
Apicoectomy Dentists in Los Angeles
An apicoectomy procedure targets the end of the dental root directly. The goal is to remove infected tissue in the surrounding area and seal the root tip to reduce the chance of persistent reinfection. This is done in an effort to preserve teeth through targeted surgical access, especially when the alternative may be extraction or ongoing flare-ups that disrupt daily comfort. Patients often consider an apicoectomy when symptoms return, imaging shows a lingering lesion, or the tooth cannot fully stabilize with non-surgical re-treatment alone.
Our apicoectomy dentists in Los Angeles approach treatment planning with an evidence-led focus on infection control and long-term maintainability for the treated tooth. The team evaluates why the infection persists, whether re-treatment alone can predictably resolve it, and what outcomes an apicoectomy should deliver in your specific case. That clarity helps patients feel confident because the recommendation connects to a defined failure point, not to a generic suggestion to “try surgery.” A successful plan should reduce the risk of repeated swelling or sensitivity, preserve bite function, and support a stable result that holds up under everyday use.
Call (323) 269-5437 to schedule a consultation with PhD Dental’s apicoectomy dentists in Los Angeles and get a clear plan for resolving persistent root-tip infection while protecting your natural tooth.
Top-Rated Dentists
in Los Angeles
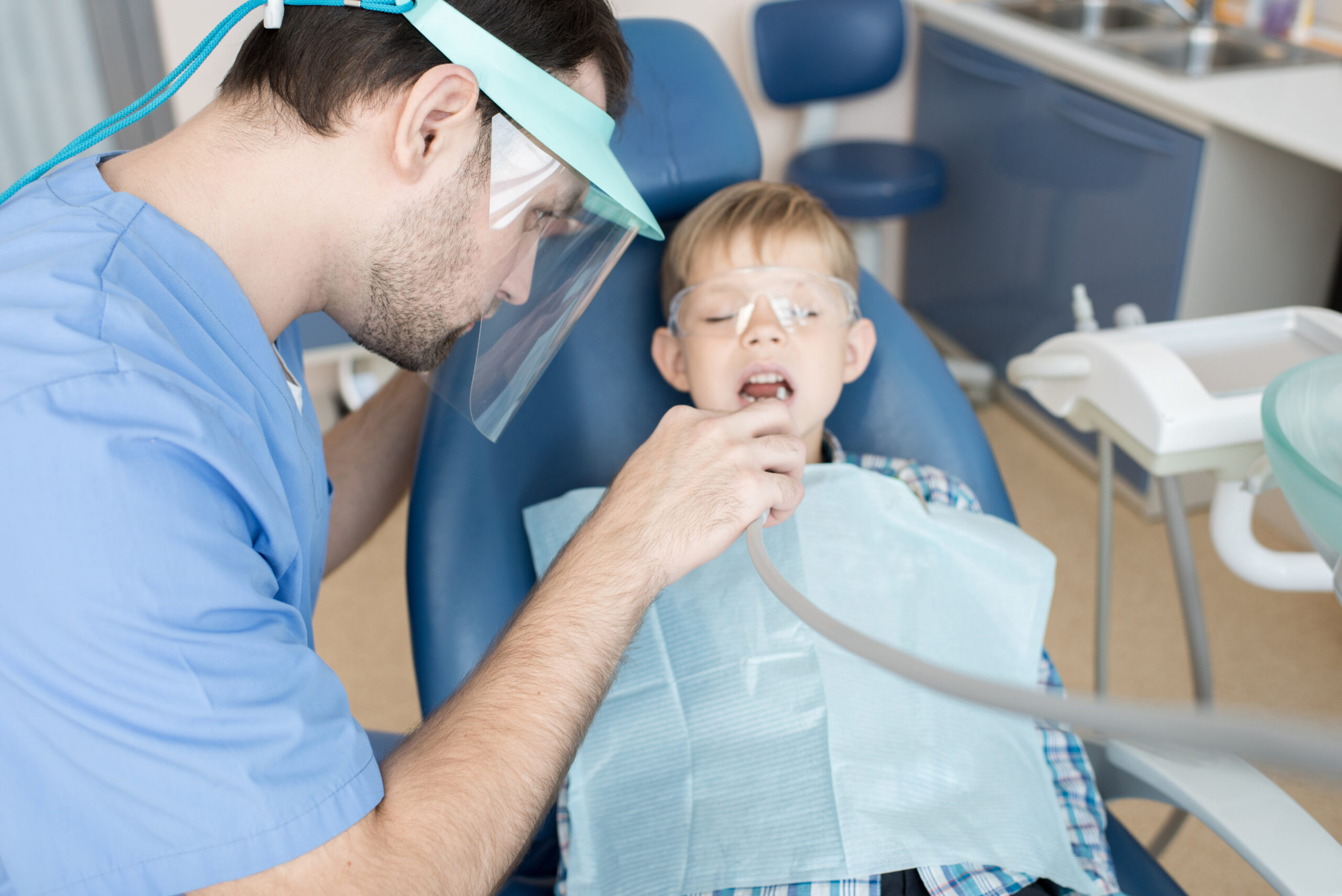
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
How Apicoectomy Dentists in Los Angeles Determine When Root-End Surgery Is Needed

An apicoectomy is a targeted endodontic surgery that addresses infection or inflammation at the root tip when conventional root canal treatment or re-treatment cannot fully resolve the problem. Instead of working through the crown of the tooth, the clinician accesses the root end directly, removes the affected tissue, and seals the root tip to reduce reinfection risk. Patients often feel more confident in the recommendation when the dentist explains the specific reason the tooth needs root-end access, since apicoectomy decisions rely on case details rather than a routine escalation.
