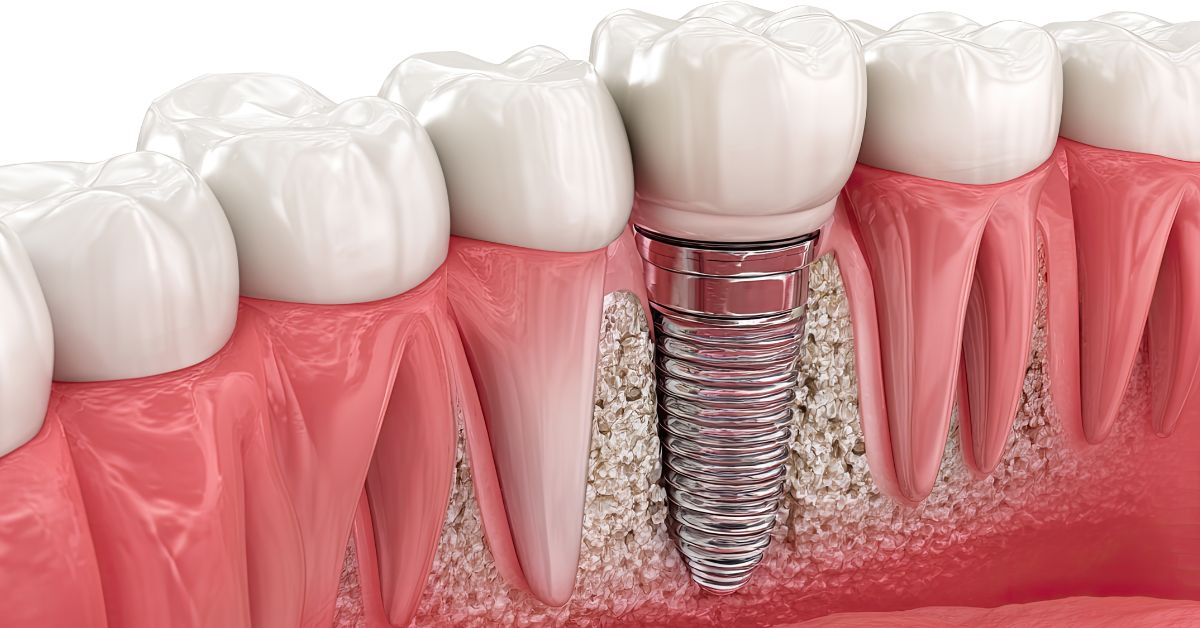
Endosteal Implants in Lynwood
Endosteal implants are selected when tooth replacement needs to be anchored within the jawbone itself rather than supported by removable structures. This approach relies on how bone responds to surgical placement, healing, and long-term functional load once a restoration is attached. Dentists consider if the jaw can provide consistent support over time and how implant placement may influence bite balance, adjacent teeth, and future dental planning.
Planning for endosteal implants in Lynwood requires looking beyond the surgical appointment and into how the implant will perform long-term under daily use. Dentists evaluate bone density patterns, implant positioning options, and how forces will be transferred through the implant. Healing, maintenance access, and adaptability for future care are reviewed before treatment is recommended. This planning process focuses on longevity and future maintenance over rapid replacement. Implant decisions are made with the full lifespan of the restoration in mind. If you are considering endosteal implants in Lynwood and want a clear explanation about if this is right for you, call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation focused on careful evaluation and realistic planning.
