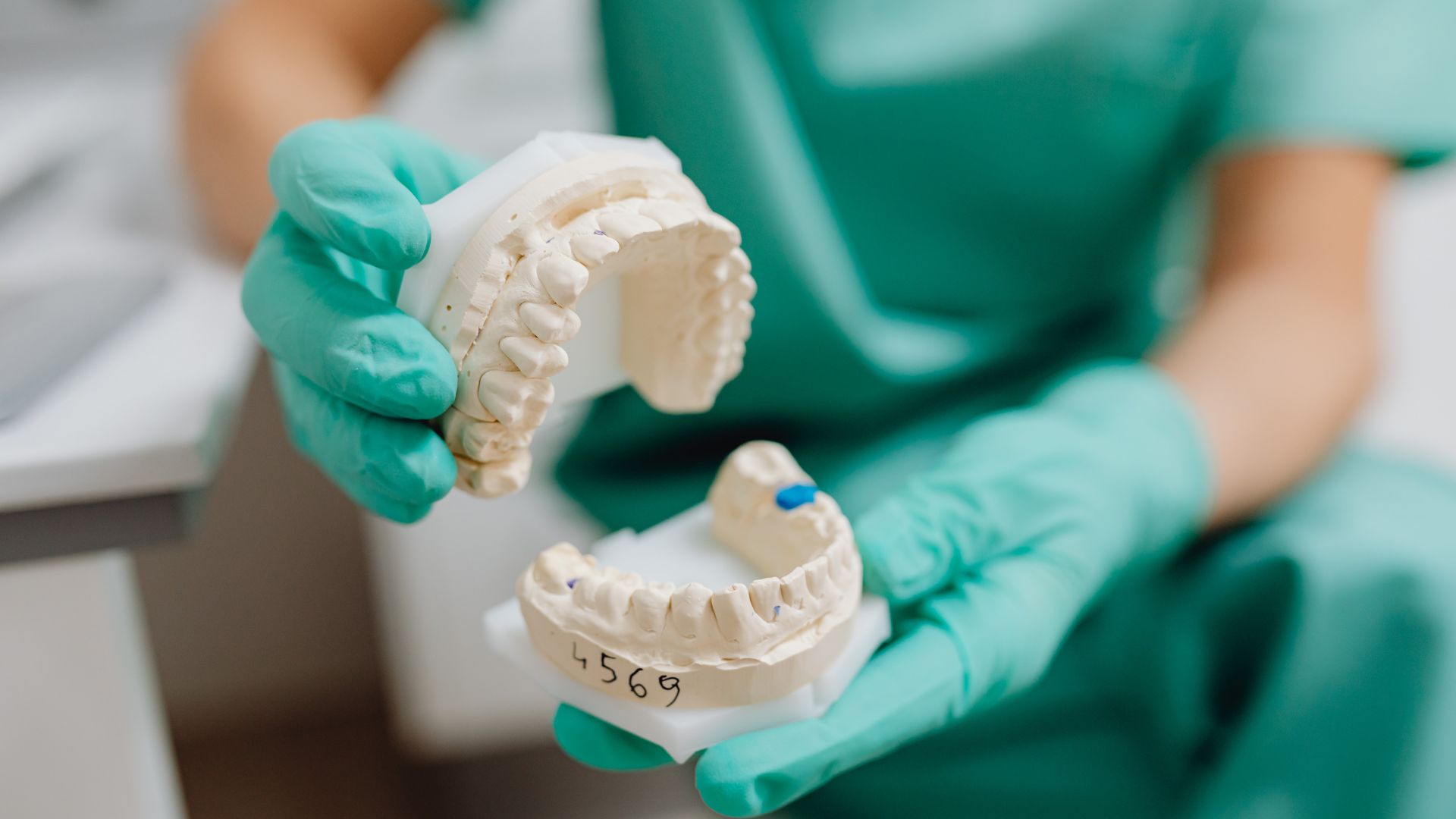
All-on-X Dental Implants in Pico Rivera
Living with widespread tooth loss changes how eating, speaking, and facial balance feel on a daily basis. All-on-X dental implants in Pico Rivera offer a fixed full-arch solution that anchors a complete set of teeth to strategically placed implants. This approach allows PhD Dental to address bone density limitations, long-term stability, and restorative goals.
