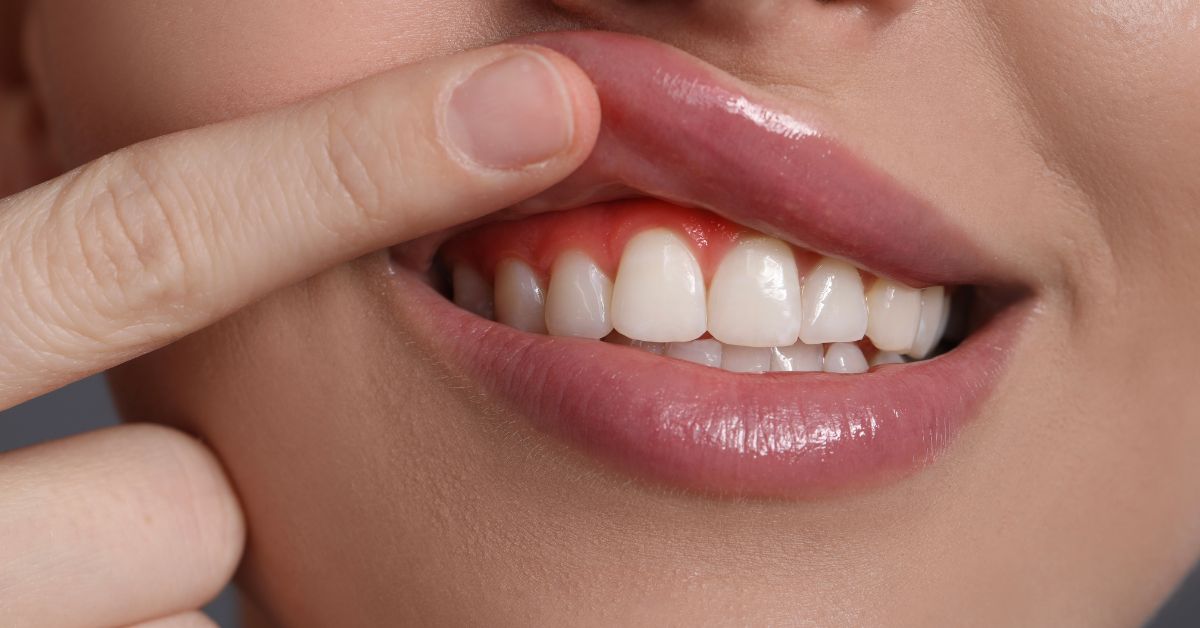
Gum Grafting for Recession in Los Angeles
Gum recession often starts quietly, but once the root stays exposed, your tooth faces higher sensitivity risk and greater long-term instability. Gum Grafting for recession in Los Angeles helps stabilize teeth when gum tissue has pulled back far enough to expose vulnerable root surfaces. and weaken the support that keeps teeth comfortable under normal bite pressure. The goal of grafting is not to “pretty up” the gumline. It is to rebuild coverage and improve tissue resilience where the tooth needs protection most. This treatment becomes especially important when recession continues to progress, when brushing triggers sharp sensitivity, or when the gumline no longer shields the root from daily wear.
At PHD Dental, we approach gum grafting with a function-first mindset. This focuses on protecting the tooth and reducing the conditions that make recession worsen over time. That means we pay attention to tissue thickness, root exposure patterns, and the mechanical forces that keep irritating the area so the graft supports a more stable baseline. We also set expectations around what grafting can change, including improved root coverage, better tolerance to temperature shifts, and less ongoing irritation at the gumline. Patients tend to feel more confident when the treatment plan explains why grafting makes sense now, and what risks often increase when recession continues untreated. The outcome we aim for is straightforward, stronger protection where the tooth has lost it, and a healthier tissue environment that helps the area hold up long term.
Call (323) 269-5437 to schedule a consultation with PHD Dental for gum grafting. Get a clear plan to protect exposed roots, reduce sensitivity, and stabilize your gumline.
