Call PhD Dental Today for Exceptional Dental Care
BOOK AN APPOINTMENTWisdom Teeth Removal in Inglewood
Wisdom teeth removal is often recommended when third molars begin to affect surrounding teeth, gum health, or jaw comfort rather than simply because they are present. Patients researching wisdom teeth removal in Inglewood are often dealing with pain, swelling, pressure, or uncertainty about if extraction is necessary now or can be delayed safely. Dentists evaluate how wisdom teeth are positioned, how they are erupting, and how they interact with nearby structures before recommending removal. Timing and approach matter, since unnecessary delay or premature extraction can create avoidable issues.
Choosing wisdom teeth removal in Inglewood also involves understanding how anatomy and healing capacity influence outcomes. Treatment planning prioritizes safety, recovery predictability, and long-term oral health. This approach supports informed decision making rather than reactive treatment. If you are considering wisdom teeth removal in Inglewood and want a clear explanation of whether removal is necessary, what risks are involved, and how recovery is managed, call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation today.
Top-Rated Dentists
in Los Angeles
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
- How Dentists Decide Whether Wisdom Teeth Removal Is Necessary
- When Timing Matters for Wisdom Teeth Removal in Inglewood
- What to Expect During a Wisdom Teeth Removal Procedure
- How PhD Dental Approaches Wisdom Teeth Removal With Long-Term Oral Health in Mind
- Speak With PhD Dental About Wisdom Teeth Removal in Inglewood Today
How Dentists Decide Whether Wisdom Teeth Removal Is Necessary
Dentists do not recommend extraction simply because wisdom teeth exist, but because their position, development, or impact on surrounding structures creates a foreseeable problem. Evaluating the need for wisdom teeth removal in Inglewood involves assessing how third molars interact with adjacent teeth, gum tissue, and jawbone over time. Some wisdom teeth remain asymptomatic initially while still posing structural or hygienic risks that progress silently. Dentists focus on predicting future complications rather than reacting only to current discomfort. This decision process prioritizes prevention of damage rather than routine removal.
The evaluation also considers whether monitoring remains a safe option or whether delay increases surgical complexity and recovery risk. PHD Dental weighs anatomical findings against patient age, healing capacity, and oral health history. Imaging and clinical examination work together to clarify whether wisdom teeth are likely to erupt normally or create long-term problems. Removal is recommended when risk trends outweigh the benefits of retention. Thoughtful decision making reduces unnecessary intervention while avoiding preventable complications.

The direction and angle at which wisdom teeth erupt strongly influence whether they can be maintained safely. Dentists assess whether third molars are upright, angled forward, angled backward, or horizontally positioned within the jaw. Improper eruption paths increase the likelihood of impaction against adjacent teeth or bone. Limited space in the jaw often prevents full eruption even when teeth appear partially visible. Position analysis forms a critical part of determining necessity for removal.
How Imaging Reveals Eruption Limitations
Panoramic and three-dimensional imaging allow dentists to see how wisdom teeth are oriented beneath the gum line. These images reveal whether roots are developing in positions that restrict eruption. Imaging also clarifies whether bone coverage prevents natural emergence. Visualizing these limitations guides clinical judgment.
Why Eruption Angle Predicts Future Problems
Angled or horizontal wisdom teeth often apply pressure to second molars. This pressure can contribute to enamel damage or crowding over time. Poor angles also create areas that trap bacteria. Predictive assessment helps prevent these outcomes.
Wisdom teeth can compromise the health of neighboring teeth even without causing pain. Dentists evaluate whether third molars create contact points that are difficult to clean or cause chronic gum inflammation. Food trapping and bacterial accumulation increase decay and periodontal risk around second molars. Over time, these effects may result in irreversible damage. Risk assessment focuses on protecting surrounding structures.
How Dentists Identify Hidden Damage Risks
Clinical examination looks for gum pocketing and inflammation near wisdom teeth. Imaging reveals early decay or bone changes that are not visible externally. Dentists correlate these findings with patient hygiene challenges. Hidden risks often drive removal recommendations.