Choosing All-on-X dental implants in Pico Rivera involves more than replacing missing teeth, since treatment decisions affect jaw health and how the restoration integrates with facial structure over time. PhD Dental approaches this treatment with digital planning, surgical precision, and restorative design that reflects how full-arch implant care functions in real daily use rather than theoretical outcomes. If you want to discuss whether All-on-X dental implants in Pico Rivera fit your health history and long-term goals, Call PhD Dental at (323)269-5437 or visit our contact page to schedule a focused consultation with our team.
Top-Rated Dentists
in Los Angeles
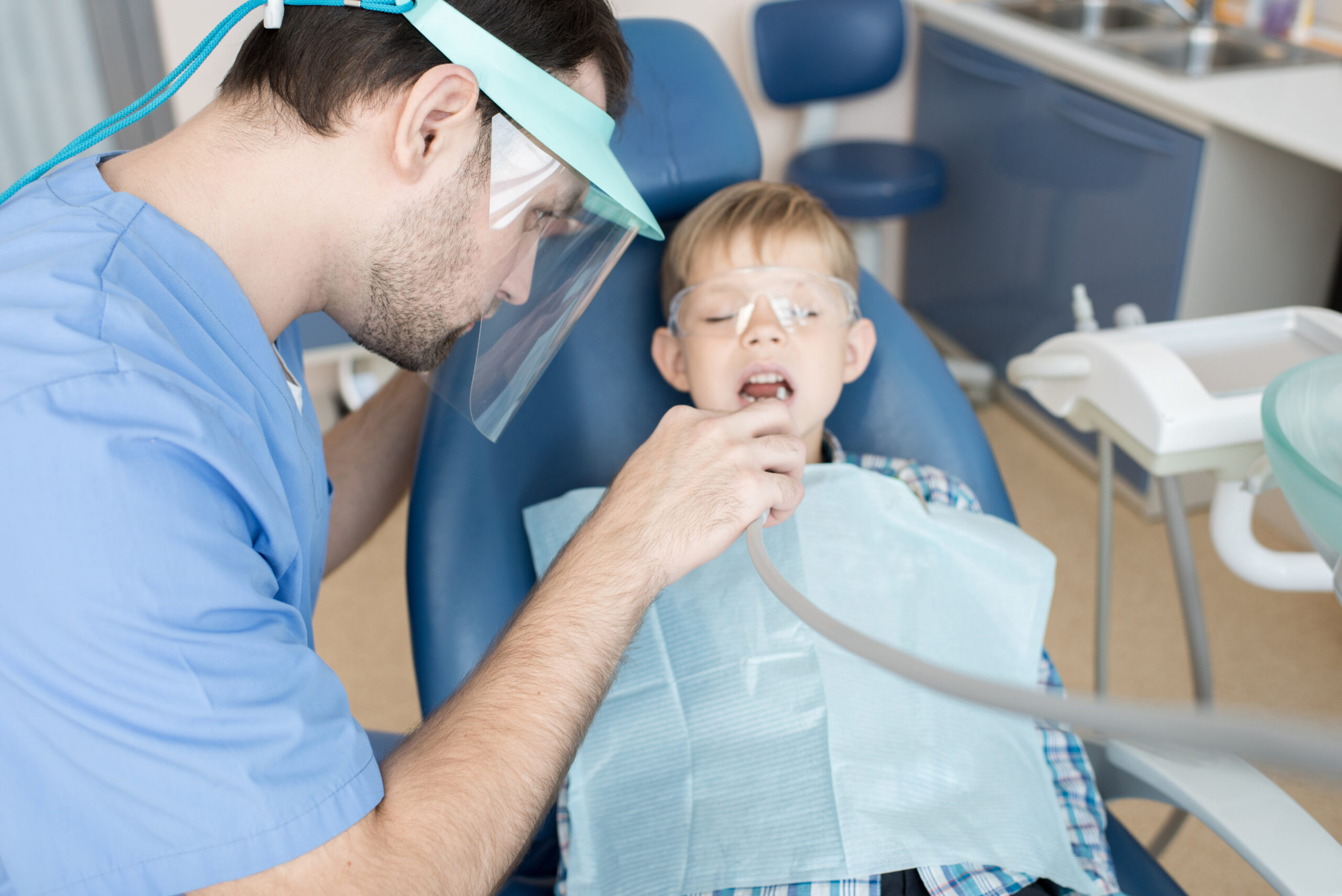
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
Table of Contents
- Who Qualifies for All-on-X Dental Implants in Pico Rivera
- How All-on-X Dental Implants in Pico Rivera Are Planned
- What the All-on-X Procedure Involves From Surgery Through Stabilization
- What Sets PhD Dental Apart in Full-Arch Implant Treatment
- Call PhD Dental Today to Get Help With All-on-X Dental Implants in Pico Rivera
Who Qualifies for All-on-X Dental Implants in Pico Rivera
Qualification for All-on-X dental implants in Pico Rivera depends on whether the mouth can support a full-arch restoration that transfers functional force into the jawbone through a limited number of implants rather than across the gums. This evaluation focuses on how bone volume, bone density, and anatomical structure interact under daily chewing forces rather than relying on surface-level indicators like tooth loss alone. PhD Dental assesses whether existing bone can accept strategically angled implants that stabilize a fixed prosthetic without requiring uniform bone height across the entire arch. The goal is determining whether the underlying structures can support long-term mechanical demands rather than simply whether implants can be placed.
Candidacy for All-on-X dental implants in Pico Rivera also requires evaluating how oral health history, healing capacity, and functional expectations intersect over time. Some patients qualify because their anatomy allows immediate stabilization, while others require sequencing or preparatory treatment to create predictable conditions. PhD Dental approaches qualification as a system-based decision rather than a checklist, examining how multiple variables combine during real daily use. This approach avoids overstating eligibility while still identifying patients who can benefit from full-arch implant stability.