Top-Rated Dentists
in Los Angeles
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Common Causes of Gum Recession That Need Grafting Surgery

Gum recession does not come from a single cause. The reason matters because it affects whether grafting becomes the most protective option. Some recession stays shallow and stable with targeted habit changes, while other patterns keep advancing even after you improve home care. PHD Dental focuses on identifying the driver that keeps the tissue retreating, then recommending grafting when the exposed root and thin tissue create an ongoing vulnerability you cannot solve with brushing changes alone. This approach prevents a one-size plan that treats every recession case the same, even when the underlying stresses differ. It also clarifies whether the main issue is repeated friction at the gumline, tissue thickness that offers limited protection, or inflammation that keeps weakening attachment. When the cause stays clear, patients can understand what grafting is meant to fix, and what needs to change so results hold. That level of specificity builds confidence because the recommendation connects to a real mechanism, not a generic warning about recession.
Many patients with recession keep their teeth very clean, but they use too much pressure or a stiff brush that scrapes the gum margin day after day. That repeated friction can thin the tissue until it pulls back and stops shielding the root surface. When the gumline remains fragile or continues receding despite better technique, grafting can add thickness and resilience where the tissue keeps losing the fight.
Overbrushing Patterns That Create V-Shaped Gum Recession and Root Notches
A common pattern shows up as a narrow, sharply defined area of gingival recession around one tooth or a small cluster of teeth. The root may also develop a worn notch that traps plaque and makes the area harder to keep comfortable. PHD Dental evaluates this shape carefully because a notch can keep irritating the gumline, which makes long-term stability harder without added tissue coverage.
Why Stabilizing the Gum Tissue Matters Even After You Switch to a Soft Brush
Changing your brush and technique often slows the damage, but it cannot rebuild tissue that has already thinned or pulled away. Exposed root surfaces stay more reactive to temperature and touch, which can keep the tooth feeling “on edge” during normal routines. A graft can provide a more durable margin that tolerates daily cleaning without flaring sensitivity as easily.
Inflammation around the gumline can weaken the attachment that helps tissue stay in place. When plaque and bacteria persist below the margin, the gum can detach and retreat as the supporting structures lose stability. PHD Dental looks at whether the recession reflects active inflammation, past periodontal breakdown, or both, because grafting works best when the underlying inflammatory driver is controlled.
Gum Recession That Flares, Calms Down, and Returns in the Same Area
Some patients notice a cycle where the gum feels irritated, then settles, then becomes inflamed again around the same tooth. That pattern often signals a local trap, an edge issue on a restoration, or a hygiene challenge created by the tooth shape. When recurring irritation keeps the tissue unstable, grafting may become part of a broader plan to rebuild a healthier, more maintainable margin.
Why “No Pain” Does Not Always Mean Your Gums are Low Risk
Recession can progress without obvious pain, especially when sensitivity has not kicked in yet. Patients often assume stability because the area feels quiet, even though the gumline continues to thin and the root remains exposed. PHD Dental emphasizes objective stability signs so decisions do not rely only on symptoms that may show up late.
Some people naturally have thinner gum tissue, and thin tissue has less tolerance for friction, inflammation, and minor trauma. When the tissue starts thin, even small triggers can lead to visible recession sooner than expected. PHD Dental evaluates tissue thickness and attachment quality because grafting can be a proactive way to strengthen a high-risk gumline before the recession becomes harder to control.
Gingival Recession Around Prominent Roots and Teeth Positioned Outside the Bone
A tooth that sits slightly forward or outside the bone housing can push the gum to a thinner edge, especially in the lower front teeth and canine areas. That anatomy can make recession more likely even when brushing habits are reasonable. When positioning and bone support limit natural protection, grafting can help create a stronger tissue barrier over the exposed root.
