Wisdom Tooth Extractions in Los Angeles
Wisdom Tooth Extractions in Los Angeles are often recommended when third molars threaten long-term stability, whether through impaction, repeated inflammation, pressure on adjacent teeth, or decay that becomes difficult to manage at the back of the mouth. Furthermore, wisdom teeth can create problems quietly, especially when they sit partially erupted or remain trapped under the gumline where bacteria collect and cleaning stays inconsistent. Removal focuses on preventing predictable complications, including infection episodes, damage to neighboring molars, and crowding pressure that can affect bite comfort over time. Patients often choose extraction when symptoms recur or when imaging shows the tooth position makes future problems likely.
PHD Dental approaches wisdom tooth removal with a planning-first mindset that prioritizes safe access, predictable healing, and a clear understanding of the tooth’s anatomy and eruption pattern. The team evaluates how each wisdom tooth sits relative to surrounding bone, soft tissue, and neighboring teeth so the treatment plan matches the complexity of the case. This clarity builds confidence because patients understand why extraction is recommended and what the procedure is designed to prevent. A well-managed outcome should reduce repeated flare-ups at the back of the mouth, protect adjacent teeth from long-term wear or decay, and support a smoother hygiene routine in a hard-to-reach area.
Call (323) 269-5437 to schedule a consultation with PHD Dental for wisdom tooth extractions in Los Angeles and get a clear plan for preventing complications and protecting long-term oral stability.
Top-Rated Dentists
in Los Angeles
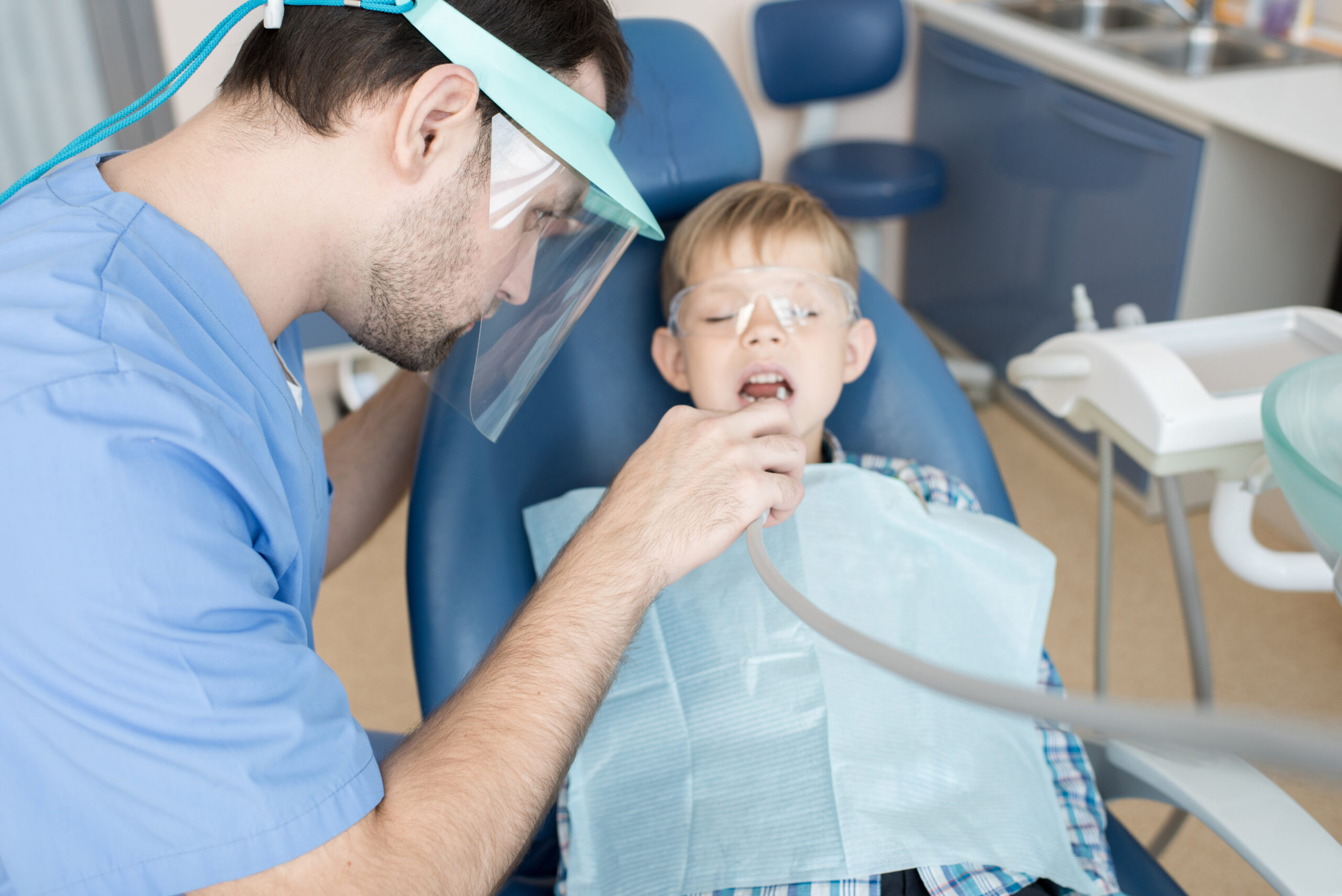
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
Common Signs of Impacted or Problem Wisdom Teeth in Los Angeles Patients
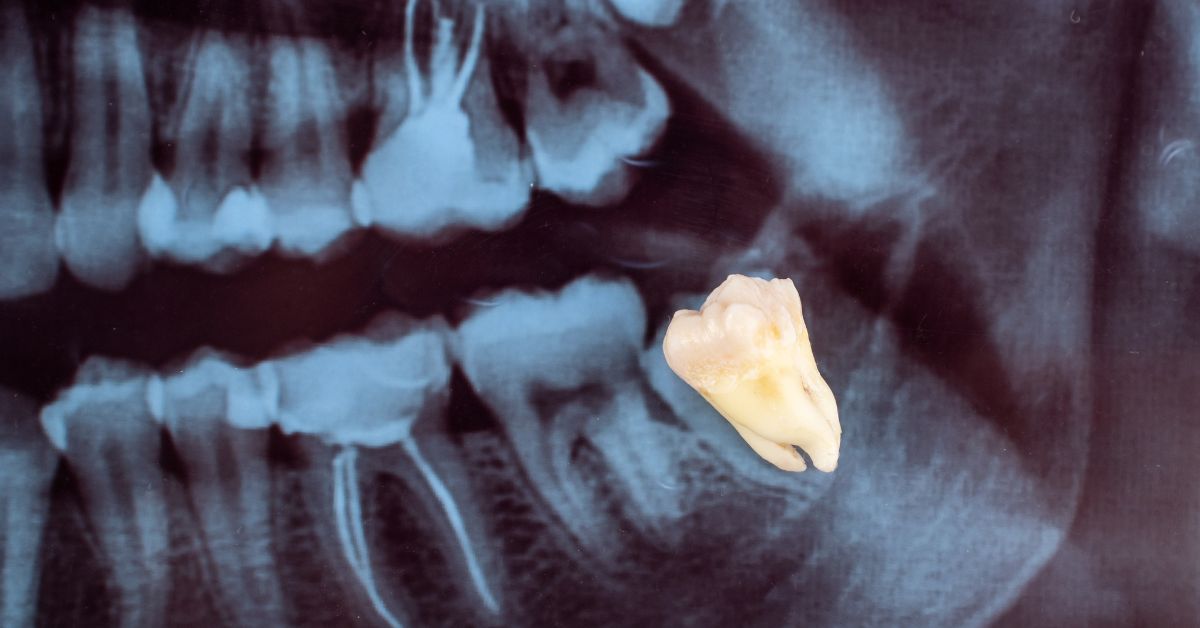
Problem wisdom teeth often announce themselves through recurring patterns, not a single dramatic symptom. The signs usually relate to limited space, partial eruption, or a position that traps bacteria and irritates surrounding tissues. Patients tend to feel more confident in the decision to remove wisdom teeth when they can connect symptoms to a clear mechanical cause, since third-molar issues often repeat until the underlying position problem is addressed. At PHD Dental, the goal is to identify whether you are dealing with a one-time irritation or a predictable cycle driven by the tooth’s position and access limitations. That distinction matters because recurring inflammation often signals that home care cannot consistently reach the problem area. A focused exam can also clarify whether the wisdom tooth is affecting the neighboring molar, which can turn a small issue into a larger repair later. When the cause is defined clearly, patients can act earlier and avoid repeated flare-ups that disrupt eating, sleep, and daily comfort.