All-on-X dental implants in Pico Rivera rely on existing jawbone to anchor a full arch using fewer implants that share functional load across the entire restoration. Dentists evaluate whether bone volume exists in strategic regions of the jaw, particularly in anterior areas where bone density is often higher and more resistant to resorption. Rather than requiring uniform bone throughout the arch, this approach depends on targeted support zones that can reliably absorb chewing forces. Structural assessment centers on whether these zones can sustain long-term stress without progressive breakdown.
How Implant Angulation Allows Use of Available Bone
Angled implant placement enables dentists to engage denser bone while avoiding anatomical limitations such as sinus cavities or nerve pathways. This technique changes how force enters the jaw by redirecting load into regions better suited for long-term support. All-on-X dental implants depend on precise angulation to maximize contact between implant surfaces and stable bone. Accurate planning determines whether this strategy can provide durable fixation.
Why Bone Distribution Matters More Than Uniform Bone Height
Uniform bone height across the entire arch is not required for All-on-X treatment when strategic support zones are present. Dentists focus on where bone can reliably accept force rather than how evenly bone is distributed. Concentrating support in stronger regions allows the restoration to function as a single stabilized unit.
Healthy gum tissue is essential for All-on-X dental implants in Pico Rivera because soft tissue forms the protective interface between the oral environment and underlying bone. Dentists assess whether inflammation, infection, or recession could interfere with healing or allow bacterial migration around implant components. Uncontrolled periodontal conditions can undermine bone stability even when implant placement is technically sound. Addressing gum health establishes a biological environment capable of supporting long-term implant integration.
Treating Periodontal Conditions Before Implant Surgery
Active periodontal disease introduces chronic inflammation that disrupts bone remodeling and soft tissue attachment. Dentists evaluate whether infection control, deep cleaning, or removal of compromised teeth is necessary before proceeding with All-on-X dental implants. Stabilizing gum conditions reduces postoperative complications and protects surrounding bone structures. Treatment sequencing is guided by biological readiness rather than procedural convenience.
How Soft Tissue Integrity Influences Long-Term Implant Protection
Soft tissue acts as a barrier that limits bacterial access to deeper structures surrounding implants. When tissue remains stable and well adapted, it protects the bone implant interface from inflammatory breakdown. All-on-X dental implants rely on this protective seal to maintain bone levels over time.