Top-Rated Dentists
in Los Angeles
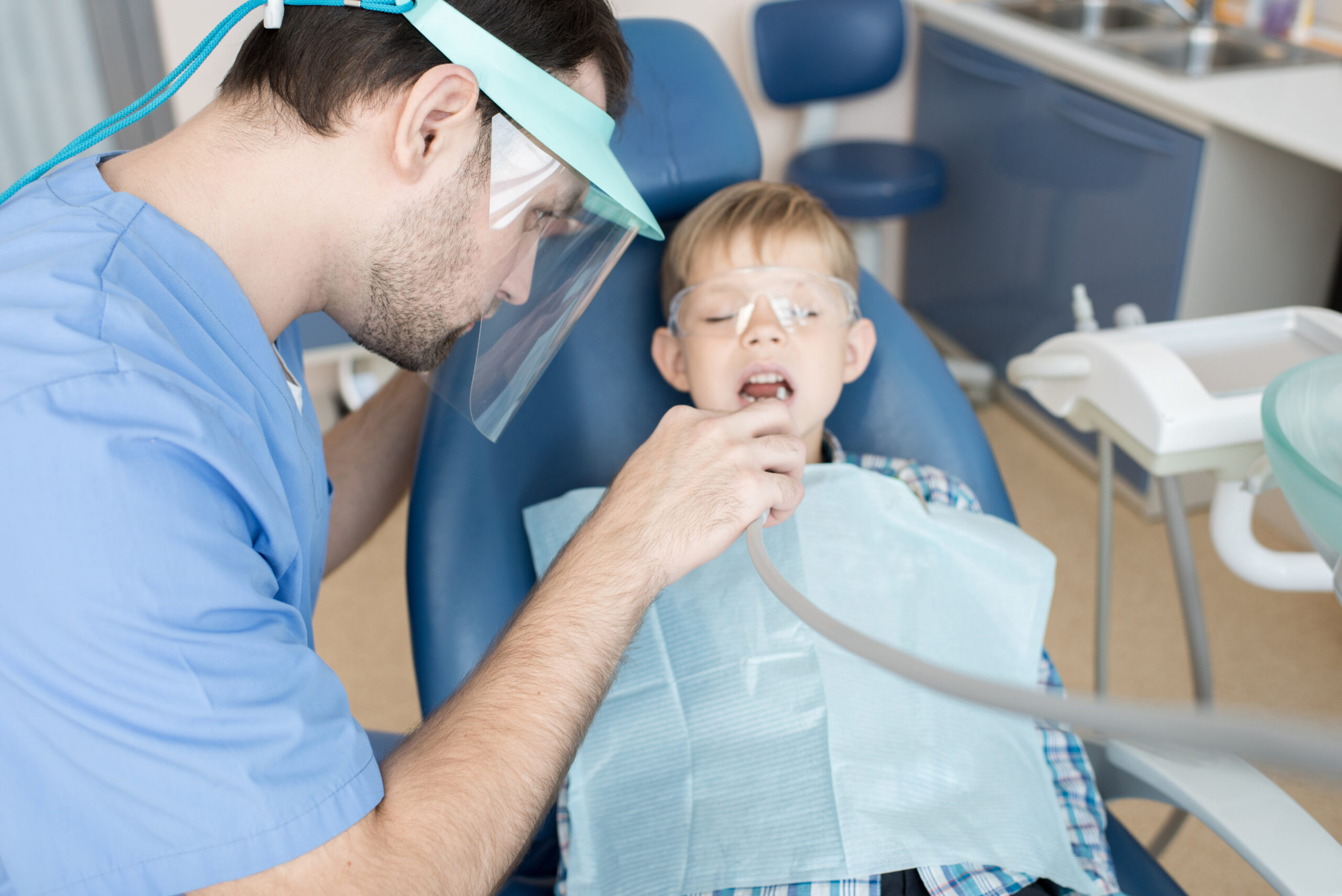
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
- How Endosteal Implants Change the Way Chewing Forces Travel Through the Jaw
- What Determines Whether Bone Can Support Endosteal Implants Long Term
- Why Endosteal Implants Are a Permanent Structural Decision
- How PhD Dental Evaluates Endosteal Implants Within a Lifetime Care Plan
- Call PhD Dental Today to Learn About Our Endosteal Implants in Lynwood
How Endosteal Implants Change the Way Chewing Forces Travel Through the Jaw
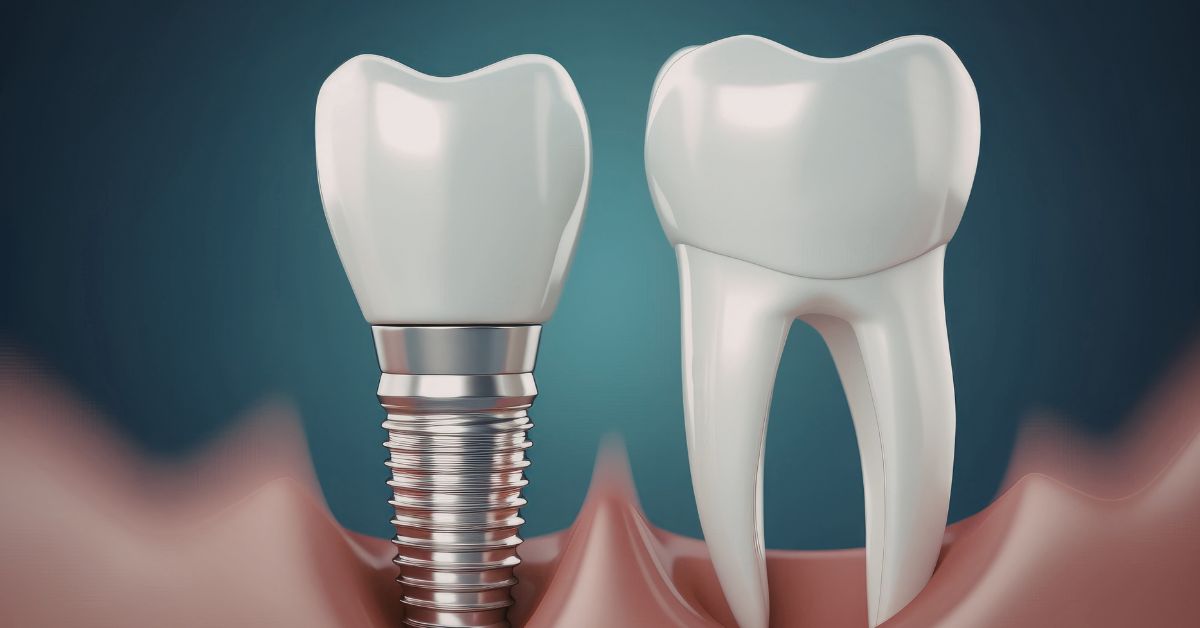
Endosteal implants alter how chewing forces are transferred through the jaw by anchoring restorations directly within bone rather than relying on surface contact or adjacent teeth for support. This structural change affects how pressure is absorbed, redirected, and distributed during everyday functions such as chewing, speaking, and clenching. With endosteal implants from PhD Dental in Lynwood, dentists consider not only whether bone can accept an implant, but also how force pathways will change once the implant becomes part of the jaw system. These changes influence comfort, durability, and how surrounding bone adapts over time. Understanding force movement helps explain why implant planning goes beyond simply replacing missing teeth.
Force transmission through the jaw becomes more localized and predictable when an implant integrates successfully with bone. Instead of load spreading across gum tissue or neighboring teeth, pressure travels through the implant into the surrounding jawbone. This shift can be beneficial when bone structure is adequate, but it also requires careful planning to avoid overload. Dentists evaluate how chewing forces will interact with bone density patterns and bite dynamics. The goal is to create a force pathway that the jaw can tolerate consistently over many years.
Natural teeth are supported by periodontal ligaments that allow slight movement and shock absorption during chewing. Endosteal implants lack this ligament and transfer force more directly into the jawbone. This difference changes how pressure is absorbed and how stress accumulates during function. Dentists account for this distinction when planning endosteal implants in Lynwood to avoid excessive force concentration. Comparing these force pathways helps guide placement and restoration decisions.
Why Direct Bone Loading Requires Careful Planning
Without a periodontal ligament, implants rely entirely on bone to absorb chewing pressure. Bone must be capable of handling repeated load without fatigue or breakdown. Dentists evaluate bone density and volume to confirm it can tolerate direct loading. Planning focuses on matching implant design to bone capacity.