At PhD Dental, our Los Angeles dental apicoectomy team focuses on why the tooth has not stabilized, such as complex anatomy near the apex, a persistent lesion that has not resolved, or limitations that make re-treatment less predictable. This clarity helps patients understand that the procedure targets a defined failure point rather than “doing more treatment” by default. The plan should also outline what the surgery is designed to accomplish, including reducing recurring flare-ups and supporting tissue healing around the root tip. When the recommendation connects directly to the tooth’s structure and the infection pathway, patients can make the decision with a clearer sense of purpose and expected outcomes.
Apicoectomy treatment focuses on the apex, which is the small tip of the tooth root where infection can persist in complex anatomy. This approach allows the clinician to remove inflamed tissue and address the part of the canal system that may not be reachable through a standard re-treatment path. When the goal is tooth preservation, root-end surgery can provide a clear, controlled way to resolve a localized failure point.
How the Root Tip Becomes a “Problem Zone” After Prior Root Canal Therapy
Some teeth have tiny canal branches, curves, or anatomical variations that make complete cleaning difficult from inside the tooth. Even when most of the canal looks well treated, bacteria can persist near the apex and continue to irritate surrounding tissue. Patients benefit from understanding that this is an anatomy-driven limitation, not a sign that the tooth was necessarily treated incorrectly.
Why Root-End Sealing Can Improve Long-Term Stability in Certain Cases
Removing the root tip alone is not the full solution, because reinfection risk depends on sealing the pathway at the apex. A root-end seal helps block communication between bacteria and surrounding tissue, which supports more predictable healing. Patients often value this detail because it explains why apicoectomy involves both removal and sealing, not just tissue cleanup.
An apicoectomy is usually recommended when findings point to a localized problem that has not responded to non-surgical options. Those findings often appear on imaging, through symptom patterns, or through evidence of persistent inflammation around the root end. A trustworthy recommendation ties the procedure to these measurable indicators so the patient understands why a targeted surgical solution fits the situation.