All-on-X dental implants in Pico Rivera require predictable healing across multiple implant sites, making systemic health an important part of candidacy evaluation. Dentists review medical conditions that influence bone metabolism, immune response, and circulation because these factors affect integration timelines and stability. Conditions such as diabetes or autoimmune disorders can alter healing dynamics even when oral anatomy appears favorable. Evaluating systemic health allows treatment planning to align with biological reality rather than idealized assumptions.
How Medical History Influences Implant Integration Timing
Certain medications and chronic conditions affect how quickly bone remodels around implant surfaces. Dentists assess dosage history, duration of use, and current stability when determining surgical timing. All-on-X dental implants may require modified sequencing to accommodate slower or variable healing responses. Integration planning reflects the body’s capacity rather than a fixed schedule.
Why Healing Predictability Matters in Full-Arch Implant Treatment
Full-arch restorations depend on multiple implants integrating as a coordinated system. Uneven or delayed healing at one site can affect load distribution across the entire prosthetic. Predictable healing reduces mechanical imbalance during early function. Stability emerges from consistency across all implant sites.
How All-on-X Dental Implants in Pico Rivera Are Planned
Planning All-on-X dental implants in Pico Rivera begins long before surgery and focuses on designing a full-arch solution that functions predictably under daily chewing forces rather than relying on generic implant formulas. The planning process integrates bone analysis, bite dynamics, and prosthetic design so implant placement and restoration work as a single coordinated system. PhD Dental approaches planning as a structural exercise, evaluating how forces will travel through implants, bone, and the final prosthesis during real-world use. This level of planning reduces reliance on adjustments later by aligning surgical decisions with restorative outcomes from the start.
All-on-X dental implants in Pico Rivera require a planning process that accounts for both immediate stability and long-term performance under repeated functional load. Decisions about implant number, angulation, and prosthetic materials are made together rather than sequentially to avoid mechanical mismatch. PhD Dental uses this integrated approach to ensure the final restoration aligns with jaw movement, speech patterns, and hygiene access. Planning prioritizes durability and consistency rather than speed or convenience.
Planning All-on-X dental implants relies on advanced imaging to understand bone volume, density distribution, and anatomical boundaries within the jaw. Cone beam scans allow dentists to visualize bone structure three-dimensionally, identifying areas capable of supporting angled implants without compromising nerves or sinus spaces. This structural mapping informs where implants can achieve stable engagement rather than where placement appears convenient. Imaging data becomes the foundation for every subsequent planning decision.
How Digital Scans Guide Implant Positioning Decisions
Digital scans provide precise measurements that allow dentists to plan implant placement relative to bone contours and load-bearing zones. These scans reveal variations in density that influence how implants will integrate and respond to force. All-on-X dental implants depend on using this information to position implants where long-term stability is most likely. Accurate scan interpretation reduces reliance on intraoperative adjustments.
Why Three-Dimensional Planning Improves Predictability
Three-dimensional planning allows dentists to anticipate how implants and restorations interact before surgery begins. Visualizing spatial relationships reduces uncertainty during placement and limits guesswork. Predictability improves when implant trajectories are mapped against anatomical constraints. Planning accuracy supports stable long-term outcomes.
Bite analysis plays a central role when planning All-on-X dental implants in Pico Rivera because chewing forces determine how implants and restorations will be stressed over time. Dentists evaluate how the upper and lower arches meet during function, including lateral movement and pressure concentration points. This assessment identifies areas where force must be distributed carefully to avoid overloading individual implants. Functional analysis ensures the restoration supports natural movement patterns.
Evaluating Chewing Patterns and Force Direction
Dentists study how force travels through the jaw during routine chewing and habitual movements such as clenching. Directional forces influence implant angulation and spacing decisions. All-on-X dental implants are planned to distribute these forces across the arch rather than allowing localized stress. Force evaluation guides structural design choices.
How Load Distribution Shapes Implant Configuration
Even force distribution reduces mechanical fatigue on individual implants over time. Dentists adjust placement and prosthetic design to prevent concentration of pressure. Balanced load sharing supports sustained stability during daily use. Configuration decisions reflect functional demand.