How PHD Dental Approaches Gum-related “Tissue Thickness”
Patients usually want to know what thickness changes in real life, not just as a clinical observation. Thicker tissue generally resists irritation better, stays more comfortable during cleaning, and holds coverage more reliably when forces act on the area. A graft can shift the baseline so the gumline has more “buffer” against the stresses that caused retreat in the first place.
Orthodontic treatment can improve alignment and function, but certain movements can place a tooth in a position where the gumline becomes more vulnerable. Heavy bite forces, clenching, or uneven contacts can also keep a thin gum margin under constant stress. PHD Dental accounts for tooth position and functional load because grafting works best when it supports a stable tooth environment, not a tooth that keeps taking repeated mechanical strain.
Clenching, Grinding, and High Contacts That May Cause the Need for Gum Grafting
Patients with grinding habits may notice recession paired with persistent sensitivity or a feeling that one tooth takes more pressure than the rest. Excess force can aggravate the gumline and contribute to micro-trauma that prevents the tissue from staying calm. When load issues show up, PHD Dental factors them into the graft plan so the result stays protected during everyday chewing.
When Correcting Force Patterns Helps the Graft Hold Its Gains
A graft can improve coverage and thickness, but the surrounding conditions still matter after surgery. Bite adjustments and habit-related guidance can reduce the repetitive stress that made the tissue vulnerable. Patients tend to feel more satisfied when the plan addresses both the graft and the mechanical factors that could otherwise shorten the benefit.
What to Expect During Los Angeles Gum Graft Surgery
Gum graft surgery follows a controlled clinical sequence that aims to rebuild protective tissue where recession has left a tooth exposed and vulnerable. The visit should feel organized and predictable, with clear checkpoints that confirm the graft site, tissue plan, and how the area will be protected once the procedure ends. At PHD Dental, we focus on practical clarity so you understand what the surgeon is trying to achieve at each stage and what “success” looks like when the graft heals and integrates.
A well-run gum graft appointment starts with confirming which teeth need coverage and how much tissue support each site requires. The plan also addresses whether one area needs priority because the recession pattern creates a higher risk of ongoing exposure. Patients tend to feel more confident when the plan explains what the graft will change and what the clinical team will monitor during healing to confirm the tissue is stabilizing as expected.
Mapping the Gum Graft Area and Setting Clear Expectations for Coverage
Gum grafting is not always about chasing maximum coverage, and a trustworthy recommendation explains the realistic target for your anatomy. The team defines where the tissue needs reinforcement and which edges must remain stable for the result to hold up over time. This clarity reduces uncertainty because you are not left guessing whether the goal is appearance, comfort, or structural protection.
How PHD Dental Clarifies the Difference Between Root Coverage and Tissue Thickening
Some cases prioritize increased tissue thickness over complete root coverage, especially when the recession pattern makes full coverage less predictable. Thicker tissue can still improve protection and reduce irritation even if the root remains partially visible. Patients appreciate this explanation because it connects the outcome to stability and comfort rather than a cosmetic promise.
Gum grafting can use your own tissue or a graft material selected for predictable integration, depending on the clinical situation. The best choice balances coverage goals, healing demands, and the number of sites being treated. PHD Dental explains these options in straightforward terms so you understand what the material choice means for healing experience and long-term tissue strength.
Using Your Own Tissue Versus Processed Graft Material in Gum Graft Surgery
Autogenous grafts use tissue from your mouth, often from the palate, which can provide strong integration and reliable thickening for certain recession patterns. In other cases, processed graft material can reduce donor-site discomfort and still provide meaningful reinforcement. Patients trust the plan more when the dentist explains why one option fits the recession pattern better instead of presenting it as a default.
What Material Choice Means for Healing Sensations and Follow-Up Care
Different graft sources can influence where you feel soreness and how you manage early healing. A clear plan explains which area will need the most protection, what foods to avoid, and how the practice will check the site during follow-up. That guidance improves satisfaction because patients feel prepared for what the first few days will realistically involve.
