
Wisdom Teeth Removal in Lynwood
Third molars can slowly create problems long before pain or swelling becomes obvious especially when space in the jaw is limited. Wisdom teeth removal in Lynwood is often discussed after dentists identify pressure against nearby teeth, gum tissue changes, or early signs of impaction during routine examination. These teeth develop later than others and frequently compete for space which can alter alignment. Evaluation focuses on how wisdom teeth are positioned within the jaw and how their continued presence may affect structure over time.
Decisions about wisdom teeth removal in Lynwood also depend on how roots are forming, how bone density may change over time, and how surgical access could become more complex if intervention is delayed. A measured assessment helps determine whether monitoring, early removal, or delayed intervention makes the most sense. If you are considering wisdom teeth removal in Lynwood and want a clear explanation of if removal is necessary, what factors influence timing, and how recovery is managed, call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation today.
Top-Rated Dentists
in Los Angeles
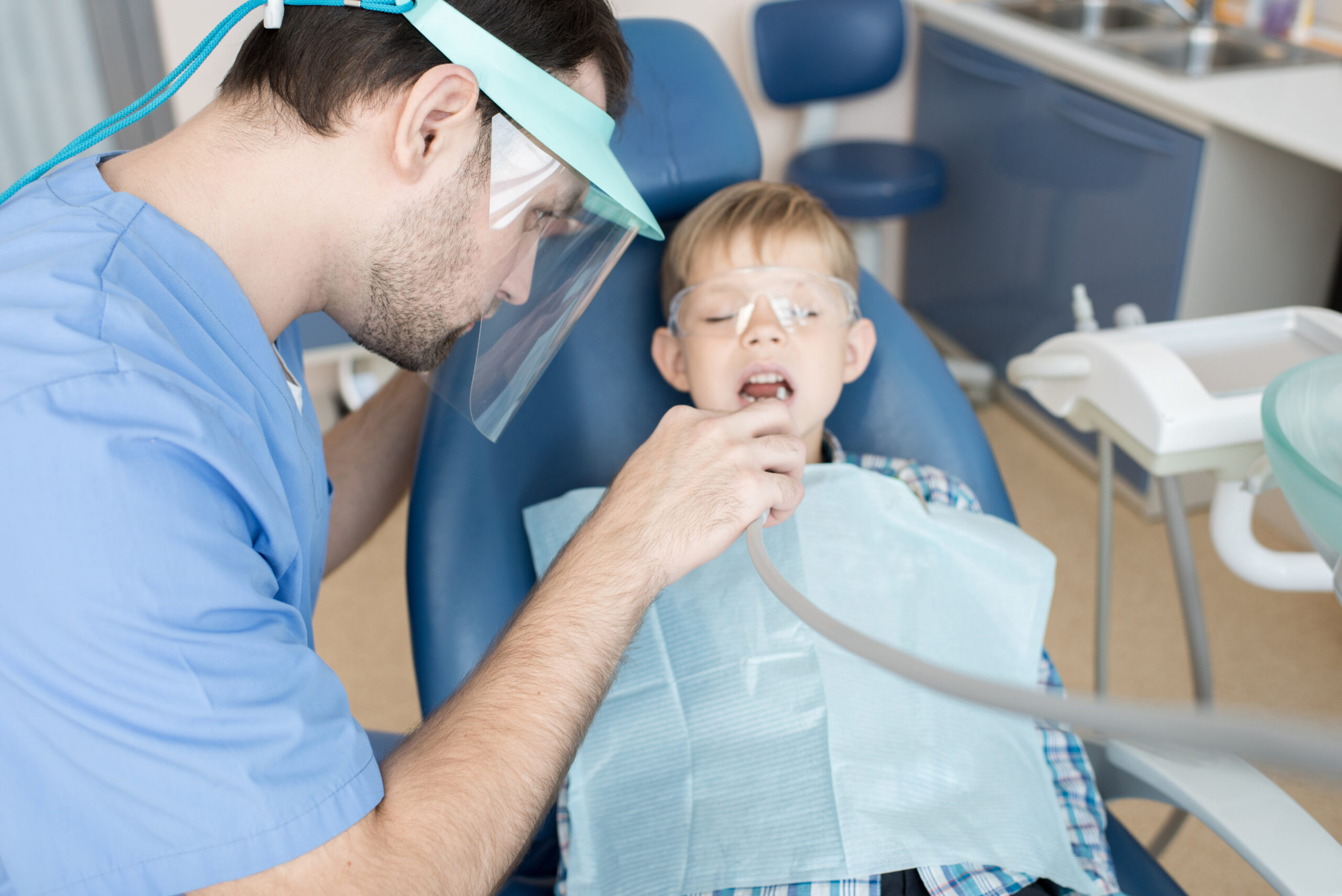
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
- What Structural Conditions Make Wisdom Teeth Removal Necessary
- Why Wisdom Teeth Removal in Lynwood Is Sometimes Recommended Before Symptoms Appear
- How Dentists Determine the Right Timing for Wisdom Teeth Removal in Lynwood
- How PhD Dental Determines When Wisdom Teeth Stop Being Low-Risk
- Contact PhD Dental to Learn About Our Wisdom Teeth Removal in Lynwood Today
What Structural Conditions Make Wisdom Teeth Removal Necessary
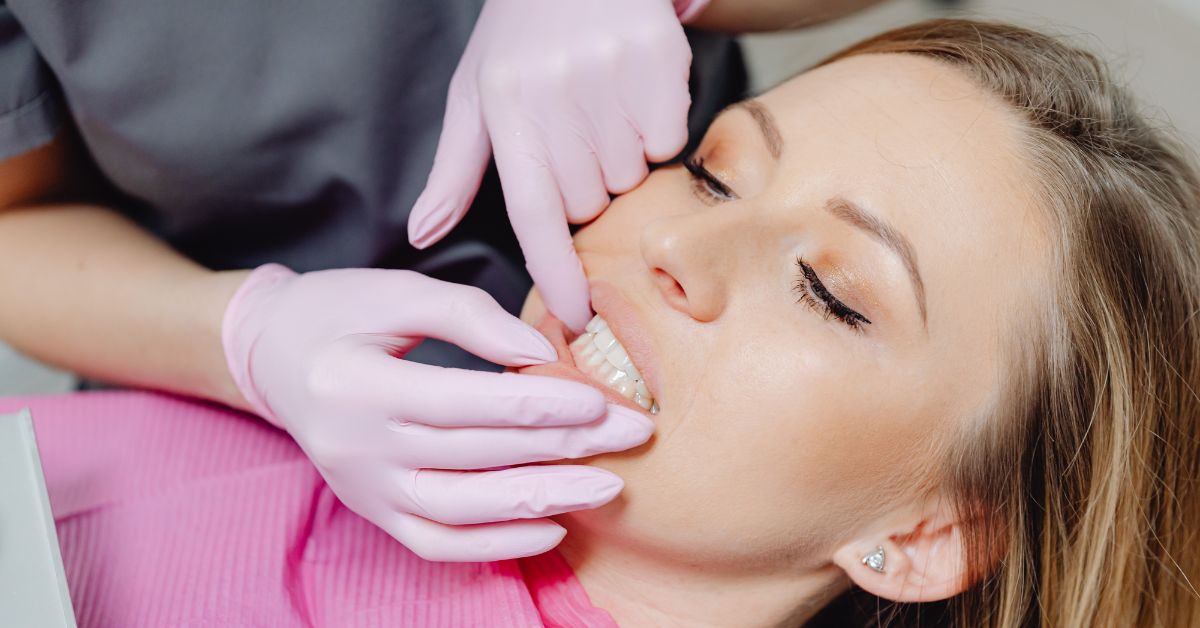
Structural factors often drive the recommendation for wisdom teeth removal, even when pain or visible symptoms are minimal. Dentists evaluate how third molars interact with available jaw space, surrounding bone, and adjacent teeth to determine whether continued eruption or retention creates ongoing risk. Wisdom teeth removal in Lynwood is frequently advised when anatomical conditions indicate that these teeth cannot integrate safely into the existing dental structure. This assessment focuses on physical constraints rather than discomfort levels. Structural incompatibility is treated as a long-term concern.