How Bone Quality Influences Force Tolerance
Denser bone can absorb and distribute force more effectively over time. Areas of reduced density may concentrate stress if overloaded. Dentists identify these variations during planning. Bone quality shapes implant positioning decisions.
The location and angle of an endosteal implant determine how chewing forces move through the jaw. Poor positioning can direct force into weaker bone areas or create uneven stress patterns. Strategic placement allows forces to travel along stronger structural pathways. Dentists plan implant orientation to align with natural bite mechanics. Proper positioning supports balanced force transmission.
How Angulation Affects Load Direction
Angled implants can redirect force toward denser bone regions. This approach may reduce stress on vulnerable areas. Dentists use angulation to improve load sharing. Orientation influences long-term stability.
Why Misaligned Forces Create Long-Term Risk
When forces travel in unfavorable directions, bone may remodel unevenly. Concentrated stress can contribute to discomfort or structural changes. Dentists aim to prevent these patterns. Force alignment protects jaw health.
The design of the final restoration plays a major role in how force is applied to an implant. Bite contacts, material choice, and arch shape affect pressure distribution. Dentists design restorations to spread load evenly during chewing. Poor design can amplify stress even when implants are well placed. Restoration planning completes the force management strategy.
How Bite Contact Design Shapes Force Flow
Contact points determine where pressure is applied during function. Dentists adjust contacts to avoid excessive load on a single implant. Balanced contact supports even force distribution. Bite design is intentional.
Why Restoration Materials Matter for Load Absorption
Different materials transmit force differently into implants and bone. Dentists select materials based on durability and force characteristics. Material choice affects long-term performance. Selection supports predictable outcomes.
What Determines Whether Bone Can Support Endosteal Implants Long Term
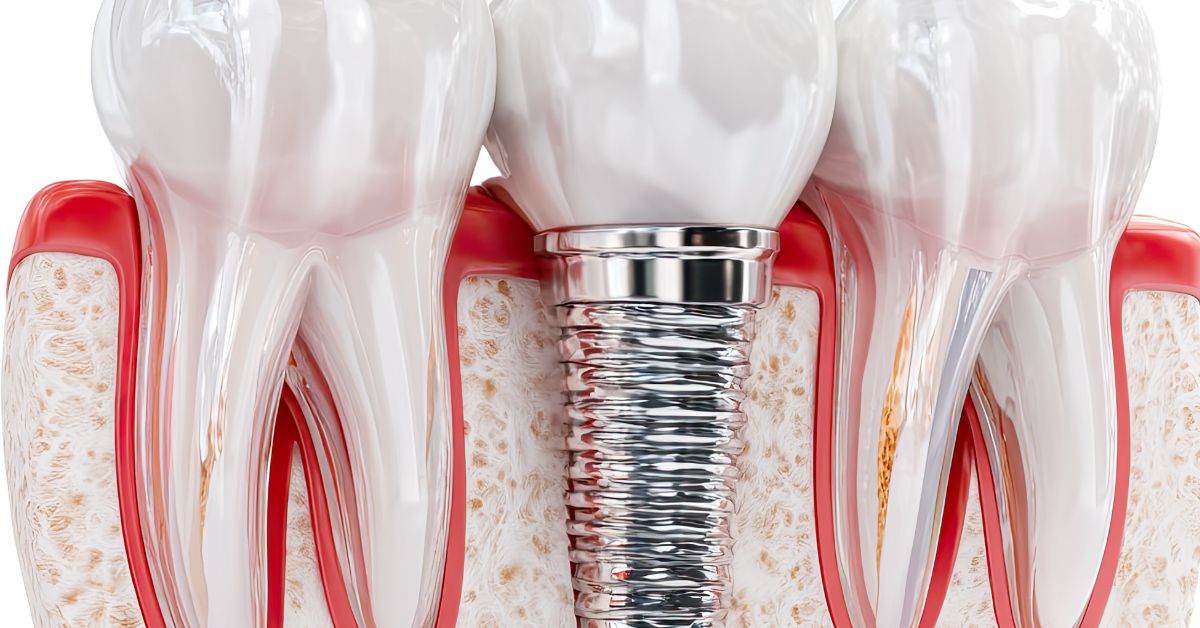
Long-term support for endosteal implants depends on how the jawbone responds to sustained functional load rather than how bone appears at a single point in time. Dentists evaluate whether bone can adapt, remodel, and maintain density around an implant as chewing forces are applied day after day. With endosteal implants in Lynwood, this assessment focuses on durability under repeated stress rather than initial surgical stability alone. Bone that supports implants successfully must tolerate ongoing pressure without progressive loss or structural fatigue. These considerations shape whether implants can remain stable years after placement.