Why Adjacent Tooth Health Influences Decisions
Preserving healthy second molars is a priority in treatment planning. Wisdom teeth that threaten adjacent teeth create a long-term liability. Preventive removal protects function and reduces future restorative needs. Decisions favor preserving stronger teeth.
Repeated infections around partially erupted wisdom teeth signal ongoing risk. Dentists review any history of swelling, pain, or difficulty opening the jaw. Even intermittent symptoms suggest that bacteria are accessing deep tissue spaces. Recurrence often indicates that conservative management will remain ineffective. Symptom history informs the urgency of removal.
How Dentists Evaluate Infection Patterns
Dentists ask about frequency, duration, and severity of prior episodes. Clinical signs such as redness or discharge are documented. Imaging may show chronic changes consistent with infection. Pattern recognition supports decision making.
Why Recurrent Infections Rarely Resolve Permanently
Partially erupted teeth create persistent pathways for bacteria. Antibiotics may reduce symptoms temporarily but do not eliminate the source. Ongoing infection increases tissue damage risk. Removal addresses the underlying cause.
Age influences both surgical difficulty and recovery response. Dentists consider how bone density and root development affect extraction complexity. Younger patients often experience smoother healing and fewer complications. Delaying removal may increase surgical risk as roots mature. Timing plays a role in determining necessity.
How Age Affects Surgical Complexity
As patients age, bone becomes denser and roots lengthen. These changes can complicate extraction and prolong recovery. Dentists factor age into risk assessment. Earlier intervention may reduce difficulty.
Why Timing Shapes Long-Term Outcomes
Proactive removal can prevent future complications. Waiting may increase surgical trauma and recovery time. Dentists balance readiness with risk progression. Timing decisions support safer outcomes.
When Timing Matters for Wisdom Teeth Removal in Inglewood
The timing of wisdom teeth removal can influence surgical difficulty, healing response, and the likelihood of complications more than many patients expect. Dentists consider wisdom teeth removal in Inglewood not only in terms of whether extraction is necessary, but also when intervention offers the safest and most predictable outcome. Changes in jawbone density, root development, and surrounding tissue occur gradually, shifting risk profiles over time. Waiting too long or acting too early can both introduce avoidable challenges depending on individual anatomy. Timing decisions are therefore based on clinical progression rather than age alone.
Dentists also evaluate how current symptoms, imaging findings, and projected development intersect over the coming years. Some wisdom teeth remain stable for extended periods, while others show signs that problems are likely to escalate. Timing recommendations aim to intervene before damage occurs, but not before conditions justify surgery. This balance requires forecasting how anatomy will change rather than reacting only to present discomfort. Thoughtful timing supports safer procedures and smoother recovery.
Age influences how the jawbone responds to surgical intervention and how tissues recover afterward. Younger patients often have less dense bone and partially developed roots, which can simplify extraction and reduce trauma. As patients age, bone becomes more rigid and roots lengthen, increasing resistance during removal. Healing capacity may also change over time. Dentists factor these trends into timing recommendations.
How Bone Density Affects Surgical Difficulty
Denser bone requires more force and instrumentation during extraction. Increased resistance can lengthen procedure time and affect surrounding tissue. Dentists assess bone characteristics through imaging before recommending timing. Anticipating density changes helps manage risk.
Why Earlier Removal Can Reduce Surgical Stress
Removing teeth before full root maturation may limit the need for extensive bone manipulation. Less resistance can translate to a more controlled procedure. Reduced trauma often supports smoother early recovery. Timing decisions reflect these mechanical considerations.
Wisdom teeth that appear stable at one stage may shift position as jaw structures continue to develop. Dentists monitor whether eruption paths are improving or worsening over time. Increasing impaction depth or angulation can complicate future removal. Progressive changes may also increase pressure on adjacent teeth. Timing recommendations account for these evolving patterns.
How Dentists Track Changes in Tooth Position
Serial imaging allows dentists to compare eruption angle and depth over time. Subtle shifts can signal increasing difficulty ahead. Monitoring helps distinguish stable cases from those trending toward complication. Tracking informs proactive decision making.