When a wisdom tooth only partially breaks through the gum, the tissue can form a flap that traps food and bacteria. That trap zone can lead to repeated inflammation episodes that feel like soreness, swelling, or tenderness at the back of the mouth. Many patients describe a cycle where the area improves briefly, then flares again, which is a common sign the tooth position is creating a predictable hygiene problem.
Swollen, Tender Gum Tissue Behind the Second Molar
Inflammation often concentrates behind the last fully erupted molar, especially when brushing irritates the area or when chewing presses on swollen tissue. The gum can feel puffy and sensitive, and the discomfort may increase when the immune system is stressed or sleep is disrupted. Patients often benefit from learning that this pattern is not just “gum sensitivity,” it can reflect repeated irritation linked to partial eruption.
Bad Taste or Persistent Odor That Returns After Cleaning
A trapped area can produce a recurring bad taste or odor even when you brush carefully. This often happens because bacteria remain below the gumline flap where normal cleaning does not reach consistently. Patients appreciate clear guidance because these signs can feel embarrassing and confusing when they keep returning.
Wisdom tooth pressure can create deep aching that feels like a dull, persistent soreness near the jaw angle. The discomfort may worsen during chewing or when the area remains inflamed for several days. Patients often describe this pressure as different from regular tooth sensitivity because it feels broader and harder to pinpoint.
Pain That Radiates Toward the Ear or Into the Jaw Joint Area
The back of the mouth shares nerve pathways that can make wisdom tooth pain feel like ear discomfort or jaw joint irritation. This referred pain can lead patients to suspect sinus issues or TMJ problems before realizing the third molar is involved. A focused dental evaluation helps clarify whether the wisdom tooth position is driving the symptoms.
Headache-Like Discomfort Triggered by Back-Molar Inflammation
Inflammation near the wisdom tooth can contribute to tension that feels like a headache concentrated near the temple or behind the ear. This pattern often accompanies jaw soreness and bite sensitivity in the back of the mouth. Patients tend to feel relieved when the cause is identified because it turns a vague discomfort pattern into a solvable problem.
When inflammation escalates around an impacted or partially erupted wisdom tooth, the jaw muscles can become reactive. Patients may notice stiffness when opening wide, discomfort when chewing, or a feeling that the back of the mouth is too tender to use normally. This sign matters because functional limitation suggests the inflammation has moved beyond a minor irritation.
Jaw Stiffness That Appears During Repeated Infection Episodes
Stiffness can develop when the tissues around the wisdom tooth remain inflamed and the jaw muscles tighten protectively. The limitation often improves after the flare calms down, then returns with the next episode. Patients benefit from understanding that recurring stiffness often signals a repeating infection pattern rather than a one-time irritation.
Why Functional Limitation Often Signals Escalation Risk
When chewing and opening become difficult, the problem tends to require more than home care adjustments. Functional limitation can indicate more significant swelling or deeper irritation that may worsen if left untreated. Patients often value this explanation because it clarifies why repeated flare-ups justify extraction planning.
Impacted wisdom teeth can press against the neighboring second molar, creating hard-to-clean contact points and increasing the chance of decay or gum problems between the teeth. This risk often develops quietly because the area is difficult to see and clean. Patients appreciate learning that extraction is sometimes recommended to protect the healthy tooth in front of the wisdom tooth.
Cavities and Gum Breakdown Between the Wisdom Tooth and Second Molar
Food and plaque can accumulate where the wisdom tooth contacts the second molar, especially when the wisdom tooth sits at an angle. That trap zone can lead to cavities on the back of the second molar or chronic gum irritation in the space between the teeth. Patients often do not notice these problems until imaging or an exam reveals early damage.