Bone support is also influenced by how force is introduced, how evenly it is distributed, and how surrounding tissues remain healthy over time. Dentists look beyond surface density measurements to understand how bone quality varies throughout the jaw. Planning accounts for how bone will behave as part of a functional system rather than as an isolated structure. Endosteal implants in Lynwood are recommended when bone conditions support predictable long-term performance. Stability is evaluated as an ongoing biological process rather than a one-time threshold.
Bone density influences how well the jaw can absorb and distribute chewing forces transferred through an implant. Areas of dense, well-organized bone tend to tolerate load more consistently than regions with porous or uneven structure. Dentists assess whether density patterns are uniform enough to avoid localized stress concentration around the implant. Variations in density can affect how bone remodels over time. Structural consistency supports reliable long-term anchorage.
How Dentists Interpret Density Beyond Imaging Numbers
Imaging provides insight into relative density, but dentists also consider distribution and continuity of bone structure. Dense bone concentrated in small areas may still present risk if surrounding regions are weak. Evaluation focuses on how forces will spread through bone during function. Interpretation goes beyond numeric values.
Why Uneven Density Can Undermine Implant Stability
When dense and weak bone coexist, force may concentrate at transition zones. These stress points can accelerate bone remodeling in unfavorable ways. Over time, uneven adaptation may reduce support. Long-term success depends on balanced structural response.
Bone supporting an implant must continually adapt to mechanical forces through remodeling. This process allows bone to strengthen in response to appropriate load but can also lead to loss if forces exceed tolerance. Dentists evaluate whether bone shows signs of healthy turnover rather than fragility. Remodeling capacity influences how bone responds years after placement. Sustainable adaptation supports longevity.
How Dentists Assess Remodeling Potential Clinically
Clinical evaluation considers bone quality, medical history, and prior healing response. Imaging trends may reveal how bone has changed over time. Dentists look for indicators of active, healthy turnover. These factors guide long-term expectations.
Why Limited Remodeling Increases Long-Term Risk
Bone that cannot adapt effectively may resorb under repeated stress. This response can compromise implant stability gradually rather than abruptly. Limited remodeling reduces margin for error. Long-term planning accounts for this risk.
Bone support depends not only on how much force is applied, but also on how consistently and predictably it is delivered. Endosteal implants transmit force directly into bone, making direction and magnitude especially important. Dentists assess bite patterns to determine whether forces will remain within tolerable ranges. Irregular or excessive loading can strain bone adaptation. Consistent force pathways support stability.
How Bite Dynamics Affect Bone Stress Patterns
Chewing patterns determine where and how force enters the jaw. Dentists evaluate whether bite dynamics create lateral or concentrated stress. Adjustments may be planned to redirect force more favorably. Bite analysis informs support evaluation.
Why Variable Loading Can Accelerate Bone Fatigue
Inconsistent force application can challenge bone’s ability to adapt evenly. Sudden or uneven loads may exceed local tolerance. Over time, this can weaken support. Predictable loading favors durability.
Long-term bone support reflects overall skeletal health and the local healing environment around the implant. Factors such as circulation, metabolic health, and prior bone loss influence adaptation. Dentists consider whether bone conditions support sustained integration rather than short-term fixation. A healthy environment promotes stable support. Broader health context matters.
How Systemic Factors Influence Local Bone Support
Systemic conditions can affect bone density and healing response. Dentists review health history to understand these influences. Local bone behavior often reflects broader physiological patterns. Evaluation integrates systemic context.