Why Delayed Removal Can Increase Complexity
As impaction deepens, access becomes more limited. Deeper positioning may place roots closer to nerves or sinus structures. Increased complexity can elevate surgical risk. Timely intervention may avoid these developments.
Intermittent pain or swelling around wisdom teeth often indicates an unstable condition rather than a resolved issue. Dentists evaluate whether symptoms are becoming more frequent or severe. Recurrent inflammation suggests ongoing bacterial access that may worsen. Waiting through repeated episodes can increase tissue damage. Timing recommendations reflect infection patterns.
How Dentists Interpret Recurrent Symptoms
Dentists review how often symptoms occur and how long they last. Clinical signs such as gum pocketing or redness are assessed alongside patient history. Patterns indicate whether conservative management remains viable. Escalation supports removal timing.
Why Repeated Infections Change Risk Profiles
Each infection episode can weaken surrounding tissue and bone. Repeated inflammation increases complication likelihood during surgery. Early removal may prevent cumulative damage. Timing choices aim to interrupt this cycle.
Not all wisdom teeth require immediate extraction, even when removal may eventually be necessary. Dentists sometimes recommend active monitoring when risks remain low and anatomy is favorable. However, prolonged monitoring without clear criteria can delay needed intervention. Timing decisions balance caution with foresight. Clear benchmarks guide when observation should transition to removal.
How Dentists Set Monitoring Thresholds
Dentists define specific changes that would prompt removal, such as increased impaction or symptom recurrence. Imaging intervals are established to reassess risk. Monitoring is structured rather than passive. Thresholds support timely action.
Why Indefinite Delay Is Rarely Recommended
Without defined limits, monitoring can allow problems to progress unnoticed. Delayed action may increase surgical difficulty later. Dentists aim to intervene before risk accelerates. Timing strategy protects long-term oral health.
What to Expect During a Wisdom Teeth Removal Procedure
A wisdom teeth removal procedure is planned as a controlled surgical process rather than a single extraction event. Dentists performing wisdom teeth removal in Inglewood base the procedure on imaging, anatomical assessment, and anticipated difficulty before the appointment even begins. Each phase of the procedure is designed to manage access, protect surrounding structures, and maintain patient comfort throughout surgery. The steps involved can vary depending on impaction depth, root development, and proximity to nerves or sinus structures. Understanding how the procedure unfolds prepares patients for both the surgical experience and the immediate recovery period.
The procedure is also shaped by intraoperative findings that may differ slightly from preoperative imaging. Dentists remain prepared to adjust technique if resistance, access limitations, or tissue response requires modification. These decisions are made in real time to preserve safety rather than adhere rigidly to a predetermined approach. Some procedures progress efficiently with minimal intervention, while others require staged removal to limit trauma. Anticipating this variability allows patients to approach surgery with realistic expectations.
Before the procedure begins, dentists confirm imaging findings, medical history details, and anesthesia plans to ensure surgical readiness. This evaluation includes reviewing root position, bone density, and the relationship of wisdom teeth to nearby anatomical structures. Anesthesia is administered based on the planned level of comfort and procedural complexity. The surgical field is prepared to maintain visibility and control throughout the procedure. Thorough preparation reduces the likelihood of interruption once extraction begins.
How Dentists Establish Surgical Readiness
Dentists verify that anesthesia has taken full effect before proceeding with tissue manipulation. Imaging is reviewed immediately prior to surgery to reconfirm orientation and access points. Instrument selection is finalized based on anticipated resistance and tooth position. These steps allow the procedure to proceed smoothly and deliberately.
Why Preparation Determines Procedural Control
Inadequate preparation can increase discomfort or prolong surgery unnecessarily. Proper setup allows dentists to work methodically rather than reactively. Controlled conditions support precision and reduce tissue stress. Preparation directly influences surgical efficiency and safety.
Once preparation is complete, dentists create access to the wisdom teeth in a way that preserves surrounding bone and soft tissue. For impacted teeth, limited bone removal may be necessary to visualize and reach the crown safely. Dentists expose only what is required to proceed rather than removing excess tissue. Access strategy is tailored to the tooth’s orientation and depth. Careful exposure reduces unnecessary trauma.