Persistent Lesions or Inflammation Seen on Dental Imaging
A recurring lesion near the root tip can signal that the tissue remains irritated by bacteria or inflammatory debris. Even if pain is not constant, the lesion may indicate a chronic process that can flare unexpectedly. Patients appreciate when the plan explains what the image suggests and what healing should look like after a successful root-end intervention.
When Symptoms Return After Treatment and Suggest Ongoing Root-End Infection in Teeth
Some patients notice recurring tenderness, biting discomfort, swelling, or intermittent gum pimples near the tooth. These signs can suggest a persistent infection pathway that has not been fully eliminated. An apicoectomy may be recommended when the pattern indicates the issue sits at the root end rather than in the coronal portion of the tooth.
Re-treatment can be effective, but it is not always feasible or predictable depending on the tooth’s anatomy and existing restorations. Some teeth have posts, crowns, or structural constraints that make re-entering the canal system difficult without compromising the tooth. Apicoectomy offers an alternative route when the end goal is to preserve the tooth without introducing unnecessary structural risk.
Restorations, Posts, or Canal Blockages That Limit Re-treatment Access
If a tooth has a post or a restoration that would be difficult to remove safely, re-treatment can increase the risk of fracture or loss of the restoration. Calcified canals or internal blockages can also prevent instruments from reaching the apex through the traditional approach. Patients often trust the decision more when the dentist explains why a surgical route provides a more controlled solution than forcing access through the crown.
Why Surgical Access Can Be More Predictable Than Re-Opening the Tooth in an Apicoectomy
A surgical approach can allow direct visualization and treatment of the root end without dismantling restorations that still function well. This can preserve tooth structure while addressing the localized infection source. Patients tend to feel more satisfied when the plan explains that predictability is the primary reason for choosing surgery, not convenience.
Many Los Angeles patients choose apicoectomy because they want to preserve a natural tooth that remains functional and restorable. When the tooth has strong structure and a stable restoration, addressing the root-end failure can be a more conservative preservation path than extraction. A careful plan frames apicoectomy as a targeted salvage procedure, with realistic expectations tied to the tooth’s condition.
Maintaining Bite Function by Resolving a Localized Failure Point
Apicoectomy dentists in Los Angeles often recommend this procedure when a tooth remains structurally sound but continues to show a persistent root-end problem. By treating the apex and surrounding tissue, apicoectomy can help the tooth return to stable function without recurring inflammation. Patients often value this option because it can reduce the need for more extensive replacement decisions when the tooth still has good long-term potential.
How PhD Dental Explains Success Metrics for Apicoectomy Healing
Patients deserve clear expectations about what improvement should look like and what the team will monitor after treatment. Success often includes fewer symptoms, clearer healing signs on imaging over time, and fewer recurrence indicators like swelling or draining tracts. This clarity builds trust because it gives patients concrete markers to track instead of leaving them to guess.