Why Local Healing Depends on More Than Surgery
Surgical placement alone does not determine long-term outcome. Ongoing bone health shapes how support evolves. Favorable healing conditions must persist. Long-term stability depends on continued biological support.
Why Endosteal Implants Are a Permanent Structural Decision
Endosteal implants represent a long-term structural commitment because they are integrated directly into the jawbone and become part of how the mouth handles force, balance, and function over time. Once placed, these implants influence bone remodeling, bite mechanics, and future restorative options in ways that cannot be easily reversed or adjusted without additional surgery. With endosteal implants in Lynwood, dentists evaluate permanence as a defining characteristic rather than a secondary consideration. Decisions made at the planning stage shape how the jaw adapts for decades, not just during the initial healing phase. This permanence is central to understanding why implant treatment requires careful, forward-looking judgment.
The structural nature of endosteal implants also means that early choices establish constraints and opportunities for future care. Implant position, depth, and orientation determine what types of restorations are possible later and how easily maintenance or modification can be performed. Unlike removable or surface-supported solutions, implants do not allow for casual repositioning once bone integration occurs. Endosteal implants in Lynwood are therefore approached as foundational decisions that affect the entire oral system. Long-term thinking guides whether this level of permanence is appropriate.
When an endosteal implant integrates with bone, it alters how the jaw responds to functional stress and load over time. Bone remodels around the implant surface, reinforcing areas that receive consistent force while adapting away from regions that no longer experience pressure. This process effectively incorporates the implant into the skeletal structure of the jaw. Once integration is complete, removal or repositioning requires additional surgical intervention and bone modification. Structural change is therefore not temporary.
Why Osseointegration Limits Reversibility
Osseointegration creates a direct connection between bone and implant without an intervening ligament. This connection stabilizes the implant but also binds it to the surrounding bone architecture. Reversing this integration requires disrupting bone that has adapted to the implant’s presence. The process is inherently invasive.
How Long-Term Bone Adaptation Reinforces Permanence
Over time, bone density and structure adjust to accommodate repeated functional load through the implant. These adaptations strengthen the implant site but also make the configuration increasingly fixed. Bone that has been remodeled around an implant does not easily return to its prior state. Permanence increases as adaptation progresses.
The exact location and angulation of an endosteal implant determine how restorations can be designed and modified later. Placement affects access for hygiene, distribution of chewing forces, and compatibility with adjacent teeth or restorations. Poorly planned placement can restrict future corrective options or require complex revisions. Dentists treat placement decisions as long-term commitments rather than adjustable steps. Precision at this stage preserves flexibility.
Why Early Planning Errors Are Difficult to Correct
Once an implant is integrated, correcting misalignment often involves removing bone or placing additional implants. These interventions increase complexity and risk compared to initial placement. Early errors can cascade into long-term limitations. Careful planning reduces the likelihood of such outcomes.
How Strategic Placement Preserves Long-Term Adaptability
Thoughtful placement anticipates future restorative needs and potential changes in oral health. Allowing space for maintenance and modification protects long-term usability. Strategic decisions made early maintain options later. Adaptability depends on foresight.
Endosteal implants establish a consistent pathway through which chewing forces travel into the jawbone. Unlike natural teeth, which have some capacity for movement and shock absorption, implants transmit force directly into bone. This fixed load pathway influences how stress is distributed across the jaw over time. Once established, altering this pathway is difficult without surgical change. Load commitment is part of implant permanence.
How Fixed Load Transfer Affects Jaw Dynamics
Direct force transmission can strengthen bone when loads are appropriate and evenly distributed. However, unfavorable force patterns may concentrate stress in specific areas. Dentists evaluate whether the jaw can tolerate this fixed pathway long term. Load dynamics are central to planning.
Why Load Commitment Requires Conservative Decision Making
Since force pathways cannot be easily changed after placement, dentists avoid aggressive or marginal planning. Conservative decisions reduce the risk of overload or imbalance. Permanence demands restraint. Long-term stability depends on respecting these limits.