How Dentists Determine Access Approach
Imaging guides whether access can be achieved through soft tissue alone or requires bone modification. Dentists evaluate the angle of eruption and available space. Decisions are adjusted intraoperatively based on resistance encountered. Access planning balances visibility with tissue preservation.
Why Conservative Access Reduces Complications
Excessive bone removal can increase post-operative discomfort and prolong healing. Limiting access to what is necessary protects structural integrity. Conservative exposure supports smoother recovery. Precision during access matters.
When wisdom teeth cannot be removed intact due to size or impaction, dentists divide the tooth into smaller sections. Sectioning allows removal through a smaller opening without excessive force. This approach reduces leverage stress on the jaw and adjacent teeth. Dentists remove each segment carefully to maintain control. Sectioning strategy reflects anatomical constraints.
How Dentists Decide When Sectioning Is Required
Teeth with curved roots or deep impaction often require division. Imaging and tactile feedback guide this decision. Dentists section teeth to follow natural root anatomy. This method improves control during extraction.
Why Sectioning Protects Surrounding Structures
Forcing intact removal can damage bone or neighboring teeth. Sectioning reduces pressure and unintended movement. Controlled removal limits collateral impact. Structural preservation remains a priority.
After tooth removal, dentists focus on managing the extraction site to support early healing. The area is inspected for debris, bone fragments, or residual tissue. Bleeding is controlled through pressure and, when appropriate, suturing. Stabilization encourages clot formation and tissue adaptation. Proper site management reduces post-operative complications.
How Dentists Promote Stable Healing Conditions
Dentists clean the site thoroughly before closure. Gauze placement and sutures are used strategically. Instructions are given to protect the clot during early healing. These measures support tissue recovery.
Why Early Stabilization Influences Recovery
Disruption of the extraction site can delay healing and increase discomfort. Stable clot formation protects the underlying bone. Early care reduces complication risk. Site management shapes recovery quality.
Before discharge, dentists review procedure details and recovery expectations with the patient. Instructions cover pain management, swelling control, diet progression, and activity restrictions. Warning signs that require follow-up are explained clearly. Medication use is reviewed to avoid confusion. Clear discharge planning supports safe recovery at home.
How Dentists Tailor Post-Procedure Instructions
Guidance is adjusted based on extraction complexity and patient health factors. Dentists explain when normal activities can resume. Dietary recommendations reflect tissue sensitivity. Customization improves adherence.
Why Understanding Instructions Prevents Setbacks
Missteps during early recovery can disrupt healing. Following guidance reduces the likelihood of complications. Patient understanding supports smoother recovery. Education remains part of care.
Wisdom teeth can place sustained pressure on neighboring molars and create hygiene challenges that increase decay and periodontal risk over time. PhD Dental evaluates whether removal will protect adjacent teeth from progressive damage that may not yet be producing noticeable symptoms. Surgical planning emphasizes preserving surrounding bone that supports nearby teeth and overall jaw structure. Limiting unnecessary bone disruption helps maintain long-term stability and function.
How Adjacent Teeth Influence Clinical Removal Decisions
Dentists assess contact relationships, gum tissue health, and enamel condition near wisdom teeth during clinical examination. Imaging is reviewed to identify early bone loss or decay that may not be visible during surface evaluation. These findings help determine whether retaining wisdom teeth presents cumulative risk to neighboring structures. Adjacent tooth health plays a decisive role in removal timing.
Why Jawbone Preservation Affects Future Oral Stability
Jawbone surrounding wisdom teeth contributes to structural support throughout the dental arch. Excessive bone removal can complicate future restorative or orthodontic procedures. Preserving bone volume maintains flexibility for later treatment needs. Long-term oral planning depends on structural conservation.
Surgical technique is selected based on how tissues are expected to heal and function years after extraction rather than how quickly removal can be completed. PhD Dental plans access, sectioning, and instrumentation carefully to avoid unnecessary trauma to bone and soft tissue. Conservative technique helps preserve anatomy that may be required for implants, orthodontic movement, or restorative care later in life. Avoiding excessive trauma protects future treatment options.