What to Expect During an Apicoectomy Procedure in Los Angeles
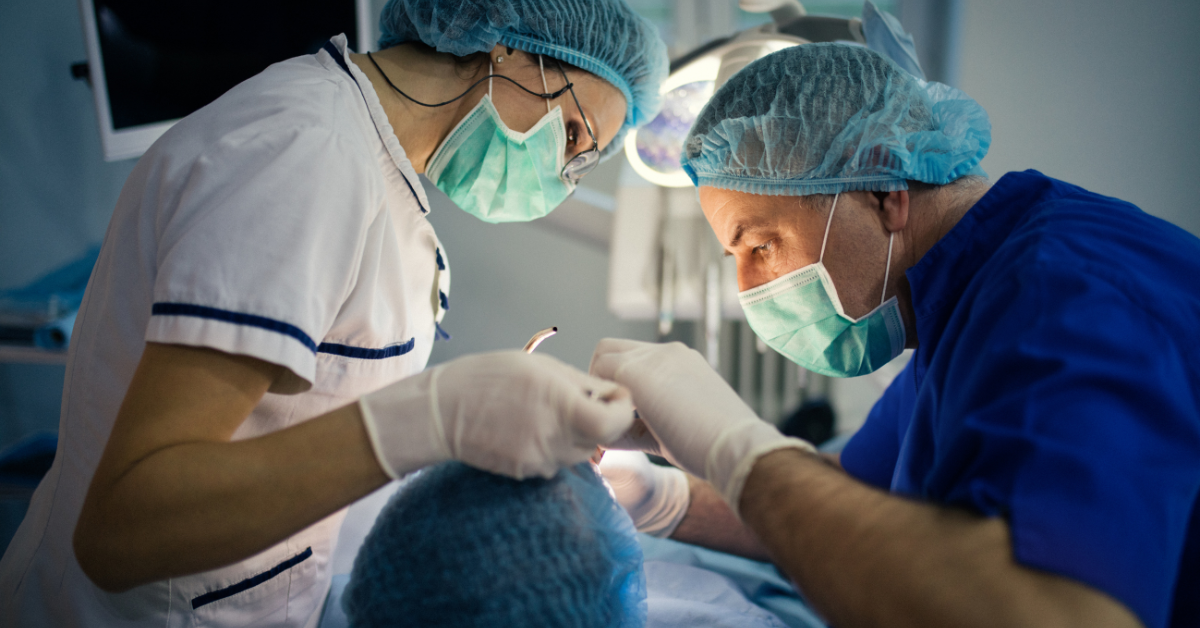
An apicoectomy appointment should feel structured and predictable because precision matters at the root end. The procedure focuses on accessing the root tip through the gum tissue, addressing the infected area directly, and creating a sealed endpoint that supports healing in the surrounding bone. For skilled Los Angeles dentists, the process is built around clear clinical checkpoints so patients understand what is happening, why each step matters, and what signs will be used to confirm a stable result.
Before the procedure begins, the clinical team confirms the tooth, the root involved, and the exact area that needs root-end access. Planning also considers surrounding structures and the most direct route to the apex so the approach stays controlled and conservative. Patients tend to feel more confident when they know the plan is built around specific anatomy rather than a generic template.
Imaging Review and Site Mapping for Root-End Accuracy
Imaging helps the team locate the root tip precisely and assess the surrounding bone and tissue condition. Accurate mapping reduces guesswork and supports a cleaner, more efficient procedure. Patients often appreciate that careful planning is part of what makes the outcome more predictable.
How PhD Dental Explains Procedure Goals Before Treatment Begins
Patients should understand the procedure’s practical goals, including removing the infection source at the root end and sealing the pathway that can lead to reinfection. Our team explains which symptoms should improve and monitors healing over time. This clarity builds trust because it replaces vague reassurance with clear outcome targets.
Dentists typically complete an apicoectomy with local anesthesia to keep the area numb and controlled throughout the appointment. Our team also plans comfort through thoughtful pacing, clear communication, and predictable transitions between steps so the patient stays informed rather than surprised. Patients often value this approach because the team manages comfort through technique and clarity, not vague promises.
Keeping the Procedure Calm and Predictable Through Step-by-Step Communication
Patients tend to tolerate procedures better when they know what to expect next and how long each stage will last. A calm, steady explanation helps reduce tension and supports a more cooperative experience. Clear communication also makes the visit feel more professional and trustworthy because nothing feels rushed or unclear.
What Patients Can Expect to Feel During an Apicoectomy Procedure in Los Angeles
Most patients feel pressure and vibration sensations rather than sharp pain when anesthesia is working as intended. The team checks numbness before proceeding and adjusts as needed to keep the experience controlled. This approach supports satisfaction because patients know the practice prioritizes comfort and clear feedback throughout the appointment.
Apicoectomy dentists in Los Angeles create access through the gum tissue to reach the root end and the area of infection in the surrounding bone. This step is done carefully to keep the field visible and controlled so the root tip can be treated precisely. Patients often feel reassured when they understand that direct access is what makes apicoectomy effective in cases where internal re-treatment is not enough.