How PhD Dental Evaluates Endosteal Implants Within a Lifetime Care Plan
PhD Dental evaluates endosteal implants by considering how today’s implant decisions will interact with oral health needs years and decades into the future rather than focusing only on immediate restoration goals. Planning accounts for how bone structure may change with age, how bite forces may evolve, and how future dental treatments could be affected by permanent implant placement. Endosteal implants in Lynwood are assessed as long-term structural commitments that influence flexibility for later care. This evaluation framework emphasizes foresight, restraint, and durability rather than short-term problem solving. Implant decisions are positioned within the broader lifespan of oral health.
Endosteal implants influence which restorative or corrective options remain available later in life, especially as surrounding teeth, bone, and bite patterns change. PhD Dental evaluates whether implant placement may limit future orthodontic movement, restorative modifications, or surgical options. Planning examines how fixed implant positions interact with teeth that may shift or require treatment later. The goal is to avoid creating rigid constraints that complicate future care. Flexibility is treated as a clinical asset.
How Implant Positioning Can Restrict Later Modifications
Once integrated, implants cannot move with natural teeth or adapt to bite changes. Placement that does not anticipate future needs may block corrective options. Dentists assess spacing and orientation with long-term adaptability in mind. Early foresight reduces later limitations.
Why Preserving Future Options Influences Implant Decisions
Oral health evolves over time due to wear, aging, and health changes. Preserving flexibility allows treatment plans to adapt without invasive revisions. Dentists prioritize decisions that avoid locking the mouth into a single outcome. Lifetime planning values adaptability.
Bone density, jaw structure, and bite dynamics can shift gradually as part of natural aging. PhD Dental evaluates whether current bone conditions are likely to remain supportive under long-term functional demands. Planning considers how implants will behave as bone remodels or density changes occur. Bite forces may also redistribute over time, affecting load on implants. Anticipating these changes supports longevity.
How Aging Bone Influences Implant Performance Over Time
Bone may become denser or more fragile depending on health factors. These changes affect how force is absorbed around implants. Dentists evaluate whether bone can adapt safely long term. Aging patterns inform planning decisions.
Why Bite Evolution Matters for Long-Term Implant Success
Chewing patterns and bite balance often change gradually with tooth wear or dental treatment. Implants do not adapt naturally to these shifts. Planning accounts for potential bite evolution to avoid overload. Long-term success depends on anticipating change.
Endosteal implants require ongoing professional monitoring and daily hygiene access to remain healthy over time. PhD Dental evaluates whether patients can realistically maintain implants as part of lifelong oral care. Planning includes consideration of access for cleaning, restoration servicing, and follow-up care. Implant placement that complicates maintenance can increase long-term risk. Lifetime care planning includes maintenance feasibility.
How Maintenance Access Shapes Placement Strategy
Implants placed without regard for hygiene access can trap plaque and bacteria. Dentists plan spacing and restoration contours to allow effective cleaning. Maintenance access supports tissue health. Placement strategy reflects this priority.
Why Long-Term Care Demands Influence Treatment Approval
Even well-placed implants can fail without proper ongoing care. Dentists evaluate whether maintenance demands align with patient capacity. Treatment approval considers long-term responsibility. Lifetime planning includes realistic care expectations.
Call PhD Dental Today to Learn About Our Endosteal Implants in Lynwood
Choosing endosteal implants involves committing to a treatment that will influence oral health decisions for many years, not just resolving a current concern. A consultation provides the opportunity to discuss how endosteal implants in Lynwood may affect future dental flexibility, bone behavior over time, and long-term maintenance responsibilities. PhD Dental uses this conversation to review how implant placement fits within a lifetime care plan.
During the consultation, dentists explain how aging, bite changes, and ongoing oral care affect permanent implant placement. The discussion covers what can realistically be expected over time and how future dental needs are considered before treatment begins. Patients leave with a clear understanding of why an implant may or may not be recommended within their oral health goals. Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation today.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