Why Protecting the Second Molar Often Drives the Extraction Decision
The second molar plays a critical role in chewing and long-term bite function, so preserving it matters. When a wisdom tooth threatens the second molar through pressure, decay risk, or gum breakdown, extraction becomes a preventive stability decision. Patients often feel more satisfied when the plan focuses on protecting a healthy tooth rather than waiting for damage.
A wisdom tooth region that repeatedly swells, drains, or becomes tender can signal an infection pattern that will likely recur. Patients may notice pus-like drainage, a gum bump, or swelling that comes and goes. Clear identification of these signs helps patients seek care sooner rather than waiting for the next escalation.
Swelling Episodes That Return After Temporary Improvement
Wisdom tooth infections often calm down briefly, then flare again because the underlying trap zone remains. This pattern can create a cycle of antibiotics or home care measures without long-term resolution. Patients tend to trust the recommendation more when they understand why temporary improvement does not mean the issue is solved.
Fever or Feeling Run-Down Along With Back-Molar Swelling
When back-molar inflammation coincides with fever or feeling unusually tired, the body may be reacting to a higher infection load. These systemic signs deserve prompt evaluation because they can indicate a more significant infection pattern. Patients benefit from clear guidance because it helps them separate routine discomfort from higher-risk warning signs.
How Wisdom Tooth Extraction Protects Crowding, Gum Health, and Bite Stability
Wisdom tooth extraction protects long-term oral stability by removing a predictable source of pressure, inflammation, and hard-to-clean anatomy at the back of the mouth. Even when symptoms feel mild, third molars can create conditions that undermine gum health and make bite function less reliable over time. Patients often feel more confident in the decision when the benefits are framed as protection of what you already have, including the second molars, the surrounding gums, and a bite that stays comfortable and balanced. PHD Dental emphasizes these long-view outcomes so the procedure feels like a preventive stability move rather than a reactive response to the latest flare-up.
Third molars often erupt into limited space, and that crowding pressure can push on adjacent teeth or create a feeling of tightness in the back of the arch. While every mouth responds differently, impacted or partially erupted wisdom teeth can still add force and contact that complicates long-term alignment stability. Removing the wisdom teeth can reduce that back-of-arch pressure and help preserve the space relationships that support a more stable bite.
How Limited Space Creates Ongoing Force Against Adjacent Molars
When a wisdom tooth pushes into the second molar, the contact can create chronic pressure and make the area harder to keep stable. That pressure can also trap plaque and increase the risk of gum irritation between the teeth. Patients appreciate understanding that extraction can remove a constant mechanical stressor rather than waiting for the second molar to become compromised.
Why Crowding Protection Often Matters Most After Orthodontic Treatment
Patients who have invested in orthodontics often want to protect their alignment results long term. Wisdom teeth that erupt into limited space can create new pressure and increase the risk of shifting, especially if the third molars remain partially trapped. A preventive extraction plan can support stability by removing an unpredictable force source at the back of the arch.
The far back of the mouth is difficult to clean consistently, even for patients with excellent hygiene habits. Wisdom teeth that sit partially erupted or angled can create pockets and food traps that repeatedly inflame the surrounding gum tissue. Extraction can reduce these trap zones so patients can maintain healthier gums without recurring tenderness, swelling, or bleeding in the back-molar area.
Lowering the Risk of Recurrent Pericoronitis and Tissue Irritation
Pericoronitis refers to inflammation of the gum tissue around a partially erupted wisdom tooth. The condition often recurs because bacteria and debris keep collecting under the gum flap, which makes true stability difficult. Patients often value extraction because it removes the anatomy that keeps triggering repeated inflammation cycles.
How Healthier Back-Molar Access Supports More Consistent Daily Hygiene
After removal, patients can often clean the back of the arch more thoroughly because the trap zone is gone. Improved access supports gum stability around the second molars, which helps protect long-term comfort and reduces future periodontal maintenance burdens. This benefit tends to feel practical because it improves day-to-day manageability rather than relying on perfect technique in a difficult area.
Second molars are essential for chewing and long-term bite function, and wisdom teeth can threaten them quietly. Impacted wisdom teeth can create contact points where plaque accumulates and cavities develop on the back surface of the second molar. Extraction protects the second molars by removing the adjacent risk factor that makes decay and gum breakdown more likely.