How the Root-End Area Is Exposed Without Compromising Nearby Structures
The team uses a conservative approach to expose the necessary area while protecting adjacent tissues. Visibility matters because the clinician needs direct access to remove affected tissue and prepare a clean root-end site. This precision helps reduce the chance of leaving behind infected material that could continue to irritate the area.
Why Clean Visibility Supports Better Healing Outcomes After an Apicoectomy
A controlled field allows the dentist to decontaminate the area more completely and prepare the root end more accurately. When the dentist can see the treatment area clearly, they can remove the problem source with precision instead of relying on feel alone. Patients benefit because the team’s careful execution promotes more predictable healing trends.
Once the dentist establishes access, they remove the affected tissue and treat the root tip directly. The dentist prepares and seals the root end to stop bacteria from migrating into the surrounding tissue. Dental patients often value this explanation because it shows why sealing plays a central role and why an apicoectomy can succeed when repeated cleaning alone can’t.
How Apicoectomy Dentists in Los Angeles Prepare the Root End for a Secure Seal
The clinician creates a preparation at the root end so the seal can sit in a stable, clean position. This step aims to reduce pathways for bacteria and create a more predictable endpoint for the canal system. A well-prepared seal supports healing because it limits continued irritation from bacterial leakage.
How the Seal Supports Long-Term Tooth Preservation
A successful apical seal reduces reinfection risk and allows the surrounding tissue to calm down over time. It supports tooth preservation by addressing the root-end failure point while keeping the rest of the tooth intact. Patients often feel more confident when they understand that the seal protects the tooth long after the appointment ends.
After treatment, the dentist closes the site to support stable healing and protect the area as early recovery begins. Our team gives patients clear guidance on what feels normal in the first few days and which warning signs should prompt a call to the practice sooner. PhD Dental emphasizes realistic expectations so patients leave the office feeling prepared and supported, not unsure.
Follow-Up Timing and Monitoring Milestones for Apicoectomy Healing
Our team tracks healing through symptom improvement and imaging changes over time because bone and tissue recovery progresses gradually. We explain when follow-up visits occur and which markers show that healing is moving in the right direction. Patients often value this structure because it confirms progress instead of leaving them to guess.
How PhD Dental Supports Patients If Symptoms Persist or Return
Patients deserve a plan for what happens if discomfort does not improve as expected or if symptoms return later. Clear communication about follow-up and response steps reinforces trust because it shows the practice remains accountable after the procedure. This approach supports satisfaction because patients know they have guidance and continuity beyond the appointment day.
How Apicoectomy Dentists in Los Angeles Evaluate Risks and Long-Term Outcomes
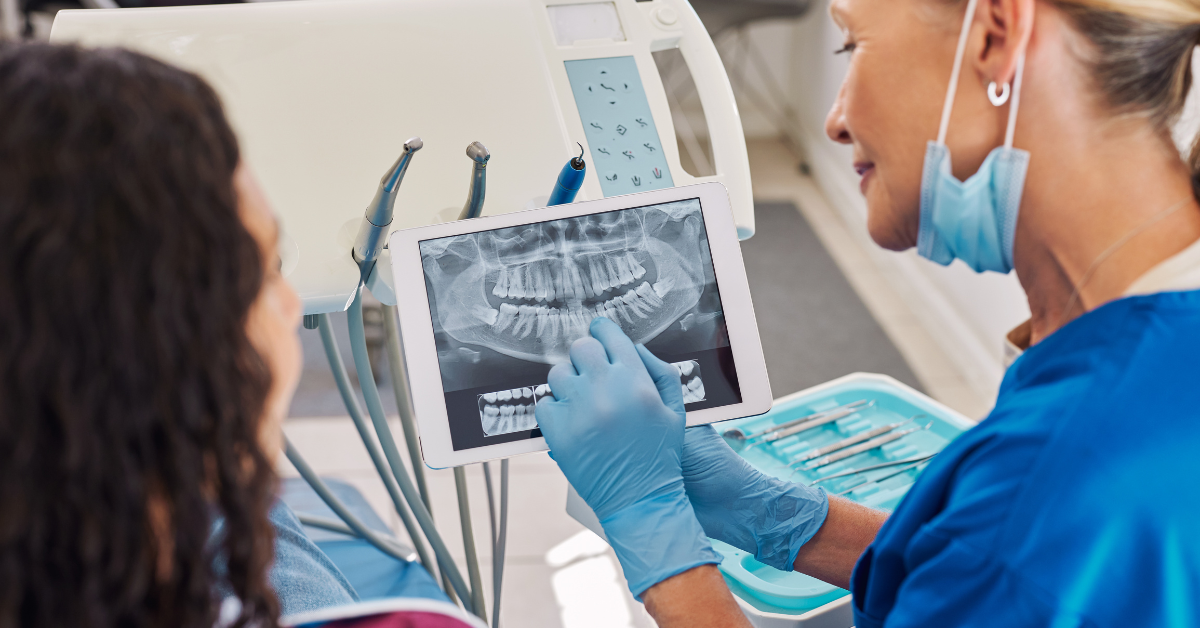