How Technique Selection Shapes Long-Term Anatomical Outcomes
Dentists choose surgical approaches that minimize leverage stress on the jaw during extraction. Controlled sectioning reduces the need for extensive bone removal. Precision during surgery limits unintended tissue disruption. Technique decisions influence long-term anatomical integrity.
Why Preserved Anatomy Supports Future Dental Planning
Future dental treatments often rely on existing bone and tissue contours for stability. Altered anatomy can restrict available treatment paths later. Preserving natural structures supports adaptability in care planning. Long-term outcomes benefit from restraint.
Wisdom teeth removal is evaluated alongside current and anticipated dental treatments rather than treated as an isolated procedure. PhD Dental considers how extraction timing aligns with orthodontic care, restorative planning, or periodontal management needs. Coordinated scheduling helps avoid unnecessary treatment delays or overlapping recovery periods. Integration supports continuity across all phases of care.
How Dentists Align Removal Timing With Other Treatments
Treatment timelines are reviewed in relation to extraction planning and healing requirements. Dentists consider how recovery may affect other scheduled procedures. Adjustments are made to reduce disruption. Coordinated timing supports efficient care progression.
Why Integrated Planning Prevents Future Complications
Treating wisdom teeth removal independently can complicate later dental procedures. Overlapping healing phases increase patient burden and risk. Integrated planning reduces avoidable conflicts. Long-term oral health benefits from coordination.
Speak With PhD Dental About Wisdom Teeth Removal in Inglewood Today
Deciding if and when to proceed with wisdom teeth removal is easier when the discussion focuses on long-term oral health rather than immediate discomfort alone. Patients considering wisdom teeth removal in Inglewood benefit from a consultation that explains how anatomy, timing, and surgical approach can influence your dental care options. PhD Dental uses this visit to review imaging findings, discuss projected changes over time, and explain how removal decisions are made with future oral health in mind.
A consultation also provides space to understand surgical expectations, recovery planning, and how wisdom teeth removal in Inglewood fits into a broader dental care strategy rather than standing alone. Dentists explain potential risks, healing considerations, and how monitoring or removal decisions may change as conditions evolve. Patients leave knowing why a recommendation is made, giving them the clarity they need. Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation today.
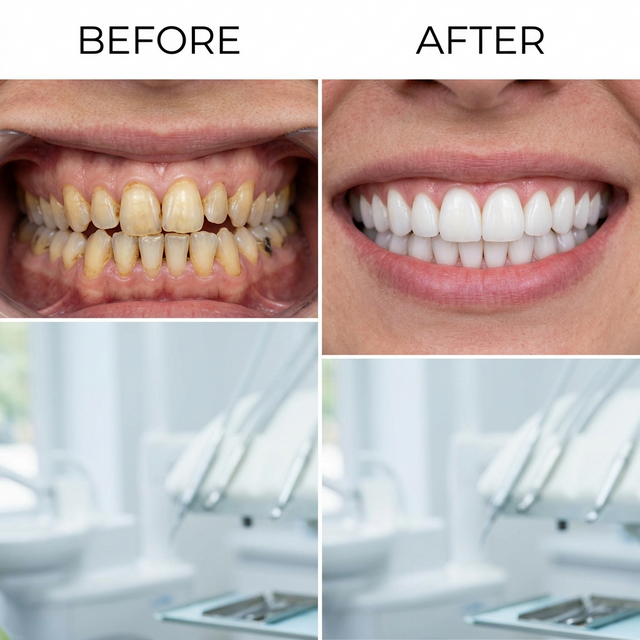
Before and After
Lorem ipsum dolor sit amet
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Sed metus mi, vehicula ut urna vel, ultrices aliquam ipsum. Mauris sit amet ipsum et ipsum interdum blandit ac id justo. Pellentesque efficitur egestas neque, quis sagittis diam venenatis a. Nulla et porttitor purus. Curabitur aliquet consequat varius. Praesent tincidunt, dui facilisis bibendum consequat, felis purus porta erat, sed luctus urna lacus eu tortor. Maecenas dignissim metus vel ex ultricies laoreet. Praesent felis est, ornare sodales eros non, tempus condimentum lectus.
LEARN MOREGet in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed