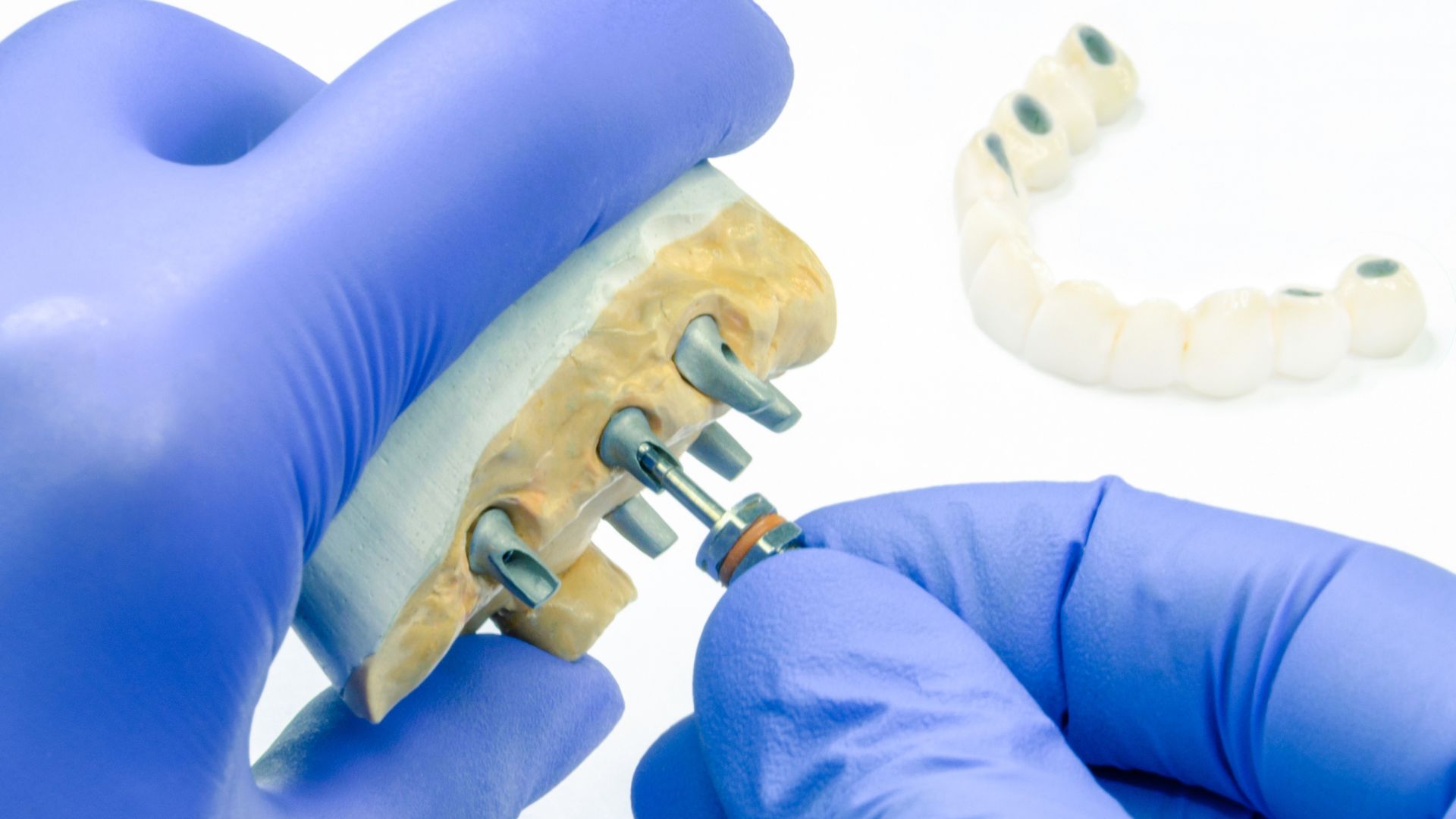
Endosteal Implants in Pico Rivera
Replacing a missing tooth requires more than filling visible space, since the jawbone must absorb chewing forces in a way that remains stable over years of use. Endosteal implants in Pico Rivera are placed directly into the jawbone, allowing restorations to function through bone-supported anchorage rather than surface-level support. This implant type relies on sufficient bone volume and density to achieve integration that withstands daily mechanical demand. PhD Dental evaluates this treatment by examining how bone structure, bite forces, and restorative goals interact once the implant becomes part of routine oral function.
Implant shape, placement depth, and alignment influence how forces travel through bone and how tissues respond during healing. PhD Dental approaches this process by planning around long-term performance rather than focusing only on surgical placement success. Each recommendation reflects how the implant will behave after restoration during chewing, speaking, and ongoing maintenance. If you want to discuss if endosteal implants in Pico Rivera are appropriate for your oral health needs, Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation focused on long-term stability and realistic treatment planning.
Top-Rated Dentists
in Los Angeles
Patient-First Dentistry for Every Stage of Life
From early childhood development to adult care, we focus on patient comfort and comprehensive treatment.

Removing Barriers to Dental Care
We believe everyone deserves access to high-quality dental care, regardless of financial situation.

Comprehensive Dentistry Under One Roof
Orthodontics, implants, oral surgery, and preventative care all conveniently located in our clinics.
Expertise, Access & Convenient Locations
Multiple clinic locations across Los Angeles with extended hours to fit your busy schedule.
How Jaw Anatomy Influences Implant Placement Decisions
Jaw anatomy plays a defining role in determining how and where implants can be placed, since bone shape, density, and internal structures directly affect stability under functional load. For endosteal implants in Pico Rivera, placement decisions are guided by how the jawbone accepts internal anchorage rather than surface-level support, which requires careful evaluation of depth, width, and structural continuity. PhD Dental analyzes jaw anatomy as a three-dimensional system, focusing on how bone responds to drilling, insertion, and long-term force transmission during daily use. This approach ensures implant placement aligns with biological limits rather than theoretical positioning.
Anatomical evaluation also considers how variations within the same jaw influence different placement strategies, since bone quality can change significantly from one region to another. Some areas provide dense cortical support, while others rely more heavily on cancellous bone that responds differently to stress. PhD Dental incorporates these variations into placement decisions so implants engage bone capable of sustaining repeated chewing forces over time. Anatomical planning prioritizes predictable performance rather than uniform placement patterns.
Bone density differs between the upper and lower jaw, influencing how implants achieve initial fixation and long-term integration. The lower jaw often presents denser bone that responds well to threaded implant designs, while the upper jaw may require adjustments in depth or angulation due to softer bone composition. Dentists evaluate these differences to determine how implants will interact with surrounding structures under load. Density assessment informs placement strategy rather than serving as a simple pass or fail metric.
How Density Affects Initial Implant Stability
Denser bone provides stronger resistance during implant insertion, which influences immediate mechanical stability. Softer bone requires careful preparation to avoid compression that could impair healing. Dentists adjust drilling protocols and implant selection based on density findings. Stability expectations are set according to how bone responds at placement.
Why Density Alone Does Not Determine Success
Bone density represents only one factor within a broader anatomical system. Even dense bone can fail under poor load distribution or misaligned placement. Dentists evaluate density alongside geometry and force direction. Long-term success depends on how these factors interact.
Jawbone width and height determine whether an implant can be placed without compromising surrounding structures or requiring excessive modification. Narrow ridges may limit implant diameter, while reduced vertical height affects how deeply implants can be seated. Dentists assess these dimensions to avoid encroaching on nerves, sinus spaces, or weakened bone regions. Dimensional analysis guides conservative yet stable placement decisions.
How Ridge Dimensions Influence Implant Selection
Implant diameter and length must correspond to available bone dimensions. Oversized implants increase the risk of structural compromise when space is limited. Dentists select implant designs that fit within anatomical boundaries while maintaining stability. Selection reflects measured dimensions rather than idealized sizing.
Why Preserving Native Bone Structure Matters
Excessive alteration of bone can weaken long-term support and complicate healing. Preserving the existing structure maintains natural load-bearing capacity. Dentists limit modification to what stability requires. Conservation supports predictable outcomes.
Implant placement must account for nearby anatomical features such as nerves, sinus cavities, and vascular channels that influence safe positioning. Dentists map these structures to establish placement boundaries that protect function and sensation. Avoiding these areas requires precise angulation and depth control. Anatomical awareness prevents complications that affect comfort and longevity.