These structural conditions tend to worsen over time rather than remain static. Changes in root development, bone density, and eruption direction can increase pressure on nearby teeth or create areas that are difficult to clean effectively. PHD Dental considers how these factors are likely to progress rather than evaluating wisdom teeth as a snapshot in time. When anatomy suggests escalating risk, removal becomes a proactive decision. Planning emphasizes preventing future complications rather than responding to late-stage damage.
Limited jaw space is one of the most common structural reasons wisdom teeth fail to erupt properly. When there is not enough room for third molars to align vertically, they may press against adjacent teeth or remain partially trapped in bone or gum tissue. Dentists assess arch length, tooth spacing, and eruption trajectory to determine whether adequate space exists. Insufficient space often leads to impaction or misalignment. Structural crowding increases the likelihood of future problems.
How Dentists Measure Available Eruption Space
Dentists use imaging and clinical examination to evaluate how much room exists behind the second molars. Jaw length and tooth size are compared to predict whether an eruption can occur safely. These measurements help anticipate crowding before it becomes destructive. Space analysis informs removal decisions.
Why Crowded Eruption Creates Ongoing Risk
Crowded wisdom teeth can exert pressure that shifts neighboring teeth over time. This pressure may compromise alignment or contribute to enamel wear. Crowding also creates areas that are difficult to clean. Long-term risk increases as space limitations persist.
Wisdom teeth that grow at an angle rather than vertically often collide with adjacent molars or remain trapped beneath the gum line. These growth patterns are determined early and rarely correct themselves without intervention. Dentists evaluate the angle of eruption to determine whether the tooth can clear surrounding structures. Angled growth frequently leads to partial eruption or impaction. Structural interference makes removal more likely.
How Imaging Reveals Growth Orientation
X-rays and advanced imaging show the direction in which wisdom teeth are developing. Dentists assess whether the crown is angled toward neighboring teeth or bone. Orientation helps predict future contact and pressure points. Growth direction guides treatment planning.
Why Angled Teeth Rarely Become Harmless
Teeth growing horizontally or diagonally continue to push against surrounding structures. This pressure can damage adjacent roots or trap bacteria under the gum. Natural correction is uncommon once roots develop. Risk increases as growth continues.
Wisdom teeth positioned too close to neighboring molars can compromise the health of both teeth. Limited separation increases the risk of decay, bone loss, or periodontal problems where cleaning access is restricted. Dentists evaluate how close wisdom teeth sit to adjacent roots and bone structures. Close proximity often creates shared problem areas. Structural overlap raises concern.
How Dentists Assess Risk to Neighboring Teeth
Imaging allows dentists to see whether wisdom teeth contact or overlap adjacent molar roots. Bone levels and gum attachment are evaluated for early changes. These findings indicate whether neighboring teeth are at risk. Proximity assessment supports early intervention.
Why Shared Structures Increase Long-Term Damage
When teeth share tight spaces, plaque and bacteria accumulate more easily. Bone and gum tissue may deteriorate where access is limited. Damage often progresses quietly until advanced. Removing the wisdom tooth can protect adjacent structures.
Why Wisdom Teeth Removal in Lynwood Is Sometimes Recommended Before Symptoms Appear
Wisdom teeth do not need to cause pain or swelling to create meaningful long-term risk within the mouth. Dentists often recommend wisdom teeth removal in Lynwood after identifying conditions that are likely to worsen quietly as roots develop and surrounding structures change. Third molars can remain asymptomatic while still contributing to decay, bone loss, or pressure against adjacent teeth that is not immediately noticeable. Decisions are based on how these teeth are expected to behave over time rather than how they feel on a given day. Early recommendation reflects risk projection, not urgency.
