and long-term oral health, call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation today.
Top-Rated Dentists
in Los Angeles
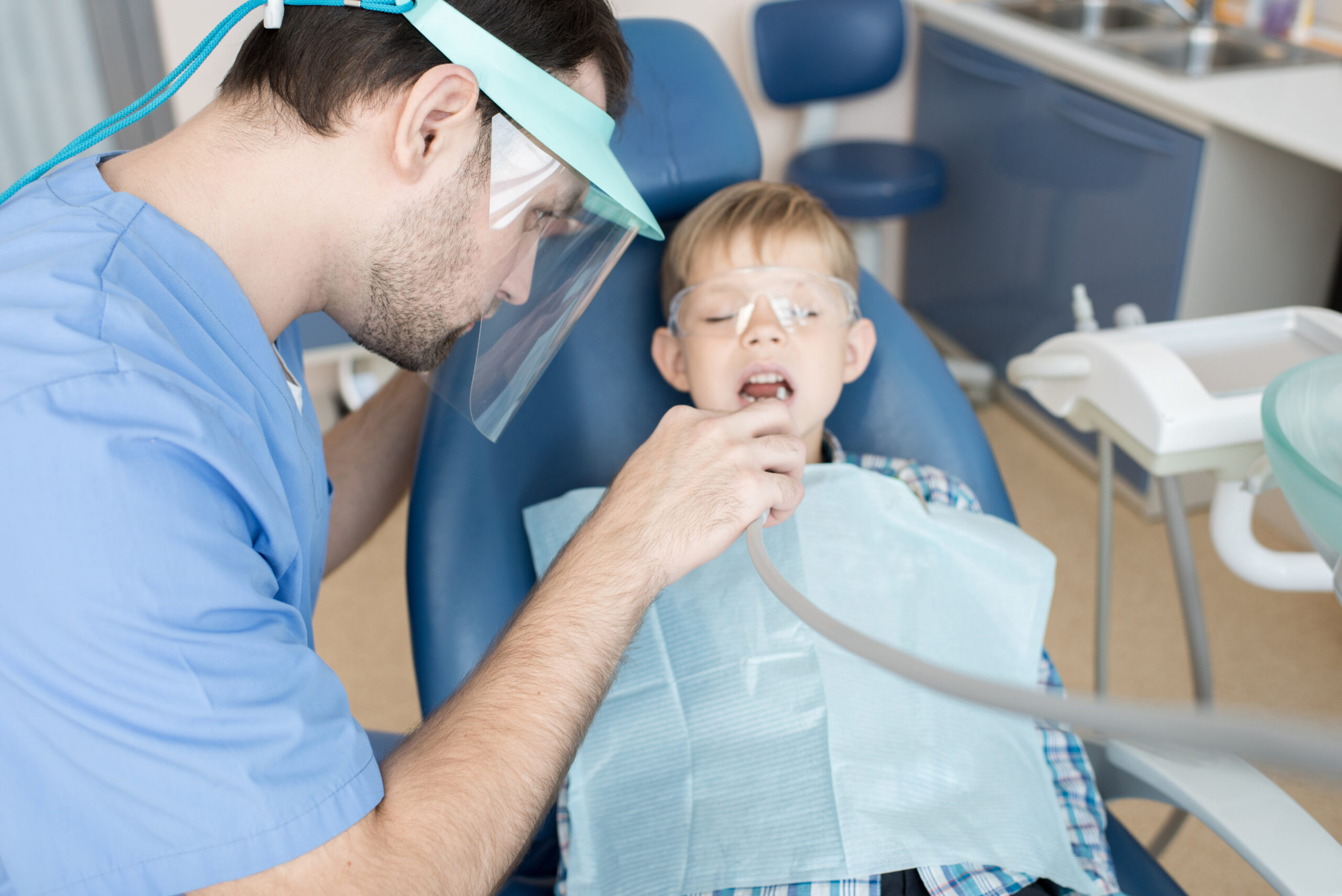
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
- How Mini Dental Implants in Inglewood Are Structurally Different From Standard Implants
- What the Mini Dental Implant Placement Process Involves
- Why Dentists Recommend Mini Dental Implants in Specific Treatment Situations
- How PhD Dental Coordinates Mini Implant Planning With Long-Term Oral Health
- Talk With PhD Dental About Mini Dental Implants in Inglewood Today
How Mini Dental Implants in Inglewood Are Structurally Different From Standard Implants
Mini implants differ from traditional implant systems in ways that directly affect how they interact with bone, tolerate functional forces, and support restorative components. Dentists evaluate mini dental implants in Inglewood as a distinct structural category rather than a reduced version of conventional implants. Differences in diameter, surface area, and load behavior influence which clinical situations are appropriate for their use. These distinctions shape placement strategy, restoration design, and long-term expectations for stability. Understanding structural differences helps patients avoid assumptions that all implant types perform identically once placed.