How Imaging Identifies Safe Placement Zones
Advanced imaging reveals the exact location of internal structures relative to proposed implant sites. Dentists use this information to plan trajectories that maintain safe clearance. Imaging transforms placement from estimation to precision. Safety margins are defined before surgery begins.
Why Respecting Anatomical Boundaries Supports Longevity
Encroachment on anatomical structures can lead to chronic discomfort or functional impairment. Respecting boundaries preserves nerve health and sinus integrity. Long-term performance improves when placement remains within safe zones. Anatomical respect underpins durability.
How Bone Integration Shapes Implant Stability Over Time
Bone integration determines whether an implant becomes a stable, long-term part of the jaw or remains vulnerable to movement under repeated functional load. For endosteal implants in Pico Rivera, integration occurs when surrounding bone adapts to the implant surface and begins to transfer chewing forces through the jaw rather than around the implant site. PhD Dental evaluates integration as a gradual biological process influenced by bone quality, surgical precision, and how force is introduced during healing. Stability over time depends on how successfully this relationship develops beyond the initial placement phase.
The integration process continues well after surgery, since bone responds dynamically to stress, loading patterns, and oral habits over months and years. Even when early healing appears successful, long-term stability depends on whether bone maintains density and contact around the implant body. PhD Dental considers how daily function, maintenance behavior, and restoration design influence bone response over time. Implant performance is therefore evaluated as an evolving condition rather than a fixed outcome.
During the early healing phase, bone surrounding an implant begins reorganizing in response to surgical preparation and implant insertion. This response includes cellular activity that determines whether bone will form direct contact with the implant surface or retreat under stress. Dentists monitor this phase closely because excessive movement or loading can disrupt early attachment. Controlled conditions during healing influence the quality of long-term integration.
How Surgical Precision Influences Early Bone Attachment
Precise drilling and implant insertion preserve bone vitality and blood supply around the site. Excessive heat or compression during placement can damage bone cells responsible for integration. Dentists control technique variables to support healthy early response. Attachment quality reflects surgical discipline.
Why Early Stability Affects Long-Term Outcomes
Bone requires a stable environment to form durable contact with implant surfaces. Micromovement during early healing interferes with cellular attachment processes. Dentists limit early stress to protect integration. Stability during this phase shapes future performance.
Once healing progresses, bone continues adapting to the forces transmitted through the implant during chewing and speaking. This adaptation involves remodeling processes that either reinforce or weaken support depending on load consistency. Dentists evaluate whether forces remain within tolerable ranges that encourage bone maintenance. Long-term stability depends on balanced stress exposure.
How Repeated Force Influences Bone Density Over Time
Bone strengthens when exposed to consistent, moderate loading patterns. Irregular or excessive forces can trigger resorption rather than reinforcement. Dentists assess bite behavior to understand loading conditions. Density changes reflect functional patterns.
Why Load Distribution Matters More Than Force Magnitude
Even moderate forces can cause problems if concentrated unevenly. Proper distribution allows bone to respond uniformly around the implant. Dentists design restorations to spread stress effectively. Balanced loading supports sustained integration.
Several factors can gradually undermine integration even after initial success, including inflammation, poor hygiene, and uncontrolled bite forces. Bone loss around an implant often develops slowly without immediate symptoms. Dentists monitor these risk factors during follow-up evaluations. Early detection allows corrective intervention.
How Inflammation Affects Bone Stability Around Implants
Chronic inflammation alters bone metabolism and weakens structural support. Bacterial accumulation around implant components contributes to this process. Dentists emphasize tissue health to protect bone contact. Stability depends on inflammatory control.
Why Long-Term Monitoring Supports Implant Longevity
Subtle changes in bone level may not cause discomfort initially. Regular imaging and evaluation reveal trends before failure occurs. Dentists adjust care plans based on observed changes. Monitoring preserves long-term stability.