Recommending wisdom teeth removal in Lynwood before symptoms appear also accounts for how surgical complexity and healing response can change with age. Teeth that are easier to remove earlier may become more difficult once roots fully form or bone density increases. Dentists consider whether delaying intervention increases the likelihood of complications, longer recovery, or damage to neighboring teeth. Preventive removal is discussed when long-term risk outweighs the benefit of continued monitoring. The emphasis remains on protecting future oral health.
Wisdom teeth can remain trapped beneath gum tissue or bone without producing obvious discomfort. These impacted teeth may still apply pressure to adjacent molars or compromise bone health in ways that are not visible during routine brushing or flossing. Dentists evaluate imaging to identify whether impacted wisdom teeth are positioned in a way that creates ongoing structural stress. Lack of symptoms does not eliminate mechanical impact. Hidden impaction often justifies early removal.
How Dentists Identify Risk Without Pain Signals
Imaging allows dentists to assess tooth orientation, root development, and proximity to critical structures. Subtle changes in bone or spacing can indicate increasing stress. These findings often appear before discomfort develops. Risk identification relies on anatomy rather than symptoms.
Why Waiting for Pain Can Increase Damage
Pain often emerges only after infection or structural compromise has progressed. By the time symptoms appear, adjacent teeth or bone may already be affected. Early intervention can prevent irreversible changes. Delayed action increases complexity.
Wisdom teeth that partially erupt or sit deep in the jaw often create areas that are difficult to clean effectively. Food debris and bacteria can accumulate in these spaces without causing immediate symptoms. Dentists recognize that decay or gum disease can progress quietly in these regions. Wisdom teeth removal in Lynwood may be recommended when hygiene limitations pose predictable long-term risk. Silent decay is a common reason for preventive removal.
How Dentists Assess Cleanability Around Wisdom Teeth
Dentists evaluate how accessible the area around wisdom teeth is for routine oral hygiene. Deep pockets or partially covered teeth limit effective cleaning. These conditions are assessed during examinations and imaging review. Poor access increases disease risk.
Why Decay Near Wisdom Teeth Often Goes Unnoticed
Decay in hard-to-see areas may not cause sensitivity until advanced stages. Neighboring molars can also be affected before symptoms develop. Regular brushing cannot always compensate for limited access. Preventive removal reduces this hidden risk.
Wisdom tooth roots continue to grow and anchor more firmly into the jaw as time passes. This progression can increase surgical difficulty and recovery demands if removal is delayed. Dentists consider root maturity when recommending wisdom teeth removal in Lynwood. Early removal may involve less bone disruption and smoother healing. Timing decisions account for developmental trajectory.
How Root Formation Influences Surgical Planning
Imaging reveals how developed roots are and how close they lie to nerves or bone structures. Less mature roots often allow simpler extraction. Advanced development increases complexity. Root assessment informs timing recommendations.
Why Early Intervention Can Simplify Recovery
Removing wisdom teeth before roots fully mature can reduce surgical trauma. Healing may be more predictable in younger bone. Early intervention can shorten recovery time. Planning considers these advantages.
How Dentists Determine the Right Timing for Wisdom Teeth Removal in Lynwood
Determining the right timing for wisdom teeth removal requires evaluating how third molars are developing in relation to jaw anatomy, surrounding bone, and adjacent teeth rather than reacting only to discomfort. Dentists assess whether current conditions suggest that risk will remain stable or increase as roots mature and bone density changes. Wisdom teeth removal in Lynwood is often recommended when timing supports easier surgical access, more predictable healing, and reduced long-term impact on neighboring structures. Decisions are individualized and based on projected progression rather than age alone. Timing is treated as a strategic factor in long-term oral health.