Apicoectomy outcomes depend on why the tooth failed to stabilize in the first place, how localized the problem is, and whether the tooth remains structurally strong enough to justify preservation. A trustworthy discussion should separate predictable healing patterns from the factors that can lower success, such as complex root anatomy, large lesions, or cracks that compromise the tooth. PhD Dental focuses on setting measurable expectations so patients understand both the upside of saving a natural tooth and the limits that can affect long-term reliability.
Apicoectomy success tends to be higher when the tooth has a clear, localized root-end issue and the surrounding structures can heal into a stable baseline. The best cases involve a tooth that remains restorable and functional, with a failure point that is limited to the apex rather than a broader structural problem. Patients usually feel more confident when the dentist explains which factors are working in their favor and which ones require a more cautious prognosis.
Tooth Integrity and Restorability as the Foundation for Long-Term Stability for Los Angeles Dental Patients
A tooth can only benefit from an apicoectomy if it can still handle everyday bite forces after the infection resolves. Structural issues such as extensive fractures, severe decay, or compromised restorations can reduce predictability even if the root-end problem is treated well. Our apicoectomy dentists in Los Angeles evaluate restorability carefully because long-term satisfaction depends on stability after healing, not just short-term symptom relief.
Why Cracks and Structural Defects Change a Dentist’s Recommendation
A crack can create an ongoing pathway for bacteria and can undermine the tooth’s ability to remain stable under load. Even when the root end heals, a cracked tooth may continue to flare or become painful when chewing. Patients appreciate direct guidance here because it prevents investing in treatment that cannot reliably protect the tooth long term.
Success rates vary because studies group different tooth types, lesion sizes, and patient factors, and those differences can shift outcomes. A meaningful discussion focuses on your specific risk profile rather than quoting a single number that ignores anatomy and diagnosis details. Patients tend to trust the recommendation more when the clinician explains what “success” means clinically and how it will be confirmed over time.
What “Success” Means for Apicoectomy Dentists in Los Angeles
Clinical success typically includes symptom resolution and evidence of healing trends on imaging as the surrounding bone repairs. The timeline matters because bone changes occur gradually, and improvements may be tracked across follow-up milestones rather than immediately. This explanation helps patients feel prepared, since a stable outcome involves verification over time instead of instant confirmation.
Realistic Healing Benchmarks and What They Indicate
Early improvements often involve fewer flare-ups, less biting tenderness, and reduced swelling indicators. Longer-term benchmarks rely on imaging changes that show the lesion shrinking and bone filling in as the area stabilizes. Patients value these benchmarks because they make progress measurable and reduce anxiety about what normal healing should look like.