Maintenance Considerations for Endosteal Implants
Maintaining bone-anchored implants requires ongoing attention to how surrounding tissue, restoration components, and daily habits interact under repeated functional use. Endosteal implants function as internal structures within the jaw, which means maintenance focuses on preserving bone contact, managing soft tissue response, and monitoring mechanical wear rather than addressing surface-level irritation alone. PhD Dental frames maintenance as an active process that continues throughout the life of the implant rather than a passive expectation after placement. This perspective recognizes that long-term stability depends on consistent conditions rather than one-time success.
Care considerations for endosteal implants in Pico Rivera also involve understanding how small changes accumulate over time through chewing patterns, hygiene practices, and restorative aging. Bone response, tissue adaptation, and component integrity evolve gradually, which makes regular evaluation essential for identifying subtle shifts before they become structural concerns. PhD Dental integrates maintenance planning into treatment discussions so expectations remain realistic and actionable. This approach emphasizes prevention through observation and adjustment rather than reaction to complications.
Daily hygiene around implants focuses on maintaining clean interfaces between the restoration, gum tissue, and underlying bone. Plaque accumulation near implant components can trigger inflammatory responses that alter bone metabolism over time. Dentists evaluate whether hygiene routines effectively reach areas where bacteria tend to concentrate. Consistent cleaning supports tissue stability and bone preservation.
How Implant Geometry Influences Cleaning Access
Implant-supported restorations create contours that differ from natural tooth anatomy. These contours influence how easily brushes and floss reach critical contact areas. Dentists explain specific techniques based on restoration shape and attachment design. Access considerations guide personalized hygiene instruction.
Why Consistency Matters More Than Technique Perfection
Daily repetition maintains stable conditions even when technique varies slightly. Irregular hygiene allows bacterial buildup to persist long enough to affect tissue response. Dentists emphasize routine adherence over occasional thoroughness. Stability depends on sustained effort.
Professional monitoring tracks how bone and soft tissue respond to functional load over extended periods. Dentists use clinical exams and imaging to observe changes that are not visible or symptomatic early. These evaluations establish baseline trends that guide future recommendations. Monitoring transforms maintenance into an evidence-based process.
How Imaging Reveals Gradual Bone Changes
Radiographic imaging shows bone level patterns around implant surfaces over time. Small changes often appear before discomfort or mobility develops. Dentists compare sequential images to identify progression or stability. Imaging supports informed intervention timing.
Why Scheduled Visits Support Long-Term Planning
Regular visits create opportunities to reassess force distribution and tissue health. Dentists adjust guidance based on observed adaptation rather than assumptions. Skipped evaluations remove this feedback loop. Planning benefits from continuity.
Mechanical components experience wear as chewing forces pass through the restoration into the implant. Dentists assess how materials respond to stress and whether contact patterns remain balanced. Excessive wear can alter force pathways gradually. Maintenance includes monitoring these mechanical variables.
How Bite Changes Affect Implant Components
Natural changes in bite alignment occur as surrounding teeth shift or restorations age. These shifts influence how force contacts implant-supported restorations. Dentists evaluate contact points during follow-up visits. Adjustments maintain balanced stress distribution.
Why Early Adjustment Prevents Escalation
Minor imbalances can increase strain when left unaddressed. Early correction limits cumulative mechanical fatigue. Dentists intervene before wear affects bone support. Proactive care preserves performance.
How PhD Dental Evaluates Bone-Based Implant Stability
Evaluating implant stability requires more than confirming initial fixation, since long-term performance depends on how bone responds to sustained functional load over time. PhD Dental approaches bone-based implant stability as a dynamic condition shaped by anatomy, force transmission, and biological adaptation rather than a single surgical outcome. This evaluation framework examines how implants behave once healing transitions into everyday use involving chewing, speaking, and hygiene routines. Stability is assessed as an ongoing relationship between implant surfaces and surrounding bone rather than a static measurement.
PhD Dental also emphasizes evaluation methods that remain relevant years after placement, not only during early healing phases. Bone density patterns, tissue response, and mechanical stress pathways are reviewed together to understand how stability may change gradually. This approach allows early identification of risk patterns that might otherwise remain unnoticed. Evaluation focuses on long-term predictability rather than short-term confirmation.
Initial stability evaluation begins once biological integration has progressed beyond early healing and bone contact has matured. Dentists examine whether implants demonstrate consistent resistance to functional movement under normal bite forces. This assessment considers how surrounding bone supports the implant circumferentially rather than relying on isolated contact points. Baseline stability establishes a reference for future comparison. Early documentation provides context for interpreting subtle changes over time.