Structural distinctions also influence how dentists approach treatment planning when bone volume, spacing, or surgical tolerance limits traditional options. Mini implants are selected intentionally for defined indications rather than as a universal alternative. Their design offers advantages in certain anatomical contexts while introducing specific constraints under functional load. PHD Dental weighs these tradeoffs carefully during evaluation. Responsible selection depends on understanding how structure governs performance.
Mini implants feature a significantly narrower diameter than standard implant systems, which changes how the implant engages surrounding bone during placement and function. Reduced width allows placement in areas with limited bone volume where wider implants may require grafting or staged preparation. However, narrower diameter also reduces total surface contact between implant and bone. This structural reality places greater emphasis on bone quality and placement accuracy. Dentists account for these factors when evaluating suitability.
How Implant Diameter Influences Initial Stability
Initial stability depends on how effectively the implant threads engage available bone at placement. A smaller diameter limits surface area available for mechanical engagement. Dentists therefore assess bone density carefully before selecting mini implants. Stability evaluation influences loading decisions and restoration planning.
Why Bone Density Plays a Larger Role With Mini Implants
Higher bone density provides stronger resistance to micromovement around narrow implants. Lower density bone increases mechanical risk when surface contact is limited. Dentists incorporate density findings into candidacy decisions. Structural compatibility supports predictable outcomes.
Mini implants are engineered to support lower functional loads compared to standard implant systems. Their reduced diameter changes how chewing forces transfer through the implant into surrounding bone. Dentists evaluate anticipated bite forces to determine whether they fall within safe limits for mini implants. Load assessment becomes central to appropriate case selection. Long-term performance depends on managing these forces realistically.
How Dentists Evaluate Functional Load Expectations
Dentists analyze bite patterns, opposing dentition, and restoration type to estimate functional demand. These factors help determine whether forces can be distributed safely across mini implants. Load evaluation guides restoration design and number of implants used. Proper assessment reduces overload risk.
Why Force Concentration Affects Long-Term Stability
Concentrated forces increase stress at the bone implant interface. Sustained overload can accelerate bone remodeling or compromise integration. Managing force distribution supports mechanical stability. Structural limits define safe application.
Placement techniques for mini implants differ from those used for standard diameter systems. Mini implants often require less extensive osteotomy preparation, but demand higher placement precision. Reduced diameter allows less tolerance for angulation or depth error. Dentists adapt surgical techniques accordingly to protect bone and implant stability. Technique selection influences healing response.
How Placement Technique Shapes Early Healing Response
Less invasive preparation may reduce surgical trauma to surrounding tissues. Healing response depends on both technique and bone condition. Dentists monitor early stability carefully following placement. Surgical precision supports controlled integration.
Why Accuracy Is Critical With Narrow Implants
Smaller implants provide less margin for positional correction. Minor placement errors can affect load distribution significantly. Accurate angulation and depth protect long-term performance. Precision remains essential.
Restorations supported by mini implants require specific design considerations due to structural limitations. Dentists evaluate restoration size, weight, and leverage carefully during planning. Heavier restorations increase stress on narrow implants. Design constraints influence material choice and contour. Restoration planning aligns with implant capacity.
How Restoration Design Is Modified for Mini Implants
Dentists select lighter materials and conservative contours for restorations supported by mini implants. Design adjustments reduce stress concentration at the implant interface. Restoration geometry supports force management. Adaptation protects structural integrity.
Why Some Restorations Are Not Appropriate for Mini Implants
Certain restorations generate forces beyond what narrow implants can tolerate safely. Using mini implants in these situations increases mechanical risk. Dentists avoid inappropriate applications intentionally. Responsible selection protects patient outcomes.
What the Mini Dental Implant Placement Process Involves

The placement process for mini implants follows a carefully controlled clinical sequence that reflects their smaller diameter and narrower tolerance for error. Dentists approach mini dental implants in Inglewood by prioritizing precision, bone preservation, and realistic load expectations rather than relying on generalized implant protocols. Each stage of placement is designed to limit unnecessary trauma while achieving sufficient primary fixation for the intended restoration. Because mini implants offer less opportunity for post-placement correction, each decision is made deliberately rather than assumed. This process emphasizes control and predictability rather than speed.