This evaluation also weighs the consequences of delaying removal against the benefits of continued monitoring. As wisdom teeth continue to develop, extraction may involve greater bone involvement and longer recovery periods. Dentists consider whether postponing removal increases the likelihood of complications affecting adjacent teeth or supporting bone. Wisdom teeth removal in Lynwood is advised when preventive benefit outweighs the risks of waiting. The objective is to intervene when conditions favor safer and more controlled outcomes.
The stage of root development significantly influences how complex wisdom teeth removal may become over time. Dentists evaluate whether roots are partially formed, fully developed, or positioned near critical anatomical structures. Less developed roots may allow removal with less disruption to surrounding bone and tissue. Root maturity is therefore a central factor in timing decisions. Surgical access often becomes more challenging as roots elongate.
How Dentists Evaluate Root Formation Using Imaging
Imaging allows dentists to assess root length, curvature, and proximity to nerves or bone structures. Early-stage roots are typically shorter and less firmly anchored. Advanced root development may increase resistance during extraction. These findings help dentists anticipate surgical complexity.
Why Earlier Root Stages Can Favor Easier Removal
Removing wisdom teeth before roots fully mature can limit the amount of bone that must be altered. Less invasive removal often supports smoother healing and reduced postoperative discomfort. Dentists consider these advantages when recommending timing. Early intervention may simplify recovery in appropriate cases.
Bone density evolves gradually with age, affecting how the jaw responds to surgical intervention and healing. Dentists evaluate whether current bone conditions are likely to support predictable recovery compared to later stages. Increased bone density can require greater force during extraction and may prolong healing. Healing potential is therefore an important timing consideration. Bone characteristics influence surgical planning.
How Bone Density Shapes Recovery Expectations
Denser bone may resist extraction and increase postoperative inflammation. Healing responses can vary as bone remodels differently over time. Dentists assess whether current density favors more predictable healing. These observations guide timing recommendations.
Why Healing Capacity Influences Removal Decisions
More predictable healing reduces the likelihood of prolonged discomfort or complications. Dentists aim to recommend removal when recovery expectations are more favorable. Healing capacity is weighed alongside surgical access. Timing decisions reflect this balance.
Monitoring wisdom teeth may be appropriate when positioning and surrounding tissues remain stable. Dentists track whether eruption patterns, hygiene access, and periodontal conditions show signs of change over time. Escalation occurs when imaging or examination reveals increasing pressure, decay risk, or inflammation. Wisdom teeth removal in Lynwood is recommended when observation no longer adequately protects oral health. Timing shifts as risk evolves.
How Dentists Recognize When Monitoring Is No Longer Adequate
Progressive changes in imaging, repeated inflammation, or reduced cleanability indicate rising risk. Dentists compare findings across visits to identify trends rather than isolated events. These patterns signal when intervention becomes advisable. Monitoring thresholds are defined carefully.
Why Delaying Intervention Can Increase Long-Term Consequences
Allowing risk to progress can compromise adjacent teeth and supporting bone. Surgical complexity may increase as conditions worsen. Dentists account for these potential outcomes when advising timing. Earlier action can prevent broader impact.
How PhD Dental Determines When Wisdom Teeth Stop Being Low-Risk
PhD Dental approaches wisdom teeth evaluation by identifying the point at which retained third molars transition from being clinically manageable to presenting escalating long-term risk. This determination is not based on pain alone, since wisdom teeth can remain asymptomatic while still contributing to structural strain, hygiene limitations, or progressive damage to surrounding tissues. Wisdom teeth removal in Lynwood is discussed when clinical findings suggest that continued observation no longer offers meaningful protection. The focus remains on recognizing change over time rather than reacting to isolated symptoms. Low-risk status is reassessed continuously as anatomy and conditions evolve.