Prosthetic design is planned simultaneously with implant placement for All-on-X dental implants to ensure structural compatibility. Dentists evaluate how the final restoration will connect to implants, transmit force, and allow for hygiene access. Material selection and contour design influence weight, rigidity, and stress transfer throughout the system. Integrating prosthetic considerations early prevents misalignment between surgery and restoration.
Coordinating Implant Placement With Final Restoration Design
Implant positioning is adjusted based on where restorative components require support. Dentists plan attachment points to align with prosthetic geometry and bite contact areas. All-on-X dental implants rely on this coordination to prevent leverage issues. Surgical precision supports restorative accuracy.
Why Early Prosthetic Planning Prevents Structural Compromise
When prosthetic needs are considered late, implants may experience unfavorable stress patterns. Early planning allows dentists to design around mechanical limits. Structural compromise is avoided by aligning design and placement. Integration protects long-term performance.
What the All-on-X Procedure Involves From Surgery Through Stabilization
The full-arch implant procedure follows a structured sequence designed to create immediate structural control while protecting bone and soft tissue during early healing. Surgical planning translates into coordinated steps that address tooth removal, implant placement, and temporary stabilization without treating any phase as independent from the others. PhD Dental approaches this procedure as a continuous mechanical process where each action influences how force is introduced and managed during recovery. The objective centers on establishing controlled stability early rather than waiting for function to emerge gradually.
Stabilization during the procedure depends on precision timing and alignment rather than speed or aggressive loading. Each step accounts for how bone responds immediately after placement and how the provisional restoration limits unwanted movement during healing. PhD Dental evaluates how temporary components manage force while tissues adapt around the implants. This structured progression supports consistency during the most vulnerable phase of treatment.
When remaining teeth require removal, dentists coordinate extractions to preserve surrounding bone and soft tissue contours needed for implant stability. Site preparation focuses on shaping implant channels with controlled depth and angulation rather than removing excess bone unnecessarily. This approach limits trauma while creating precise contact surfaces for implant engagement. Preparation decisions directly affect how implants achieve early fixation.
How Extraction Timing Influences Implant Stability
Immediate or staged extraction decisions influence bone preservation and soft tissue response. Dentists evaluate whether removing teeth and placing implants during the same appointment supports predictable fixation. Coordinated timing can reduce structural collapse within the socket walls. Stability depends on minimizing uncontrolled tissue change.
Why Conservative Bone Handling Matters During Preparation
Bone responds best when manipulation remains limited and deliberate. Excessive removal can weaken surrounding support structures unnecessarily. Dentists preserve bone to maintain engagement surface area. Conservative handling supports early mechanical control.
Implant placement focuses on achieving mechanical engagement strong enough to resist micromovement during early healing. Dentists adjust angulation and depth based on bone density patterns identified during planning. Initial fixation allows implants to remain stable before biological integration occurs. Placement accuracy directly affects early load tolerance.
Achieving Stability Without Overloading Bone
Dentists apply controlled torque to seat implants securely without compressing bone excessively. Overloading bone can impair blood supply and compromise healing. Balanced fixation supports mechanical stability while protecting biological response. Precision governs placement force.
Why Multiple Implants Share Early Mechanical Demand
Using several implants distributes stress rather than concentrating force at a single site. Shared demand limits overload during chewing and speaking. Dentists design placement to balance force pathways. Distribution supports system-wide stability.
A temporary restoration attaches shortly after placement to control movement and guide functional behavior. Dentists design provisional components to limit bite force while allowing speech and appearance normalization. Early stabilization reduces soft tissue irritation caused by uncontrolled motion. The provisional phase shapes healing conditions.
How Temporary Prosthetics Control Functional Stress
Temporary restorations restrict contact points to reduce force magnitude. Dentists adjust contours to guide chewing patterns conservatively. Controlled stress protects implants during integration. Design choices manage early load exposure.
Why Early Movement Management Influences Integration
Micromovement beyond tolerance levels interferes with bone attachment. Stabilization limits displacement during daily activity. Dentists prioritize rigidity without excessive force. Integration benefits from controlled conditions.