Preventing Cavities Between Teeth That Are Difficult to Detect Early
Decay between the second molar and an impacted wisdom tooth can develop without obvious symptoms. The location is hard to see and can be missed until the cavity becomes larger and more costly to treat. Patients often feel reassured when the plan focuses on protecting the healthy tooth in front, since that tooth does most of the daily chewing work.
Why Saving the Second Molar Often Drives the Long-Term Recommendation
When a wisdom tooth threatens the second molar, waiting can allow damage that requires fillings, crowns, or more complex treatment later. Patients tend to feel more satisfied when extraction is framed as preventing a bigger problem rather than reacting after damage occurs. This protection-first logic supports trust because it connects the recommendation to preserving function.
Recurring wisdom tooth irritation can lead patients to chew on one side or avoid certain foods to protect the painful area. Over time, this guarded pattern can strain the jaw and create uneven bite habits. Removing the wisdom teeth can reduce the flare-ups that drive avoidance so patients can chew more evenly and maintain a more stable bite pattern.
Reducing One-Sided Chewing Patterns That Develop During Wisdom Tooth Flare-Ups
When the back molars hurt, patients often avoid chewing on that side, which shifts work to the other side of the mouth. This uneven pattern can create fatigue and discomfort, and it can make the bite feel less balanced over time. Extraction helps by removing the recurring trigger that forces patients into long-term guarding.
How PHD Dental Connects Wisdom Tooth Removal to Long-Term Functional Comfort
Patients often want to know how extraction helps beyond “getting rid of a problem tooth.” PHD Dental explains the functional goal, which is a back-of-arch environment that stays calm, cleanable, and stable under normal chewing forces. This framing supports patient confidence because it ties the procedure to everyday comfort and long-term reliability.
Recovery Priorities, Risks, and How to Avoid Dry Socket After Extraction
Wisdom tooth recovery goes more smoothly when patients focus on a few high-impact priorities in the first several days, including clot protection, swelling control, and keeping the area clean without disturbing healing. The most common setbacks happen when the extraction site gets disrupted early, which can increase pain and slow stabilization. Patients tend to feel more confident when they understand which actions matter most and why, because it turns recovery into a practical plan rather than a list of vague restrictions. PHD Dental emphasizes risk prevention steps that protect healing and reduce the likelihood of dry socket, infection flare-ups, and prolonged discomfort.
A stable blood clot acts as the protective seal over the extraction site and supports early tissue repair. When the clot dislodges, the site can become exposed and painful, which is the common pathway to dry socket. Patients benefit from understanding that most early recovery rules exist to protect this clot so healing can progress steadily.
Avoiding Suction, Spitting, and Forceful Rinsing in the Early Window
Suction and forceful mouth movements can pull the clot out before the site has sealed. Many patients disrupt healing unintentionally by using straws, spitting repeatedly, or rinsing aggressively on the first day. Protecting the clot requires gentle habits, especially during the first 24 to 48 hours when stability is still forming.
Why Smoking and Nicotine Products Increase Dry Socket Risk
Nicotine can impair healing and increase the likelihood that the clot will break down or fail to stabilize. Smoking also adds suction forces and heat that can irritate the site. Patients often appreciate direct guidance here because avoiding nicotine is one of the most reliable ways to reduce dry socket risk.
Some swelling is normal after wisdom tooth removal, especially when the tooth was impacted or required more tissue manipulation. The goal is to reduce inflammation early so discomfort does not spike and the jaw stays functional. Patients tend to recover more predictably when they follow a consistent plan rather than reacting only after pain escalates.
Cold Therapy Timing and Jaw Rest to Reduce Early Inflammation
Cold therapy can help limit fluid buildup in the tissues during the early recovery window. Resting the jaw and avoiding excessive talking or chewing can also reduce irritation and help swelling settle sooner. Patients benefit when they understand that early swelling control is most effective in the first day, not after inflammation is already established.
Recognizing Normal Soreness Versus Pain That Signals a Complication
Normal soreness usually improves gradually and feels manageable with basic pain control. Complication-related pain often worsens, becomes sharp, or returns strongly after a brief improvement period. Knowing this difference helps patients contact the practice at the right time instead of guessing whether the pain is normal.