This approach reflects an emphasis on prevention informed by evidence rather than routine removal or indefinite monitoring. PhD Dental evaluates how multiple risk factors interact, including eruption behavior, bone response, and proximity to adjacent teeth. When those factors begin to align in ways that increase future complication likelihood, the classification of risk changes. Wisdom teeth removal in Lynwood is recommended once the balance shifts away from safe retention. Decisions are grounded in projected outcomes rather than assumptions.
PhD Dental monitors subtle anatomical changes that indicate increasing strain around wisdom teeth before overt problems develop. Dentists evaluate whether pressure against neighboring molars is increasing, whether bone levels show early compromise, or whether eruption patterns are becoming less favorable. These indicators often emerge gradually rather than suddenly. Structural risk is identified through comparison over time. Early recognition allows intervention before damage accelerates.
How Dentists Track Progressive Changes Across Visits
Dentists compare imaging and clinical findings from multiple examinations to detect trends rather than relying on single snapshots. Small shifts in position, bone contour, or tissue response can signal escalation. Consistent documentation supports accurate risk assessment. Longitudinal tracking informs decisions.
Why Incremental Changes Matter More Than Sudden Symptoms
Gradual progression often causes more cumulative damage than acute episodes. Waiting for pain may allow irreversible changes to occur. Early indicators provide an opportunity to act preventively. Risk assessment prioritizes trajectory over immediacy.
Wisdom teeth that become increasingly difficult to clean may shift from low-risk to high-risk even without discomfort. PhD Dental evaluates whether access for brushing and flossing remains adequate as eruption or crowding progresses. Areas that trap bacteria increase susceptibility to decay and gum disease over time. Hygiene limitations are treated as a significant risk factor. Disease susceptibility influences risk classification.
How Dentists Assess Long-Term Cleanability
Dentists examine gum contours, pocket depth, and tooth position to determine whether effective cleaning is realistic. Imaging helps reveal areas hidden from routine hygiene. These assessments are revisited as conditions change. Cleanability plays a central role in risk evaluation.
Why Poor Access Leads to Silent Progression
Disease can advance quietly in areas that cannot be cleaned thoroughly. Symptoms may appear only after damage has occurred. Recognizing limited access early helps prevent progression. Risk increases when hygiene cannot be maintained.
Root formation changes how wisdom teeth interact with surrounding bone and nerves. PhD Dental evaluates whether continued root development increases the likelihood of surgical complexity or adjacent tooth impact. As roots mature, extraction may become more invasive and recovery less predictable. Root progression is factored into risk reassessment. Timing decisions account for these changes.
How Dentists Monitor Root Maturity Using Imaging
Imaging allows dentists to observe root length, curvature, and proximity to critical structures. Changes in root development are tracked across visits. These findings inform projections about future difficulty. Root monitoring supports proactive planning.
Why Advancing Root Development Shifts Risk Classification
More developed roots anchor teeth more firmly within the jaw. Increased anchorage raises the potential for bone disruption during later removal. Early intervention may reduce these challenges. Risk classification adapts as roots mature.
Contact PhD Dental to Learn About Our Wisdom Teeth Removal in Lynwood Today
Wisdom teeth decisions are rarely clear cut, especially when underlying risk may be changing slowly over time. A consultation creates the opportunity to review imaging, eruption patterns, hygiene access, and projected development so wisdom teeth removal in Lynwood can be considered within the context of future oral health rather than immediate symptoms alone. PhD Dental uses this discussion to explain how low-risk situations are identified, how risk evolves as conditions change, and when preventive action becomes the protective choice.
This visit also allows for an open conversation about timing, recovery expectations, and how removal or continued monitoring may affect your teeth and future dental care options. Dentists explain what factors are watched over time and why recommendations may shift even in the absence of pain. Patients leave with clarity around why a recommendation is made and what the long-term implications may be. Thoughtful evaluation supports decisions that feel informed rather than rushed. Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation and discuss whether wisdom teeth removal in Lynwood is appropriate based on your anatomy, development stage, and long-term oral health priorities.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