Placement planning also accounts for the limited margin for error inherent to narrow-diameter implant systems. Dentists rely heavily on imaging, insertion control, and anatomical mapping to reduce uncertainty during surgery. Surgical decisions are adjusted to patient-specific bone conditions rather than standardized implant spacing assumptions. This individualized approach limits mechanical stress that may not be apparent immediately after placement. Careful sequencing reflects the structural constraints of mini implants.
Before placement begins, dentists gather detailed imaging to evaluate bone dimensions, density, and proximity to anatomical structures. Imaging data guides decisions about implant length, angulation, and depth to avoid encroachment on adjacent roots or nerves. Planning focuses on identifying bone regions capable of resisting rotational and vertical forces after placement. These findings determine whether placement can proceed safely without preparatory intervention. Accurate planning reduces intraoperative adjustments that can compromise bone integrity.
How Imaging Shapes Placement Strategy
Three-dimensional imaging allows dentists to visualize internal bone contours and spatial limitations that are not detectable during surface examination. This information informs precise trajectory planning and depth control before surgical instrumentation begins. Imaging also clarifies where reduced bone volume may affect primary fixation. Strategic use of imaging minimizes reliance on tactile feedback alone during placement.
Why Planning Is Especially Important With Mini Implants
Mini implants provide less tolerance for positional deviation once inserted into bone. Minor errors in angulation or depth can significantly alter how forces are transferred during function. Thorough planning compensates for this reduced margin by identifying optimal placement zones in advance.
Mini implant placement typically involves conservative osteotomy preparation to preserve surrounding bone structure. Dentists control insertion torque carefully to avoid microfractures that may weaken early fixation. Technique selection reflects bone density findings rather than standardized insertion thresholds. Excessive force during placement can compromise bone response around narrow implants. Surgical execution prioritizes accuracy over speed.
How Dentists Control Insertion Forces
Dentists monitor resistance continuously during insertion to match torque levels with bone density. Adjustments are made to prevent overstressing cortical bone during engagement. Controlled insertion preserves mechanical stability at the bone–implant interface. These precautions reduce the likelihood of early mobility.
Why Precision Matters During Insertion
Narrow implants allow little opportunity for correction once seated. Inaccurate angulation can increase lateral stress during function. Depth errors may limit restorative alignment options. Precision during insertion directly affects long-term load behavior.
After placement, dentists evaluate whether the implant has achieved sufficient primary fixation to tolerate limited functional exposure. Stability assessment determines whether the implant can support provisional loading or must remain unloaded during early healing. Bite contacts are adjusted to prevent unintended force application. Early functional decisions are guided by measured resistance rather than assumption. These evaluations influence healing conditions.
How Dentists Assess Primary Stability
Dentists assess insertion resistance, tactile feedback, and implant response during placement. Imaging may be reviewed to confirm seating and orientation. Stability findings determine whether early functional contact is appropriate. These assessments prevent premature loading.
Why Early Force Management Is Necessary
Mini implants are more sensitive to overload during early healing due to reduced surface contact. Excessive force at this stage can disrupt early bone attachment. Managing load during this period reduces mechanical failure risk.
Following placement, dentists schedule follow-up visits to evaluate tissue response and implant behavior during early integration. Soft tissue condition and implant mobility are assessed systematically. Patients receive guidance on hygiene practices and activity limitations that influence healing. Follow-up allows clinicians to detect stress or inflammation before bone adaptation is compromised. Early oversight supports controlled integration.
How Follow-Up Visits Support Healing
Dentists evaluate tissue contours, inflammation levels, and patient comfort during early visits. Adjustments are made when localized irritation or early stress patterns appear. These interventions prevent progression toward instability. Follow-up reinforces appropriate healing conditions.
Why Early Detection Prevents Escalation
Subtle changes in tissue response often precede mechanical or biological failure. Identifying these changes early allows corrective action before integration is affected. Timely intervention preserves implant viability.
Why Dentists Recommend Mini Dental Implants in Specific Treatment Situations
Dentists recommend mini dental implants only when specific anatomical, functional, or procedural constraints make other treatment paths less appropriate. This recommendation reflects a deliberate clinical decision rather than a simplified or downgraded alternative to standard implants. Mini dental implants in Inglewood are selected when their structural characteristics align more closely with patient conditions than wider implant systems or non-implant solutions. The decision weighs surgical risk, restorative demands, and long-term maintenance realities together. Understanding these situations helps patients see mini implants as a targeted tool rather than a universal solution.
These recommendations are often made after other approaches have been evaluated and found to introduce greater risk, complexity, or recovery burden. Dentists consider whether modifying bone, altering restoration design, or staging treatment would meaningfully improve outcomes compared to using a narrower implant. In many cases, mini implants allow treatment to proceed without compromising biological limits. This restraint reflects an emphasis on predictability rather than maximal intervention. Clinical judgment guides these choices more than preference or convenience.
Limited bone width can restrict the safe placement of standard diameter implants without preparatory grafting procedures. Dentists may recommend mini implants when existing bone can support a narrower implant without additional surgical modification. This approach avoids altering bone anatomy beyond what is necessary for functional support. Bone limitations are evaluated carefully to ensure stability expectations remain realistic. Mini dental implants in Inglewood are chosen in these cases to respect anatomical boundaries rather than override them.
How Dentists Decide Between Grafting and Mini Implants
Dentists compare the structural benefit of bone grafting against the added surgical risk and healing time. Grafting may not provide proportional benefit when restorative demands are modest. Mini implants can offer sufficient support without extending treatment timelines significantly. This comparison centers on risk versus necessity rather than preference.
Why Avoiding Grafting Can Be Clinically Appropriate
Additional surgical procedures increase healing variables and complication potential. Some patients benefit from a simpler surgical pathway when load demands are limited. Avoiding grafting preserves existing anatomy. Clinical appropriateness depends on balancing benefit against burden.
Not every restoration generates the same functional demand on an implant. Dentists may recommend mini implants when the intended restoration places limited load on supporting structures. Smaller restorations allow narrower implants to perform within safe mechanical limits. This alignment between restoration size and implant capacity supports longevity. Mini dental implants in Inglewood are used when restorative goals remain compatible with reduced implant diameter.
How Restoration Type Influences Implant Selection
Dentists evaluate whether a crown, bridge component, or stabilization device will exert excessive force. Restoration geometry and material selection affect load transfer. Smaller restorations reduce leverage forces on the implant. Implant choice follows restorative demand.
Why Oversizing Implants Is Not Always Beneficial
Larger implants may require unnecessary bone modification. Excessive intervention does not always improve outcomes. Matching implant size to function reduces biological disruption. Proportional planning supports long-term success.
Some patients present medical or anatomical factors that favor reduced surgical intervention. Dentists may recommend mini implants when minimizing surgical trauma supports safer healing. Reduced osteotomy preparation can lower stress on surrounding bone and tissue. Medical history influences how aggressively treatment should proceed. Mini dental implants in Inglewood may align better with these constraints.
How Medical Considerations Shape Implant Recommendations
Healing capacity, medication use, and systemic conditions affect surgical planning. Dentists adapt treatment to reduce complication risk. Conservative approaches prioritize safety. Medical context guides implant selection.
Why Surgical Restraint Can Improve Predictability
Less invasive procedures reduce variables during healing. Predictability improves when surgical demands remain within patient tolerance. Restraint does not imply lower standards. It reflects informed judgment.
How PhD Dental Coordinates Mini Implant Planning With Long-Term Oral Health
PhD Dental plans mini implant treatment by evaluating how each decision will affect oral function, tissue health, and maintenance demands years after placement. Coordination focuses on aligning surgical placement with restorative design, hygiene access, and bite behavior rather than isolating the implant as a standalone procedure. Mini dental implants in Inglewood are considered within the broader context of how the mouth adapts to daily forces and long-term care routines. This planning model prioritizes durability and serviceability over short-term procedural convenience. The goal is to preserve oral health stability while meeting realistic restorative objectives.
Long-term coordination also requires anticipating how future dental needs may intersect with today’s implant decisions. PhD Dental evaluates whether current planning will allow adjustments, repairs, or alternative treatments later without creating avoidable constraints. This foresight shapes placement position, restoration contours, and material selection from the outset. Patients benefit from a plan that remains flexible rather than fragile over time. Strategic coordination supports sustained oral health rather than episodic intervention.
Bite behavior influences how forces travel through implants and surrounding bone during everyday function. PhD Dental evaluates occlusal patterns to determine whether mini implants can operate within safe mechanical limits over time. Placement and restoration contours are adjusted to minimize lateral stress that may exceed implant tolerance. Bite integration planning reduces cumulative wear and tissue irritation. Managing occlusion remains essential for long-term stability.
How Occlusal Analysis Shapes Implant Planning
Dentists analyze contact points, jaw movement, and functional patterns before finalizing implant position. This analysis identifies areas where force concentration may occur during chewing or parafunctional activity. Planning adjustments are made to redirect stress away from vulnerable structures. Occlusal analysis informs both placement and restoration design decisions.
Why Bite Coordination Prevents Progressive Complications
Unmanaged occlusal stress can lead to gradual bone changes or restoration fatigue. Coordinated planning limits force escalation that may develop over time. Preventive adjustments reduce the likelihood of late-stage complications. Long-term oral health depends on managing functional dynamics early.
Restoration design affects how easily patients can maintain hygiene around mini implants. PhD Dental plans contours and emergence profiles that allow cleaning tools to reach critical areas. Restricted access increases plaque accumulation and tissue inflammation risk. Design decisions are evaluated for their impact on daily care routines. Hygiene access planning protects soft tissue health.
How Restoration Contours Influence Cleaning Effectiveness
Convexity, spacing, and margin placement determine whether plaque can be removed consistently. Dentists design restorations to avoid creating sheltered zones beneath prosthetic components. Accessible contours support patient compliance. Effective cleaning reduces inflammatory burden.
Why Tissue Health Depends on Design Choices
Chronic inflammation around implants compromises supporting bone over time. Design that limits hygiene access accelerates tissue breakdown. Planning for cleanability preserves tissue stability. Long-term success requires daily maintenance feasibility.
Mini implant planning includes consideration for how restorations will be serviced or adjusted later. PhD Dental evaluates whether components can be repaired or replaced without disrupting implant stability. Serviceability influences material selection and attachment methods. Planning anticipates wear patterns and maintenance intervals. Future access remains a priority.
How Serviceability Shapes Material and Attachment Decisions
Dentists select materials that balance durability with repair feasibility. Attachment methods are chosen to allow removal when maintenance becomes necessary. These decisions reduce invasive intervention later. Serviceability supports long-term care continuity.
Why Future Flexibility Protects Patient Outcomes
Oral conditions change over time due to wear and health factors. Flexible planning accommodates these changes without major reconstruction. Limiting rigid solutions preserves options. Long-term outcomes benefit from adaptable design.
Mini implant treatment is coordinated with periodontal health, adjacent teeth, and overall restorative planning. PhD Dental evaluates how implants interact with neighboring structures during function and maintenance. Coordination avoids creating isolated solutions that disrupt oral balance. Each decision supports comprehensive care goals. Integrated planning sustains oral health.
How Adjacent Teeth and Structures Are Considered
Dentists assess spacing, contact relationships, and shared load with neighboring teeth. Planning ensures implants do not introduce new stress to compromised areas. Adjacent structures influence placement and restoration geometry. Coordination maintains harmony across the arch.
Why Whole-Mouth Planning Matters With Mini Implants
Focusing narrowly on a single implant overlooks system-wide effects. Integrated planning reduces unintended consequences elsewhere in the mouth. Oral health functions as a connected system. Long-term stability requires comprehensive coordination.
Talk With PhD Dental About Mini Dental Implants in Inglewood Today
Choosing an implant option requires more than identifying what can be placed today, especially when long-term comfort, hygiene access, and functional balance remain priorities. Patients considering mini dental implants in Inglewood benefit from understanding how implant size, placement strategy, and restoration design influence oral health years after treatment. PhD Dental approaches these decisions by explaining not only when mini implants may be appropriate, but also when alternative approaches better protect long-term stability. This clarity allows patients to move forward in this procedure with confidence.
PhD Dental uses consultations to examine how existing bone support, functional bite patterns, and restorative priorities intersect over time, rather than reviewing each factor in isolation. The discussion focuses on tradeoffs, boundaries, and realistic performance expectations. Patients leave knowing not only what treatment involves, but why certain options are recommended or ruled out. This depth of planning helps prevent surprises after care has already begun. Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation and discuss if mini dental implants in Inglewood align with your expectations.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 9:30AM - 6:30PM
- Tue 9:30AM - 6:30PM
- Wed 9:30AM - 6:30PM
- Thu 9:30AM - 6:30PM
- Fri 9:30AM - 6:30PM
- Sat 9:00AM - 4:00PM
- Sun Closed