How Dentists Identify Meaningful Stability Indicators
Dentists analyze imaging data, tactile feedback, and functional response to assess stability quality. These indicators provide insight into how well bone has adapted around implant surfaces. Observations focus on consistency rather than absolute measurements. Stability indicators are interpreted within the context of overall jaw behavior. Multiple indicators are reviewed together to avoid relying on a single signal.
Why Baseline Data Guides Future Evaluations
Baseline records allow dentists to detect subtle changes that develop gradually over time. Without reference points, slow shifts in bone response can be difficult to recognize early. Comparative evaluation strengthens long-term oversight. Data continuity supports informed decision making. Historical records provide perspective when conditions evolve.
Bone continues adapting long after integration appears complete, responding to how force is applied during daily function. Dentists monitor whether loading patterns reinforce bone density or contribute to gradual resorption around implant sites. This monitoring considers both magnitude and direction of force. Stability depends on balanced adaptation. Long-term evaluation focuses on trends rather than isolated observations.
How Bite Behavior Influences Bone Support
Chewing patterns and parafunctional habits affect how stress enters the jaw through implants. Dentists evaluate whether forces remain evenly distributed across the restoration. Irregular loading can challenge bone tolerance over time. Behavior analysis informs stability evaluation. Bite behavior is reviewed alongside restoration design factors.
Why Adaptation Matters More Than Initial Strength
Strong early fixation does not guarantee sustained performance if adaptation trends become unfavorable. Bone may remodel negatively when stressed inconsistently. Dentists focus on how bone responds over months and years. Long-term trends outweigh initial impressions. Adaptation reflects real-world use conditions.
Gradual changes in bone or tissue often occur without discomfort, making proactive evaluation essential. Dentists look for subtle radiographic or functional indicators that suggest altered load tolerance. Early signs allow corrective action before structural compromise develops. Stability preservation depends on timely recognition. Monitoring prioritizes detection before symptoms appear.
How Imaging and Clinical Exams Reveal Subtle Shifts
Sequential imaging highlights small changes in bone level or density that single images cannot show. Clinical exams assess tissue behavior and mechanical response during function. Together, these tools provide a comprehensive picture. Early shifts become visible through comparison. Consistent imaging protocols improve accuracy.
Why Early Intervention Preserves Long-Term Performance
Addressing minor issues prevents escalation into larger structural problems. Adjustments made early require less intervention and protect bone integrity. Dentists act before symptoms arise. Preservation depends on proactive care. Early response supports sustained stability.
Call PhD Dental About Our Endosteal Implants in Pico Rivera Today
Choosing endosteal implant treatment requires a clear understanding of how bone structure, healing behavior, and long-term maintenance intersect once implants become part of daily oral function. A consultation at PhD Dental focuses on evaluating how your jawbone responds to implant placement, how chewing forces will be managed over time, and if long-term stability can be maintained under realistic conditions. This discussion centers on anatomy, mechanics, and durability rather than assumptions or generalized implant outcomes.
During your visit, the team reviews diagnostic imaging, explains how endosteal implants are evaluated for stability, and outlines what ongoing care and monitoring involve after placement. Expectations around maintenance and performance over time are addressed directly so decisions are grounded in clarity rather than uncertainty. This approach allows you to move forward with a treatment plan built around long-term oral health. If you are considering endosteal implants in Pico Rivera and want an individualized evaluation based on bone health and functional demands, Call PhD Dental at (323)269-5437 or visit our contact page to schedule a consultation focused on long-term implant stability and informed decision making.
Get in Touch with PhD Dental
Pick your location
Los Angeles
Los Angeles is a diverse and fast-moving city where access to dependable dental care is essential for individuals and families alike. PhD Dental serves patients throughout Los Angeles with a commitment to personalized care and long-term oral health.
Hours
- Mon 10:30AM - 7:30PM
- Tue 10:30AM - 7:30PM
- Wed 10:30AM - 7:30PM
- Thu 10:30AM - 7:30PM
- Fri 9:30AM - 7:30PM
- Sat 9:00AM - 3:00PM
- Sun Closed