Patients usually feel calmer when the appointment has a defined rhythm and the team explains transitions clearly. Gum graft surgery includes anesthetic planning, site preparation, graft placement, and stabilization measures that protect the tissue during early healing. The goal is to create a secure environment for the graft to attach and mature without unnecessary disruption.
Site Preparation and Tissue Conditioning Before Graft Placement
The surgeon prepares the recipient area so the graft has a stable foundation and the tissue edges can support healing. That preparation may involve cleaning the exposed root surface and shaping the site so the graft sits flush and protected. Patients benefit from this precision because graft success depends on stability at the margins, not only on the graft itself.
Stabilization Methods That Help the Graft Stay Protected During Early Healing
A gum graft needs to remain stable so blood supply and tissue integration can develop as intended. The surgeon uses techniques to secure the graft and reduce movement that could interfere with attachment. When patients understand that stability drives success, they tend to follow post-procedure restrictions more consistently, which protects the result.
Early guidance should feel specific and easy to follow, especially during the first days when the graft site remains delicate. Patients receive instructions about eating, cleaning, and how to avoid accidental trauma that can compromise the graft. PHD Dental emphasizes practical guardrails that reduce guesswork so you can protect healing without feeling overly restricted.
Eating, Brushing, and Activity Guidelines That Reduce Gum Graft Disruption Risk
Most setbacks happen when the graft area gets bumped, stretched, or irritated during routine habits. Patients typically need temporary adjustments in chewing and brushing technique to avoid disturbing the site. Clear instructions improve trust because they prevent vague rules that leave patients unsure what is safe.
Follow-Up Timing That Confirms Healing Progress Without Unnecessary Visits
A reliable plan includes follow-up checkpoints that match the risk level of the graft site and the number of areas treated. The practice confirms that the tissue looks stable, healing is trending in the right direction, and the patient can slowly return to normal routines. Patients value this structure because it provides verification, not guesswork, about whether healing is on track.
Long-Term Benefits of Gum Grafting for Tooth Stability and Sensitivity Reduction

The long-term value of gum grafting comes from changing the environment around an exposed root so the tooth can tolerate everyday forces and hygiene without constant irritation. When recession leaves the root uncovered, the tooth often becomes more reactive to temperature shifts and more vulnerable to ongoing wear at the gumline. A successful graft improves structural protection and helps the area stay calmer over time, which many patients experience as both better stability when chewing and less sensitivity during normal brushing and eating.
Exposed root surfaces do not have the same protective outer layer as enamel, so they can wear down faster under routine contact and cleaning. Over time, that wear can deepen sensitivity and make the gumline harder to maintain comfortably. Gum grafting adds a protective tissue layer that helps shield the root and reduce the chance that the exposed area continues to deteriorate with everyday use.
Reducing Root Surface Abrasion That Can Worsen Gum Sensitivity Over Time
When the root stays exposed, brushing friction and normal oral habits can gradually roughen the surface. That roughness can increase reactivity and make plaque control more difficult because the area catches buildup more easily. Patients often value grafting because it helps stabilize the margin and reduces the cycle of irritation that makes the area feel persistently sensitive.
Why Root Protection Often Matters More Than Cosmetic Coverage in Dentistry
Some patients focus on how much of the root will be covered, but the more important outcome is whether the root becomes less vulnerable to ongoing breakdown. Even when full coverage is not the primary goal, added tissue can improve resilience and reduce ongoing stress at the gumline. PHD Dental explains this clearly so patients measure success by protection and comfort, not by an unrealistic visual endpoint.
Thin gum tissue tends to respond poorly to repeated friction, inflammation, or minor trauma, even after you improve home care. A graft can increase thickness so the gumline behaves more predictably and resists future retreat. That stability matters because it reduces the likelihood that the recession will continue advancing in the same area and exposing more root over time.
Creating a More Durable Gumline Margin That Tolerates Normal Cleaning
Many patients with recession feel trapped because thorough brushing irritates the gumline, but light brushing feels ineffective. A thicker, healthier tissue margin can tolerate careful cleaning with less discomfort, which makes daily hygiene easier to sustain. Better tolerance supports satisfaction because patients can maintain results without feeling like every brushing session risks making the recession worse.