Food texture and temperature can affect healing because chewing force and debris can irritate the sockets. The priority is to keep nutrition steady while avoiding actions that disturb the clot or inflame the tissue edges. Patients often do best when they follow simple texture rules and progress back to normal foods gradually.
Soft Foods That Reduce Trauma and Debris Trapping
Soft foods reduce chewing pressure and lower the chance of scraping the healing area. Crunchy foods can lodge particles in the sockets and increase irritation. Patients appreciate clear guidance because food mistakes are a common cause of unnecessary soreness early on.
Why Heat and Spicy Foods Can Increase Throbbing in Early Healing
Heat can increase blood flow and swelling, and spicy foods can irritate healing tissue. Many patients notice increased throbbing after hot meals or heavily seasoned foods during the first days. Avoiding these triggers helps the site settle and reduces the chance of pain spikes.
Keeping the mouth clean matters after extraction, but aggressive cleaning can do more harm than good. The goal is to control bacterial load and prevent debris buildup while protecting the sockets. Patients feel more comfortable when hygiene instructions are clear and specific, since uncertainty often leads to either overcleaning or avoiding cleaning entirely.
Gentle Brushing and Controlled Rinsing That Supports Healing
Patients can continue brushing other teeth while keeping direct brushing away from the extraction sites early on. Controlled rinsing at the appropriate time helps reduce debris without dislodging the clot. This balance supports trust because it shows the plan protects healing while still managing infection risk.
When to Resume More Normal Cleaning Without Increasing Dry Socket Risk
Timing matters because returning to normal habits too soon can disturb the sockets. Patients benefit from a clear schedule for increasing cleaning intensity and reintroducing normal routines. This structure reduces anxiety because patients do not have to guess what is safe.
Most patients heal without major issues, but it is important to know the warning signs that require follow-up. Dry socket, infection signs, and unusual swelling patterns can develop after the initial improvement period. PHD Dental encourages patients to contact the office promptly if symptoms trend in the wrong direction rather than waiting for problems to intensify.
Signs of Dry Socket, Infection Return, or Uncontrolled Swelling
Dry socket often presents as worsening pain a few days after extraction, sometimes paired with a bad taste or odor. Infection concerns can include increasing swelling, fever, drainage, or pain that does not respond to normal measures. Knowing these signs helps patients act early and protect recovery.
How PHD Dental Supports Patients Through Recovery Checkpoints
Patients benefit from knowing what milestones should improve and when follow-up is recommended. Clear checkpoints reinforce trust because they show the practice remains accountable after the procedure. This approach also improves satisfaction because patients feel supported during the recovery window, not left to manage uncertainty alone.
Contact PHD Dental for an Evaluation of Your Impacted Wisdom Teeth

If you suspect you have impacted third molars, an evaluation for Wisdom Tooth Extractions in Los Angeles should clarify what your wisdom teeth are doing now and what they are likely to do next. Impacted teeth can threaten the second molars through pressure, hidden decay risk, or repeated gum inflammation in a space that is difficult to clean reliably. PHD Dental focuses on determining whether your symptoms match a predictable flare-up pattern and whether the tooth position creates a long-term stability problem for your bite and gum health. You should leave the visit understanding which teeth are involved, what the risk looks like if you wait, and what the safest removal plan would be for your specific anatomy.
Patients also benefit from an evaluation because it turns uncertainty into a clear decision path instead of waiting for the next episode of back-molar pain or swelling. If extraction is recommended, the plan should outline what makes removal necessary, how complexity affects approach, and what recovery priorities will protect healing afterward. If monitoring is appropriate, you should still receive guidance on what changes would trigger a stronger recommendation to remove the tooth later. This level of clarity builds trust because it avoids both rushed removal and delayed treatment that allows avoidable damage. The goal is to protect your second molars and long-term bite stability by addressing impacted wisdom teeth before they create harder problems.
Call (323) 269-5437 to schedule an evaluation with PHD Dental for impacted wisdom teeth and get a clear plan for wisdom tooth extractions in Los Angeles.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