What Sets PhD Dental Apart in Full-Arch Implant Treatment
Full-arch implant treatment requires coordination across diagnosis, surgical execution, and restorative design, and PhD Dental approaches this care as a unified system rather than disconnected clinical steps. Every recommendation is shaped by how anatomy, force distribution, and long-term maintenance interact once the restoration enters daily functional use. This perspective prioritizes mechanical reality and biological response instead of default protocols or accelerated timelines. Treatment planning emphasizes accountability over promises and durability over appearance alone.
PhD Dental differentiates full-arch implant care by defining performance boundaries and proportional treatment decisions before surgery begins. Each plan reflects how much structural support is necessary, how chewing forces will be managed long term, and how ongoing care will realistically be maintained. This method avoids unnecessary expansion while preserving functional reliability. Patients receive explanations grounded in structure, behavior, and longevity rather than generalized outcome language.
PhD Dental evaluates full-arch implant treatment as an interconnected system where placement, prosthetic design, and functional behavior are planned simultaneously. Each component is assessed according to how it influences the others once chewing, speaking, and hygiene occur daily. This approach prevents surgical success from creating restorative limitations later. Planning remains integrated rather than sequential.
How Integrated Planning Reduces Mechanical Mismatch
When surgical and restorative planning occur together, implant positioning aligns with prosthetic geometry and bite dynamics. This coordination limits leverage forces that emerge when components are designed independently. Dentists adjust placement decisions based on final restorative requirements. Mechanical compatibility improves through unified planning.
Why Isolated Planning Increases Long-Term Risk
Separating surgical and restorative decisions introduces unpredictable stress pathways over time. Misalignment between implants and prosthetics alters force distribution gradually rather than immediately. These issues often emerge after healing has completed. System-based planning reduces delayed mechanical risk.
PhD Dental avoids expanding treatment beyond what daily functional demand requires, even when anatomy could support more invasive solutions. Implant number, size, and placement reflect how much force the restoration must manage during routine activity. This proportional approach limits unnecessary biological disruption. Treatment scale matches actual functional need.
Matching Structural Capacity to Daily Use Patterns
Dentists analyze chewing behavior, bite force intensity, and contact patterns to estimate long-term demand. These factors guide how much structural support is necessary across the arch. Oversizing capacity can increase surgical impact without improving function. Proportional support improves biological tolerance.
Why More Intervention Does Not Equal Better Performance
Additional implants or larger components increase surgical complexity and healing demands. Greater intervention can affect recovery behavior and long-term maintenance requirements. Performance depends on alignment with demand rather than maximum construction. Restraint supports reliability.
PhD Dental frames full-arch implant treatment around long-term responsibility rather than short-term placement success alone. Maintenance expectations, monitoring schedules, and performance limits are discussed before treatment decisions are finalized. This transparency allows informed consent grounded in realistic care commitments. Longevity depends on sustained oversight.
How Monitoring Strategy Shapes Implant Longevity
Regular evaluation identifies subtle changes in tissue response and load tolerance over time. Dentists adjust care recommendations as conditions evolve rather than remaining static. Monitoring transforms implant care into an active process. Early response limits gradual deterioration.
Why Clear Expectations Protect Outcomes
Undefined expectations often lead to misuse or inconsistent maintenance behavior. Clear boundaries guide daily habits and follow-up compliance. Patients understand how actions influence structural performance. Defined expectations support long-term stability.
Call PhD Dental Today to Get Help With All-on-X Dental Implants in Pico Rivera
Deciding whether full-arch implant treatment is appropriate requires more than understanding the procedure itself. A consultation with PhD Dental focuses on how your jaw structure, bite behavior, and oral health history interact under daily functional use rather than relying on generalized assumptions. This discussion centers on if a fixed full-arch solution can perform predictably.
During your visit, the clinical team reviews diagnostic findings, explains how stability is achieved and maintained, and outlines what ongoing care would involve after treatment. This approach allows you to move forward with confidence grounded in understanding rather than uncertainty. If you are considering All-on-X dental implants in Pico Rivera and want a detailed evaluation, Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation focused on long-term performance and realistic outcomes.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