How Stable Tissue Helps Reduce Recurring Irritation and Flare-Ups
Recession areas can become chronically inflamed if the tissue remains thin and easily traumatized. Thicker tissue often means fewer episodes of soreness or bleeding triggered by small changes in diet, brushing, or stress. Patients often notice that the area feels less reactive once the gumline gains a stronger baseline.
Tooth sensitivity related to recession usually comes from root exposure, not from a “weak tooth” in general. When the root remains uncovered, temperature changes and certain foods can trigger sharp discomfort. Gum grafting can reduce that exposure so the nerve-related response calms down and the tooth feels more normal during everyday eating and drinking.
Less Temperature Shock During Eating and Drinking After Gingival Grafting
Patients often describe a quick, sharp sensitivity when they drink cold water or breathe in cool air. As the root becomes better protected, those triggers typically become less intense and less frequent. This improvement increases confidence because patients stop anticipating discomfort during normal routines.
Why Sensitivity Improvements Often Build Gradually Instead of Overnight
Even after the graft heals, the tooth and surrounding tissues may need time to settle into a more stable baseline. Patients often see steady improvement as inflammation decreases and the area becomes less exposed and less reactive. PHD Dental sets expectations around this gradual change so progress feels measurable rather than unpredictable.
Grafting can play a meaningful role in keeping a tooth viable when recession patterns suggest continued retreat and repeated irritation. By improving tissue protection, the tooth is less likely to face ongoing root wear, chronic sensitivity, and gumline instability that can complicate future care. Patients appreciate this long-view benefit because it protects daily comfort now while also reducing the chance that the problem becomes more complex later.
Supporting Future Dental Work by Protecting the Gumline Foundation
A stable gumline makes it easier to maintain hygiene and reduces the risk that future dental work around the area becomes harder to manage. When the tissue remains fragile, even routine dentistry can feel more uncomfortable and more prone to irritation afterward. Stronger tissue support can make future care simpler and more predictable, which many patients value as part of long-term planning.
How PHD Dental Approaches Gum Grafting as a Preventive Stability Move
Patients often assume grafting only matters when the recession becomes severe, but earlier intervention can protect a tooth before the risk profile worsens. When the plan reflects structural vulnerability instead of waiting for escalating symptoms, outcomes often feel more stable and easier to maintain. This approach supports trust because it treats grafting as a strategic decision tied to long-term tooth preservation.
Schedule a Gingival Grafting Consultation in Los Angeles
When recession reaches the point where the root stays exposed and the gumline no longer feels stable day to day, timing starts to matter. A consultation for Gum Grafting for Recession in Los Angeles should clarify whether the area has crossed into a structural risk category, where waiting increases the chance of continued tissue loss, deepening sensitivity, or root surface wear that becomes harder to protect later. PHD Dental focuses on giving you a clear, defensible recommendation that matches your recession pattern and your long-term priorities, not a generic plan built around assumptions. You leave knowing what the graft is meant to accomplish for your specific tooth or teeth, what stability should look like after treatment, and what factors could limit predictability if the recession continues to progress.
Patients also benefit from a consultation because it turns uncertainty into a plan with decision points you can understand. If grafting makes sense, the visit should explain the practical tradeoffs, including what the treatment can realistically improve and what habits or force patterns still need attention so results hold. If grafting is not the right next step, you should still receive guidance that protects the area and defines what would change the recommendation later. That level of clarity builds trust because it respects your time and prevents you from cycling through temporary fixes while recession keeps advancing. The goal is straightforward, protect exposed roots, reduce instability, and support a gumline that feels easier to live with long term.
Call (323) 269-5437 to schedule a gingival grafting consultation at PHD Dental in Los Angeles and get a clear plan to protect exposed roots and stabilize recession-prone gum tissue.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