Every surgical procedure carries risk, and apicoectomy risks depend on tooth position, root anatomy, and nearby structures. Most concerns involve healing variability, lingering discomfort, or incomplete resolution when the underlying problem extends beyond the root tip. PhD Dental addresses risks in plain language so patients can weigh tooth preservation against alternative options with clear expectations.
Infection Persistence and Delayed Healing as the Most Common Concerns
Some cases heal more slowly or show incomplete resolution if bacteria persist in complex anatomy or if the lesion was extensive. Delayed healing does not always mean failure, but it can require more monitoring or additional intervention if symptoms continue. Patients feel more confident when the plan includes what will be tracked and what would trigger a change in direction.
Why Lesion Size and Anatomy Can Affect Predictability
Large lesions can take longer to heal because the body must rebuild more tissue and bone. Complex root structures can also make it harder to fully eliminate the infection source, even with precise treatment. A clear explanation builds trust because it connects risk to anatomy rather than presenting complications as random.
For many patients, the value of apicoectomy is preserving a natural tooth that still contributes to function and maintains bite continuity. Long-term outcomes are strongest when the tooth remains stable, maintainable, and free of recurring infection signs after healing milestones are met. Patients appreciate a comparison framed around durability and maintenance realities, since replacement decisions carry their own timelines and upkeep requirements.
How Preserving a Natural Tooth Can Support Bite Function Over Time
Keeping a natural tooth can help maintain familiar chewing patterns and reduce the need to adapt to a replacement solution. It can also preserve the way the tooth interacts with neighboring teeth, which can matter for long-term comfort. This perspective supports satisfaction because it focuses on day-to-day performance, not just avoiding extraction.
When PhD Dental May Recommend Moving to Replacement Instead
If the tooth shows structural compromise, repeated failure patterns, or a prognosis that does not support reliable stability, replacement may offer a more predictable long-term result. A clear recommendation should explain why the long-view outcome favors replacement rather than pushing preservation at all costs. Patients tend to trust this approach because it prioritizes durability, function, and avoidable risk control.
Why Clients Choose PhD Dental’s Apicoectomy Dentists in Los Angeles
Apicoectomy dentists need to make careful, case-specific decisions because root-end surgery only makes sense when the tooth still has a strong long-term preservation outlook. Patients often choose PhD Dental because our team focuses on identifying the true reason a tooth has not stabilized after prior endodontic care, then matching the plan to that specific failure point instead of treating surgery as an automatic next step. That approach helps patients feel confident that the recommendation is defensible and targeted, especially when they are deciding between apicoectomy, re-treatment, or extraction. Clear expectations also matter with apicoectomy, and PhD Dental emphasizes measurable success markers so patients understand what improvement should look like and how healing will be monitored over time.
Angelinos also value a practice that treats follow-through as part of the outcome, not as an afterthought. Our apicoectomy dentists in Los Angeles keep care organized around defined checkpoints, communication that stays direct, and planning that protects the tooth’s function once the infection resolves. This level of structure supports long-term satisfaction because patients can see why each step exists and how the plan reduces repeat flare-ups and uncertainty. When a tooth still has strong restorative potential, a well-executed apicoectomy can be the difference between preserving a natural bite and moving into a replacement pathway. The goal is simple, resolve the root-end problem and protect the tooth you still want to keep.
Call (323) 269-5437 or use our contact form to schedule a consultation with PhD Dental and speak with our apicoectomy dentists in Los Angeles about a clear plan for saving your tooth.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 9:30AM - 6:30PM
- Tue 9:30AM - 6:30PM
- Wed 9:30AM - 6:30PM
- Thu 9:30AM - 6:30PM
- Fri 9:30AM - 6:30PM
- Sat 9:00AM - 4:00PM
- Sun Closed
